Keywords
GENERAL CONCEPTS
The use of animal models to study cardiovascular disease has substantially contributed to increasing our understanding of disease pathogenesis, leading to the development of diagnostic techniques as well as helping to verify the effectiveness of preventive and therapeutic procedures, whether pharmacological or interventional.1-8
Although animal models never completely resemble the clinical situation, they do make it possible to obtain direct information about specific events, offering good control over several variables while applying accurate, and typically invasive, procedures which are difficult to employ in clinical studies. The information obtained from animal models has to be assessed regarding its applicability to human pathology, and thus, information obtained in either context should be complementary.
Currently, animal experimentation is a legal requirement geared toward guaranteeing safety before introducing drugs and various diagnostic and therapeutic procedures into clinical practice. On the other hand, such experimental procedures are governed by a set of rules and regulations whose purpose is to avoid animals suffering during the development of experimental studies.9,10 It is compulsory to implement the means necessary to fulfill the established norms and approval procedures, and to monitor experimental protocols. To facilitate the development and acceptance of alternative methods of demonstrating specific pathophysiological or therapeutic hypotheses, the marketing of related techniques (eg, the in vitro production of substances based on animal models) and offering incentives for their use are measures that may help to develop conditions for experimenting with animal models.
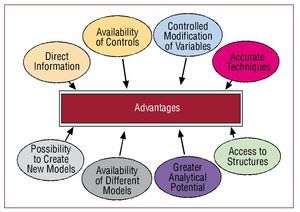
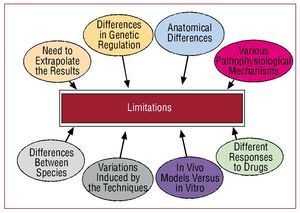
The main advantages of these types of models lie in the use of control groups and setting the conditions that could modify the results after varying one or more factors (Figure 1). Some of the limitations stem from the differences between human and experimentally induced disease, such as differences in genetic regulatory mechanisms or in factors that influence cardiovascular function1 (Figure 2). There may be important anatomical differences between phylogenetically distinct species, they may respond to different pathophysiological mechanisms, and pharmacological treatment may act in different ways. For these reasons, the extrapolation of basic research findings to human pathology should always be undertaken with caution.
Figure 1. Main advantages of animal models used in the study of cardiovascular disease.
Figure 2. Limitations of animal models used in research on cardiovascular disease.
On the other hand, the gap between the laboratory and clinical practice sometimes means that the usefulness of the results of a specific study is not immediately apparent. To decrease this gap, intermediate steps should be created to bring the results of a basic discovery nearer to daily practice with the aim of preventing, diagnosing, or treating cardiovascular disease. Basic research scientists also need to know about the concerns arising from clinical practice, unsolved problems, or observed limitations, in order to identify gaps and try to guide basic research efforts toward solving these problems. Science-based communication and discussion within multidisciplinary teams is essential to improving research findings that, in the final analysis, should be aimed at better disease control and promoting health in our society.
TYPES OF ANIMAL MODELS
The application of surgical procedures, controlled administration of drugs and compounds, selection of spontaneous genetic mutations and, more recently, genetic modification through recombination procedures have provided a large number of models with which to study cardiovascular disease. The anatomical and pathophysiological substrata may differ according to the animal species used, and different models can vary in their response to experimentally induced modifications.11
The appropriate selection of the experimental model should be based on the purpose of the study, that is, the model that is best suited to the research aims, although various factors may influence this decision, such as the techniques and methods required to obtain the information, their availability and accessibility, the conditions required to house the animals, the number of experiments, the type of study, acute or chronic, and in the latter case, its duration. Some of the models and preparations used in cardiovascular research are presented below.
Isolated Cells and Cell Cultures
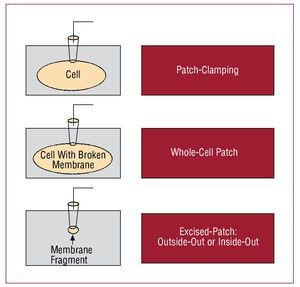
Different techniques are available to isolate cardiac myocytes from different animal species. At its simplest, the procedure consists in isolating the heart, perfusion with calcium-free enzyme solutions to degrade the collagen matrix connecting the myocytes, followed by cell extraction.4,12 Once cell viability is verified, various study techniques can be applied, eg, electrophysiological techniques, such as patch-clamping, to analyze ionic currents or changes in transmembrane voltage (Figure 3).
