Keywords
INTRODUCTION
Heart failure is the leading cause of hospitalization in individuals older than 65 years in Spain and the third cause of cardiovascular morbidity and mortality. The prevalence of this condition has risen sharply in the past few decades because of population aging, an increase in hypertension and diabetes mellitus, and the longer survival of patients with acute myocardial infarction.1
Various studies have shown a decrease in morbidity and mortality in heart failure with some beta-blockers (BB).2-4 The latest meta-analyses have concluded that BB treatment of 28 patients with acute systolic heart failure for 1 year prevents at least 1 death, with lower figures in the moderate and severe grades.5-7
Despite the evidence, however, BB use in clinical practice at the primary care level is low. This is seen in studies such as Euros-HF (The Euro Heart Failure Survey of the EUROHEART survey program)7 and IMPROVEMENT (The IMPROVEMENT of Heart Failure Programme),8 which show that BB prescription by family doctors is very low (only 6.2% in Euros-HF to 21% in IMPROVEMENT would use these drugs for heart failure and at lower doses than needed). The recent SHAPE (Study Group on Heart Failure Awareness and Perception in Europe)9 study conducted in 9 European countries did not find any improvement in this trend. In the studies cited, Spain ranked toward the bottom in terms of percentage of patients treated with BB.
This study was based on the hypothesis that primary health care physicians can use BB safely at the evidence-based recommended dose or the maximum tolerated dose in patients with stable acute systolic heart failure who meet the criteria for its indication. The study is similar to other studies in the literature, but the first in Spain in which uptitration was performed exclusively by primary health care physicians.
METHODS
Design
The study was designed as an open-label, prospective multicenter before/after intervention study. All patients were recruited between April 2004 and April 2006 at 2 urban health care centers in Barcelona (Sant Martí Nord and Sant Martí Sud), with an assigned population of 32 357 patients older than 18 years of age; 7 family physicians and 1 referral cardiologist took part in the study.
The following inclusion criteria were used: acute systolic heart failure (ejection fraction [EF] <45%), New York Heart Association (NYHA) functional class II/III, age 18 to 85 years, angiotensin-converting enzyme inhibitor (ACEI) treatment (or angiotensin-II receptor blockers II [ARBs] in case of intolerance), and previous BB therapy (at least 1 month before inclusion in the study). All patients signed the informed consent to participate in the study.
Patients were excluded in the case of hospitalization, surgery, or an episode of cardiovascular exacerbation or instability during the 3 months before the study or if they had signs or symptoms of overload (edema, rales, jugular vein enlargement, ascites, or pleural effusion). Patients were also excluded if they had asthma, severe chronic obstructive pulmonary disease, bronchospasm, second- or third-degree atrioventricular block without a pacemaker, a moderate to severe valve condition without surgical correction, active myocarditis, sick sinus syndrome, systolic blood pressure <80 mm Hg, or heart rate <50 bpm.
Sample size was calculated using the percentage of patients who continued to tolerate BB treatment at 6 months from the start of dose titration. Assuming a prevalence of 0.5% of grade II and III systolic heart failure based on previous studies with 89% treatment tolerance, the minimum sample size is 69 individuals plus 10% possible losses (76) for a=.05 and a capacity to detect differences >7.5%.
Sampling was performed using a systematic, consecutive approach. Patients who met the inclusion criteria were invited to participate regardless of whether they were seen by the primary care physician or the referral cardiologist.
The primary health care physicians taking part in the study received 4 hours of theoretical training on heart failure and practical workshops on BB dosing.
The prescribed BB (carvedilol or bisoprolol) was chosen by the physician who included the patient in the study, after consultation with the referral cardiologist. Dosing was initiated at minimum doses (1.25 mg/d bisoprolol in 1 dose or 6.25 mg/d carvedilol split into 2 doses) and was doubled every 2 weeks if no adverse events related to the drug occurred, until the recommended target dose or the maximum tolerated dose was reached.
The dosing protocol recommended that if a patient experienced any adverse events, the dose should not be increased or should be decreased according to the severity of the effect. In the case of 2 consecutive visits with the same adverse event that required not increasing or reducing the dose, the maximum tolerated dose was considered to have been reached and the dose was not uptitrated in subsequent visits. Treatment was withdrawn if the same adverse event persisted for 2 successive visits at the minimum BB dose or if side effects that contraindicated treatment appeared. As a last resort, the decision to discontinue or downtitrate the treatment was made by the physician who performed BB dosing of the patient.
A standardized case report form was used to record the results of the examination at each visit, as well as a systematic history of adverse events, additional tests, hospitalizations, prescribed dose, and discontinuation of treatment. The case report form was completed with appendices to standardize the examination and response to adverse events.