Figure 3. Diagram of the use of the patch-clamping technique in isolated cells with the intact membrane (upper part), after perforating the membrane (middle part), or using fragments of cellular membrane (lower part).
The development of cell culture techniques in combination with those of genetic engineering has increased the possibility of analyzing various events.5,13-17 Thus, transfection techniques, in which genetic material (recombinant DNA) is introduced into the nucleus of various mammalian cells, enable protein expression to be modified and, thus, cell functions. Studies which have used these techniques include those aimed at analyzing the behavior of the ionic channels involved in the kinetics of transmembrane action potential under basal conditions and under the action of various drugs.14-16
In other areas, such as regenerative medicine and tissue engineering, multiple lines of research are being developed with the aim of understanding and controlling the process of cellular differentiation. Among the possible uses are the development of tissue structures with potential clinical application.18
Tissue and Organ Bath Preparations
The study of specific structures from various animal species, such as papillary muscles, Purkinje fibers, myocardial tissue layers, or arterial and venous vessels, provides information in various fields that range from cardiac and vascular mechanics to electrophysiology.
Papillary muscle preparations obtained from small animals are based on extracting muscle and placing it in a chamber through which liquid nutrient flows at a constant temperature and that makes it possible to attach stimulation electrodes and force transducers to the ends of the muscle. Various mechanical properties can be studied in these preparations, such as the force-frequency relationship, responses to different types of overload and the mechanisms that regulate them, as well as the effects of various pharmacological or non-pharmacological manipulations.19,20 The use of microelectrodes or extracellular electrodes has enabled the study of the electrophysiological properties of myocytes and the analysis of drug effects,21 for example, their capacity to prolong repolarization at different frequencies.12 The use of these techniques in genetically modified models has increased our capacity to analyze the pathophysiological processes involved in various human diseases.
In addition, organ baths can be used to study myocardial layers, vascular rings, or various preparations that include the sinus node, the atrioventricular node or Purkinje fibers. Access to the elements constituting the preparation makes it possible to obtain relevant information on its behavior.22-24 One of the drawbacks of these tissue and organ preparations lies in the possible difficulties involved in the adequate dissemination to their deepest layers of oxygen, solutes or drugs and the substances under study.25,26 This limitation is not an issue when dealing with isolated myocyte preparations.12 The use of more complex experimental procedures can also be avoided,27 in which the part of the heart to be studied is isolated (eg, the right atrium with the sinus node or the papillary muscle with the interventricular septum) and irrigated with blood from the arterial system of another animal (cross circulation) or with liquid nutrient through the coronary arteries that replace the circulation to these tissues (eg, the sinus node artery or the anterior septal artery).
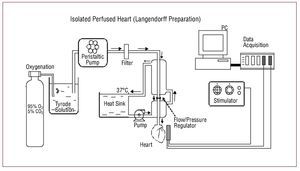
Langendorff System (Isolated Heart)The Langendorff method for studying isolated heart was described at the end of the 19th century. This method allows us to study events without neurohumoral interference, under controlled conditions, and with direct access to the areas of interest (Figure 4). Myocardial perfusion is done via the coronary arteries that are filled in a retrograde manner. In the classic preparation, the heart contracts without performing work, although variants exist (working heart) where, through various devices, the heart contracts under a specific load (liquid-filled intraventricular balloon, perfusion from the left atrium with the aorta connected to a system that regulates flow resistance, etc).2,28 Myocardial ischemia can occur after coronary artery ligation or by reducing liquid nutrient oxygenation. Hearts are used from different species, ranging from rat to large animals. After the heart has been extracted, the sectioned portion of the ascending aorta is cannulated and liquid nutrient supplied through this, via the sinuses of Valsalva to the coronary arteries, irrigating the myocardium and draining to the exterior through the cardiac venous system. The perfusion pressure (between 60 mm Hg and 80 mm Hg) or flow (between 1.5 mL/g and 2.5 mL/g) are kept constant and the liquid nutrient is oxygenated with a mixture of O2 (95%) and CO2 (5%). This liquid contains suitable proportions of electrolytes and glucose (Krebs-Henseleit solution, Tyrode solution, etc) and can be complemented with albumin or blood, especially when hearts from large species are used. The pH is kept between 7.35 and 7.4 and temperature is normally kept between 36oC and 37oC.
Figure 4. Diagram the Langendorff system used to study isolated perfused heart preparations from different animal species.
Multiple extracellular electrodes—both epicardial and endocardial or intramyocardial—can be used in the isolated perfused heart to conduct mapping studies of cardiac electrical activity and to analyze basic electrophysiological properties (refractoriness, conduction, automatism), their modification through the use of drugs, physical agents, electrical stimuli, or other procedures, as well as the mechanisms of onset, perpetuation or termination of cardiac arrhythmias29-33 (Figures 5-8). If the isolated heart is submerged in serum saline or in the liquid nutrient itself, the equivalent to electrocardiographic traces can be recorded and their variations analyzed under different maneuvers or drugs. The use of suction or pressure electrodes makes it possible to obtain the so-called monophasic action potentials which are related to the characteristics of transmembrane action potentials.34 The use of optical mapping systems based on recording changes in marker fluorescence associated with variations in membrane potential (Figure 9) has made it possible to approach the study of cardiac arrhythmias, providing additional information on the duration of action potential.35-37
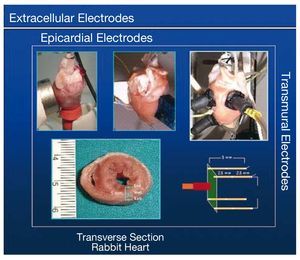
Figure 5. Various types of extracellular electrodes used to record myocardial activation processes in isolated perfused rabbit heart.
Figure 6. Devices used to conduct mapping studies of cardiac electrical activity by introducing thermal variations in isolated perfused rabbit heart.
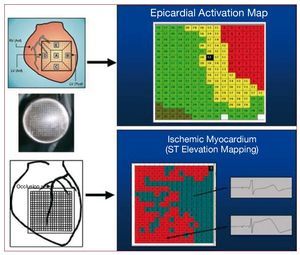
Figure 7. Upper part: activation map obtained with a multiple epicardial electrode, located on the anterior wall of the left ventricle in an isolated perfused rabbit heart preparation during epicardial stimulation. Lower part: identification of the ischemic area after coronary occlusion by analysis of ventricular repolarization modifications.
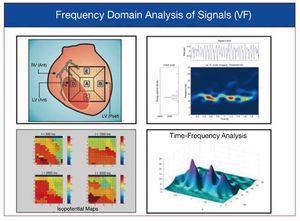
Figure 8. Frequency domain analysis (spectrum and time-frequency analysis) of the signals recorded during ventricular fibrillation in the left anterior ventricular wall. Isofrequency maps are shown at the lower left.
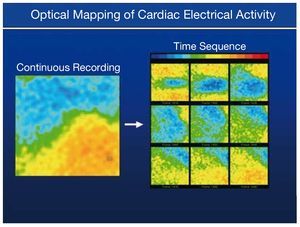
Figure 9. Images obtained using an optical mapping system during a ventricular fibrillation episode through recording changes in marker fluorescence in relation to variations in membrane potential.