Interventions
Visit 0 (study inclusion visit): once the physician and cardiologist had agreed on BB prescription (through an interdepartmental consultation sheet, verbal consultation, or joint visit), the patient was asked for informed consent, the onset of disease was recorded, and a laboratory workup, ECG, and Doppler echocardiography were requested. Each subject received the patient information sheet for the study.
Visit 1: The inclusion and exclusion criteria were reassessed once the additional test results were available. Functional status was assessed according to the NYHA classification, a cardiac auscultation and general examination were performed, and the presence of ascites, edema, rales, or jugular vein enlargement was recorded. Blood pressure, heart rate (decubitus and standing), and weight were also measured. BB was started at minimum doses, and patients were instructed to phone or visit their physician if there were any adverse events or questions.
Visits 2 to 7: Every 2 weeks and at all visits up to and including week 12 from the start of treatment, the following were performed: a physical examination, assessment of NYHA functional class, heart rate, decubitus and standing blood pressure, weight, waist circumference, orthostatic hypotension, adherence to therapy (by tablet counting), drug tolerance and adverse events; the number of hospitalizations, emergency room visits or unscheduled cardiologist or family physician visits since the last visit was recorded. Increases in BB dose and decreases, discontinuation, or modification of the BB or other treatments related to heart failure were also recorded.
Visit 7 (week 17): In addition to the usual examination, the Doppler echocardiogram and laboratory workup were repeated.
Final visit (6 months after starting treatment): In addition to the activities included in the other visits, the post-treatment echocardiogram (EF) and laboratory workup were assessed.
If any patients failed to show up for a scheduled visit, the physician contacted them by phone to determine the reason and arrange another appointment.
Statistical Analysis
SPSS 10.0 was used for the statistical analysis, and P<.05 was the significance level for the 2-sided hypothesis test. Categorical qualitative variables were compared using the Pearson c2 test for separate groups or the McNemar test for paired data. The Yates and Fisher corrections were used when the expected frequencies were less than 5 and 3, respectively. Quantitative variables are expressed as the mean values (SD), after applying the Kolmogorov-Smirnov normality test. Mean values were compared using the Student t test for independent or paired samples or the respective nonparametric tests (Mann-Whitney U test for independent samples or Wilcoxon test for paired samples) for a non-normal distribution or qualitative variables measured in nominal scales. The results of the study were then compared to those obtained from other published studies, using the odds ratio (OR) and 95% confidence interval (CI).
RESULTS
Seven of the 22 physicians at the participating sites took part in the study up to 2002. A total of 88 patients were included, 57 treated with carvedilol and 31 with bisoprolol. Baseline characteristics of the patients are summarized in Table 1.
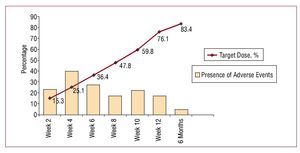
BB treatment was maintained in 85 (>96%) patients, and 75% of patients reached the recommended target dose (10 mg/d in 1 dose for bisoprolol or 50 mg/d in 2 doses for carvedilol). A mean of 83.46% (Figure 1) achieved the target dose.
Figure 1. Percentage of target dose attained at each visit and percentage of patients with adverse events at each visit.
The mean dose achieved in patients treated with bisoprolol was 9.6 mg, which accounted for 96.77% of the recommended target dose. In the case of carvedilol, the mean dose was 35.6 mg, or 76.2% of the recommended dose, with significant differences favoring bisoprolol (P=.02).
Treatment was discontinued in 3 patients. In all of them, discontinuation occurred during the first weeks of treatment: 1 for symptomatic bradycardia, 1 for stroke, and 1 for syncope. These 3 patients accounted for all hospitalizations and emergency room visits.
Regarding adverse drug-associated events, 62 (70.4%) patients experienced at least 1 adverse event during the study: 3 (3.4%) had adverse events that required BB withdrawal, 8 (9.1%), mild adverse events that required BB downtitration, and 51 (57.9%), mild adverse events that did not required BB downtitration. Of these, 12 (13.6%) required uptitration of the diuretic dose or a switch to a more potent diuretic, 5 (5.7%) required downtitration in the ACEI or ARB doses, and 34 (38.64%) experienced mild adverse events that required no change in treatment. Adverse events were not observed in 26 (29.6%) patients.
Adverse events occurred most often between weeks 2 and 4 (Figure 1). The most common were dizziness, asthenia, and shortness of breath (Table 2). Although there were no significant differences in overall side effects between the two BBs, asthenia and dizziness were significantly more common in the carvedilol group.
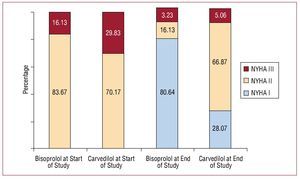
After 6 months of treatment, a significant improvement was observed in functional class, which dropped from a mean of 2.24 at the first visit to 1.56 at the last visit. Functional class improved in 69.3% of patients and worsened in only 3.4%. The improvement was significantly greater in the group treated with bisoprolol (Figure 2) (P<.01).