Small Mammals
When choosing and using models based on small animals the particular characteristics of each species have to be taken into account; for example, collateral circulation is highly developed in the coronary tree of guinea pigs and hence ligation of one of the main branches would make it impossible to stably reproduce situations of myocardial ischemia. Among other advantages related to the use of these types of animals are their high reproduction rate (important when selecting cases with specific genetic characteristics within a suitable time-frame) and short mean lifespan, and thus the natural history of the disease can be analyzed within a brief period. On the other hand, genetic similarity to humans enables the study of specific alterations and their correspondence to diseases found in clinical practice, and this provides more information on the defects implicated in inherited diseases. Nevertheless, differences between the basic mechanisms that may restrict extrapolating the results have to be taken into account.1-4
In small mammals, several types of models have been developed of cardiovascular abnormalities that occur spontaneously or that are induced experimentally.3 The potential for research is increased by having a large number of animals available through selective breeding. Mouse models based on spontaneous genetic mutations and the development of strains with polygenic or monogenic mutations have facilitated the study of the mechanisms of various pathophysiological processes and their genetic determinants. On the other hand, in animals such as the mouse, technological advances have made it possible to create models with mutations in specific genomic loci. These procedures range from non-transgenic ones, based on induced mutations and the development of strains obtained from different types of embryos, to those of gene transfer, that were begun more than 25 years ago and that have given way to controlled induced mutation procedures with the expression of mutations associated with the development of a large number of diseases.3,5,7,38,39
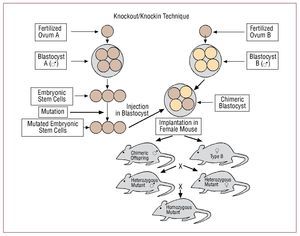
Transgenic models are based on introducing DNA into the genome of a specific animal, a fact made possible following the development of technology used in cell cultivation, manipulating embryos, and DNA recombination. Directly related techniques include pronuclear injection, viral transgenesis, and homologous recombination. Pronuclear injection involves the microinjection of DNA into the pronucleus of the zygote, and in viral transgenesis viral vectors are used to introduce genes such that they are expressed or alter the genome. Recombinant techniques are used to introduce a particular alteration into a specific site of the genome. In these cases, genetic mutation is obtained by specific genetic modification. Thus, in so-called knockout mice (genetic inactivation by homologous recombination), particular genes are inactivated to obtain information on their function, thus enabling the study of diseases created by mutations where there is a total or partial loss of protein formation through those which the gene expresses.3 On the other hand, in so-called knockin mice, specific genes are replaced or mutated, and their expression patterns are analyzed as well as the effects of these variations that involve a functional change.3,39
The procedure for creating these models is based primarily on the manipulation of embryonic stem cells. These are obtained from the inner cell mass of male blastocysts after egg fertilization and, once cultivated, specific mutations are created in vitro. These cells are pluripotent and are used to create mice with chosen mutations. Mutations are induced by introducing previously constructed genetic material into the embryonic cell. To this end, the electroporation procedure is used (via applying an electrical field), after which a small proportion of the cells undergoing the process incorporate the previously designed and constructed modifications. After multiplication of the embryonic cells carrying the mutation (heterozygous cells), these are injected into previously stored blastocysts which are later implanted in pseudopregnant female mice. Their chimeric offspring, which are derived from the modified embryonic cells and the donor blastocysts, are identified and after the heterozygous mice are crossbred, homozygous mutant mice are obtained (Figure 10).
Figure 10. Genetic modification procedures through specific gene inactivation, replacement or mutation. These are based on the manipulation of embryonic stem cells obtained from blastocysts and in which specific mutations are created by introducing previously constructed genetic material. After multiplying the embryonic cells carrying the mutation (heterozygous), they are injected into blastocysts that are later implanted in female mice. After the crossing the chimeric heterozygous offspring, homozygous mutant mice are obtained.
Lipid metabolism has been modified in transgenic rodent models to approach that of humans in order to produce models of atherosclerosis.40,41 Models of heart failure,42-44 several types of cardiomyopathies,7 and genetically-induced arrhythmias have been developed that enable the identification of forms of expression and the analysis of related genes.2,5-6,38,39 Thus, arrhythmic syndrome models are studied with characteristics common to those found in humans. For example, regarding atrial fibrillation, some of the transgenic models are characterized by the development of atrial fibrosis, or connexin 40 knockout models are created in which there are conduction abnormalities. Models have also been created in which the myocardial electrophysiologic properties are altered, with accelerated repolarization, such as occurs in those overexpressing Kir2.1 protein, altering the inward rectifying potassium current (IK1).6 Various models have been developed in relation to ischemic heart disease, including those used to study ischemic preconditioning and its relationship to connexin 43 and gap junctions.45,46
Larger Mammals
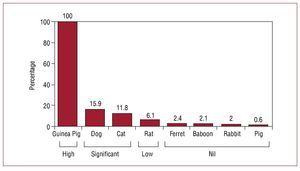
Large animals models are used in which it is important that regulatory and homeostatic mechanisms are present. Various aspects can hinder the interpretation of the results and these have to be taken into account when proposing and designing studies.2 Differences exist between species; for example, in the pig, the coronary circulation is characterized as terminal, without anastomoses between vascular branches, whereas in the canine model collateral circulation is present (Figure 11). Thus, coronary ligation in the pig resembles coronary occlusion in subjects without collateral circulation, but is unlike that of patients who have developed occlusion either spontaneously or in the context of chronic ischemic heart disease. On the other hand, there also are differences between species in the relative importance of the different branches of the coronary tree in relation to the size of the territory they irrigate. Regarding the cardiac conduction system, the distribution of the Purkinje fibers is not uniform; in the pig this is transmural, ranging from the endocardium to the epicardium,2
Figure 11. Characteristics of the collateral circulation in different animal species (adapted from: Maxwell MP, Hearse DJ, Yellon DM. Species variation in the coronary collateral circulation during regional myocardial ischaemia: a critical determinant of the rate of evolution and extent of myocardial infarction. Cardiovasc Res. 1987;21:737-46).
whereas in the dog or cat this is predominantly subendocardial, more closely resembling that of the human, thus presenting a more similar ventricular activation sequence. Differences exist between the myocardial repolarization process in canine models and humans, making it difficult to compare the changes occurring at the QT interval or T wave under different circumstances. Other differences between species stem from ion channel expression which regulates the characteristics of myocardial cell action potentials, since in some species, such as rats, the IKr channels are not expressed, whereas they are expressed in rabbits, guinea pigs, and dogs, and this fact aids in studying certain events such as arrhythmias associated with the prolongation of the QT interval.
Another aspect to take into account when using these experimental models is choice of the appropriate form of anesthesia, since its effects can modify the events studied.2 Pentobarbital effects the parasympathetic nervous system and influences the distribution of intramyocardial blood flow, whereas the combination of morphine with a-chloralose has less effect on autonomic control of the cardiovascular system, although it prolongs ventricular repolarization. Short-acting anesthetics can be of use in the initial stages of specific protocols where anesthesia is later maintained with other drugs. The anesthetic regimen can influence to what degree sedation is stable and some of their effects should be taken into account, such as depressed contractility or modifications in autonomic tone (pentobarbital, propofol). Certain inhaled anesthetics can modify the electrophysiological properties of myocardial cells and can have proarrhythmic effects (halothane, enflurane).
Chronic experiments range from those based on an acute intervention after which the effects produced by this in the presence or absence of specific drugs are observed (such as modifications in the degree of myocardial fibrosis after inducing atrial overload by valvular dysfunction) to those that require the use of special equipment to monitor the variables under study through different procedures, such as telemetry or cable transmission, and that, as a result, require the implantation of various systems (Table 1).
ANIMAL MODELS IN DIFFERENT AREAS OF CARDIOVASCULAR RESEARCH
Atherosclerosis
A large number of processes associated with atherosclerosis have been studied in animal models.40 Rabbits fed with cholesterol-rich diets have been studied to analyze lesion formation and progression, as well as lesion regression after the diet has been modified,47 or when specific treatments are added,48-51 and which have also been assessed in other animal species.52-56 In rodents, the application of transgenic techniques has enabled the creation of models with the lipid metabolism abnormalities present in humans,57 for example, through the manipulation of apolipoprotein E expression.58 In these mice, gene transfer using vectors that contain apoA-I cDNA to increase the concentration of high-density lipoprotein cholesterol (HDL-C) has led to lesion regression,59 and this has also been achieved by prolonging apolipoprotein E expression through the use of viral vectors.60,61 The transplantation of aortic segments that contain atherosclerotic lesions from transgenic mouse models with high apolipoprotein B levels, low HDL-C concentrations, and fed with hyperlipidemic diets to normal recipients has enabled the study of the processes involved in the plaque stabilization and regression.62,63 Phenomena such as thrombogenesis and platelet function have also been analyzed in animal models,64 where the use of purpose-built perfusion chambers65 has enabled the analysis of the mechanisms involved in thrombosis.
Ischemia-Reperfusion and Myocardial Infarction
Various lines of research in animal models have focused on analyzing the potential to limit the size of the infarction. Some decades ago, studies were conducted on drugs and substances that could slow down or prevent the development of necrosis,66,67 with limited and nonreplicable results.46 However, experimental models of coronary occlusion provided accurate data on the development of necrosis.68-73 After the relevance of the role reperfusion played in saving ischemic myocardium was recognized, its implication in lesion development also began to be analyzed. Pathological mechanisms associated with calcium overload, the action of oxygen free radicals, and the activity of inflammatory cells with the involvement of leukocytes, adhesion molecules, and cytokines, among other factors, have been identified in animal models.74 Mitochondrial damage has also been analyzed75 by identifying membrane abnormalities (pore formation) that make it permeable to various substances and ions and that determine cell death.
The inhibition of pore-opening may be associated with cardioprotection during ischemia-reperfusion.
Progress has also been made in the areas of ischemic preconditioning and postconditioning.76,77 Experimental protocols exist with interventions that replicably limit the size of the infarction due to preconditioning; for example, in canine models, this can be achieved by occluding the anterior descending coronary artery for several 5-min periods, separated by similar periods during which perfusion is reestablished, and after which prolonged occlusion is established. Postconditioning also reduces the size of the infarction; for example, by the application of several intermittent short-term periods of coronary occlusion (30 s) at the beginning of reperfusion following prolonged occlusion. Both phenomena have been studied in different animal species and the time course of the protective effect and molecular mechanisms involved have been analyzed, and which continue to be subjects of research.46,78-84
Cardiomyopathies
Dilated cardiomyopathy, which is characterized by ventricular dilatation and deterioration in systolic function, is one of the major causes of heart failure as well as being the most frequent cause. Among studies analyzing its pathogenesis are those focusing on familial forms, associated with genetic mechanisms, such as cardiac a-actin, the b-myosin heavy chain or troponin T, and that lead to various abnormalities.
Models have been developed in small animals, such as rats, mice, and hamsters in order to study its pathogenesis.7,42,85,86 In hamster strains with spontaneous dilated cardiomyopathy (BIO14.6, CHF 147) the steady development of rhabdomyolysis, hypertrophy, dilatation, and congestive heart failure has been described, with changes in enzymatic expression that lead to an increase in oxidative stress (TO-2 strain). In genetically modified models,42,86 dilated cardiomyopathies have been induced that include mutations in the genes that regulate the cytoskeleton (lack of genes for dystrophin and utrophin) and cause muscular dystrophy and cardiomyopathy. Muscle LIM protein knockout models have also been created that develop dilated cardiomyopathy. G protein overexpression leads to cardiomyopathies in which apoptosis mechanisms are involved. Mitochondrial mutations exist with deficits in oxidative phosphorylation occurring with dilated cardiomyopathies. In large animal models, closer to clinical practice, aspects associated with mechanics, molecular and metabolic abnormalities, and inappropriate neurohumoral adaptations have been analyzed.
Heart Failure
The analysis of the causes of heart failure, and the transfer of existing knowledge from experimental studies to clinical practice—both in the area of myocardial protection and ventricular remodeling—form another challenge that faces the researcher studying cardiovascular disease.
The development of heart failure involves both the heart and peripheral circulation and the complex neurohumoral mechanisms that regulate the hemodynamic processes. Small-animal strains exist in which heart failure has appeared due to spontaneous genetic alterations. Animals in which genetic modifications have been artificially induced are also used.43,44,86 Among the murine models where transgenic and knockout technology has been applied,43,44 are those which are characterized by abnormalities in calcium regulation and the development of hypertrophy.42,86 In these models, studies focus on the relationship between the expression of sarcoplasmic reticulum Ca2+ ATPase (SERCA) and the development of heart failure after its expression has been altered.
In larger animals, various procedures can be used to produce heart failure models, among which are rapid atrial or ventricular stimulation (3-4 times higher than spontaneous sinus rhythm),87 that within a period of 3-5 weeks causes heart failure with reduced systolic function, reduced cardiac output, increased systemic vascular resistance, increased systolic ventricular wall stress and electrophysiological and metabolic abnormalities. Various types of pressure or volume overload or myocardial ischemia are also used; for example, by provoking valvular failure leading to volume overload or by increasing ventricular ejection impedance leading to pressure overload. In addition to analyzing the factors that determine deterioration in ventricular function in these models, the response to various treatments are analyzed and various circulatory assistance techniques are assessed.
Arrhythmias
It is difficult to find models of arrhythmia that bring together all the determining anatomicopathological, electrophysiological, biochemical, and molecular factors that are present in clinical practice. Transgenic models are used to study the mechanisms involved in the genesis of several types of cardiac arrhythmias in the context of channelopathy and various types of cardiomyopathies.5,38,39 Animal models have contributed relevant information on the mechanisms of atrial fibrillation and various therapeutic procedures.6 There are several models of atrial fibrillation in different contexts which provide complementary information: vagal nerve stimulation or continuous perfusion with acetylcholine, persistent overstimulation, congestive heart failure, sterile pericarditis, atrial ischemia, mitral regurgitation, volume overload, respiratory failure, drug action (cesium to induce the formation of afterpotentials and abnormal automatisms, and aconitine to create ectopic foci) and transgenic models, among others.6
In the context of myocardial ischemia and reperfusion, various types of arrhythmias have been generated.46,88,89 Their analysis has contributed relevant information on sudden death, for example. One of the most frequently used animal models to study these events is the two-stage Harris model, where the anterior descending coronary artery is ligated with a hypodermic needle placed parallel to the artery. The needle is immediately removed to prevent complete occlusion, while producing a stenosis and a consequent reduction in flow; 30 min later the artery is completely occluded by a second ligature.2,90,91 This procedure—or those based on it that use ligatures to achieve a degree of obstruction controlled through the analysis of distal flow— prevents the immediate development of ventricular fibrillation due to ischemic preconditioning92 and thus various events produced by the myocardial ischemia, both mechanical and electrical, can be studied. These models have helped to determine the key role of abnormal automatism of partially depolarized Purkinje fibers during the onset of arrhythmias sustained during the first hours after coronary occlusion.89 It has also been observed that activity triggered by afterpotentials is a later event. Various models have been developed in order to better understand the events that occur in chronic ischemic heart disease.93 Simultaneous ischemia and physical exercise can help in understanding the mechanisms involved in the onset of arrhythmias in these situations, both without previous infarction and following infarction, as well as the factors that determine or facilitate their appearance or the possible beneficial effects of therapeutic intervention, such as those designed to prevent ventricular fibrillation and sudden death. Autonomic nervous system activity triggered by reflexes initiated by ischemia, hemodynamic changes produced by ischemia, or simultaneous exercise has been studied from various standpoints, including analyzing the intensity of the baroreceptor response that determines the probability of ventricular fibrillation occurring.93,94
The induction of specific arrhythmias can also be studied using programmed stimulation techniques. Other methods of inducing arrhythmias2 are based on the use of drugs or substances that facilitate the production of afterpotentials (catecholamines, digitalins),95 those that generate repetitive activity (ectopic foci, aconitine), or that simulate or promote the production of arrhythmias associated with prolonged QT intervals (torsades de pointes) (antiarrhythmic drugs with an inverse effect depending on frequency or other types). Clofilium, which blocks HERG channel conduction, or methoxamine, can cause torsades de pointes in rabbits in vivo. Veratridine in isolated perfused guinea pig heart2 or bradycardia induced by complete atrioventricular blockage in large animals—leading to dilatation and ventricular hypertrophy—are other models used to induce polymorphic tachycardias. Parameters that predict arrhythmias have been analyzed in these models, such as those related to QT interval variability and also the proarrhythmogenicity of specific drugs before their introduction into clinical practice.2
The concept of electrical and structural remodeling in atrial fibrillation has been based on experimental studies96-98 and has led to some therapeutic interventions being reassessed. Changes in refractoriness, conduction velocity, and the wavelength of the activation process associated with the development time of the arrhythmia have been studied in this arrhythmia,99 in addition to the ionic mechanisms involved, and changes associated with structural remodeling characterized by the development of fibrosis and conduction abnormalities. Various therapeutic approaches aimed at controlling atrial fibrillation have benefited from data obtained from animal models, including information on causal mechanisms and responses to pharmacological or surgical interventions or those based on radiofrequency ablation procedures.100-106 It has been verified that specific drugs stop arrhythmia without modifying the wavelength of the myocardial activation process.107
Controlling sudden death due to ventricular arrhythmias remains an unsolved problem and a challenge for researchers working in various disciplines. The clinical outcomes of the use of implantable automatic defibrillators are an example of progress in this field and experimental studies have contributed to their development.108
FUTURE DIRECTIONS
Progress in cardiovascular disease control is based on improved understanding of a range of highly varied issues, from those addressed in epidemiological studies, clinical trials, and registries to those studied within basic research projects. In this field, progress has been made in molecular analysis: the genetic determinants of a large number of processes, their interactions, transcription mechanisms or signaling pathways, have all provided new insights into understanding the development and functions of organs and systems.
The use of classic techniques, such as the Langendorff preparation, and variants where the heart undergoes controlled loading, as well as genetic modification procedures, have furthered the study of cardiac mechanics and contraction and relaxation processes. This has enabled analysis of the functional effects of abnormalities in the expression of proteins associated with sarcoplasmic reticulum, intracellular calcium regulation or elements of the cardiac contractile apparatus.109 In vivo determinations in murine models with genetic abnormalities that produce hypertrophy contribute information on the factors that determine systolic and diastolic function and on the pharmacological interventions that modify them. The use of these models requires adapting the recording systems to the characteristics of small transgenic animals.
The introduction of non-invasive techniques, such as echocardiography, with high-resolution transducers (high-emission power and better temporal resolution to adapt it to the high heart rate in these animals), has made it possible to obtain more information on anatomy and cardiac function and study the results of pressure and volume overloads in transgenic models, and thus analyze the factors associated with the development of hypertrophy or ventricular dilatation. The use of intracavitary catheters combined with ultrasound techniques has aided the analysis of pressure-volume curves.
More recently, cardiac magnetic resonance imaging has been introduced into experimental studies to obtain anatomical and functional information, which, together with ultrasound techniques can be applied in vivo. It also contributes information on perfusion and myocardial metabolism, the presence of myocardial necrosis, and on calcium regulation during the stimulation-contraction processes.110 Tools are being developed to study the mechanics of intramyocardial function and torsion. Metabolic analysis includes spectroscopic methods for detecting P31 or H1, establishing ratios such as that of phosphocreatinine and ATP, associated with energy production. It also enables the analysis of the basic mechanisms that influence cardiac function, ventricular remodeling processes, and postinfarction scar formation. The study of new agents which make the controlled analysis of the myocardium possible enables the assessment of various events such as myocardial cell apoptosis.
Positron emission tomography is being used in experimental models to analyze and quantify changes in glucose in the myocardium and to detect regional perfusion defects and, together with single-photon emission computerized tomography (SPECT), contributes molecular information through the use of markers that bind to specific targets.
In the area of cardiac electrophysiology, optical systems have been refined to the point of obtaining temporal resolutions comparable to those obtained with extracellular electrodes, thus extending the study of cardiac arrhythmias. This also involves progress in the development of microelectrode arrays capable of stimulating and recording bioelectrical signals with high temporal and spatial resolution, making it possible to accurately study the interactions and linkages between different types of cells and tissues, as well as to determine the effects of drugs on the characteristics of action potentials.111
This work was partly conducted with research grants from the Ministry of Health PI06/0758 (Project FCI) and RD06/0003/0010 (RETIC: REDINSCOR).
Correspondence: Dr. F.J. Chorro.
Servicio de Cardiología. Hospital Clínico Universitario.
Avda. Blasco Ibáñez, 17. 46010 Valencia. España.
E-mail: Francisco.J.Chorro@uv.es