Figura. 2. Percentage of patients and functional class according to beta-blocker.
Among the other controlled variables, there was a significant increase in EF and weight, and significant decrease in heart rate and systolic and diastolic blood pressures. No significant differences were observed in the laboratory variables (Table 3).
On average, adherence to therapy (determined by tablet counting) was 95%, and more than 94% of patients presented adequate adherence at all visits.
Regarding the identification of baseline variables that could predict which patients were more unlikely to achieve the target dose, logistic regression analysis showed that only EF was an independent predictor that maximum doses would be achieved (patients with poorer EF were less likely to reach the target dose).
DISCUSSION
BB therapy in patients with acute systolic heart failure leads to a considerable reduction in morbidity and mortality; however, the usage levels of these drugs are far from desirable. Various studies have provided explanations for the low usage, including a lack of knowledge, lack of experience, lack of time and resources, and unwarranted concern about using BB.10 Although many clinical practice guidelines for heart failure currently recommend that BB dose titration be handled by specialized care units, recent meta-analyses show that BB are well tolerated when dosed carefully, even in cases of severe heart failure and in older patients.8
Even though BB dosing is not excessively problematic, close, frequent patient follow-up is recommended, particularly during the first few weeks. The family physician is accustomed to using BB for other conditions, such as ischemic heart disease, in which maximum coverage is achieved.
The present study (88 patients, no follow-up losses) shows that careful dose titration, predefined titration charts, and monitoring for side effects allow more than 95% of patients to continue treatment past 6 months and 75% to achieve the evidence-based recommended dose. Patients who do not achieve the target dose are maintained at doses between 25% and 75% of the recommended dose, an issue of huge importance because, although morbidity and mortality were reduced at maximum doses, additional substudies of CIBIS II (Cardiac Insufficiency Bisoprolol Study II) and US CARVEDILOL (U.S. Carvedilol Heart Failure Study Group)4,6 have shown that lower morbidity and mortality are also obtained at lower doses. Therefore, low-dose BBs are better than none.
If we compare this study with key published studies on BB tolerance in patients with heart failure (Table 4), statistically higher figures are obtained in terms of patients who reach the target dose and patients who maintain BB therapy. Withdrawal levels (3% in this study) were similar to those published in the meta-analysis of Ko et al,8 which reported withdrawal in 3.6% of patients who started treatment.
There are many reasons why this study achieved superior and statistically significant results than most in terms of tolerance and target dose achievement. Patients were initially recruited from primary care and were, in principle, more stable and in a better functional class than those treated in the hospital setting or heart failure units. The patients showed no signs of decompensation, edema, ascites, or rales at the start of dosing and had been stable for at least 3 months. In principle, the primary care physician would be able to initiate dosing among such patients. In all studies with which our study showed no significant differences— BISEX (Bisoprolol Experience Investigators),11 GESICA (Grupo de Estudio de la Sobrevida de la Insuficiencia Cardiaca en Argentina [Study Group for Heart Failure Survival in Argentina]),12 ENH (Experience Nurse Heart Failure)13—, dose titration was also performed using predefined charts for starting doses, dose increases, actions in case of adverse events, and clinical variables to be recorded at each visit, and all participating professionals attended preliminary training meetings on the subject. An Italian study by Maggioni et al,14 which included 3091 patients from 197 sites and used predefined treatment charts that included actions for side effects and were distributed among professionals, showed BB coverage increases from 25% to 58% and mean doses above 70% of the recommended target dose.
It is worth noting, however, that our study presented the highest percentage of patients with adverse events, despite having maximum percentages of tolerance. The explanation is simple, since systematic, standardized recording of all adverse events (even those not reported by the patient) on the case report form was performed at each visit. If we limit ourselves only to adverse events that led to changes or withdrawal of therapy, the number of patients affected would be around 32%, a figure more consistent with that of the other studies.
As in other published studies, adverse events occurred in the first few weeks of treatment, when early hemodynamic adaptation (significant reductions in heart rate and blood pressure such as those observed in this study) takes place. In these early weeks, monitoring should be close and able to resolve adverse events using treatment protocols that minimize treatment withdrawals. It should also be taken into account, as an explanation of the results for Figure 1, that adverse events decrease over time because patients selected for their good response to treatment during the first few weeks predominate by the end of follow-up.
In this study, a significant improvement was observed in the functional parameters, whether EF (mean increase, 12.5%) or functional class. A significant improvement was also seen in the functional class, from a mean of 2.24 at the first visit to 1.56 at the last; functional class improved in 69.3% of patients and worsened in only 3.4%. These data are also consistent with those obtained in most published studies: the GESICA14 study, for example, reported an improvement in baseline functional stage in 48% of patients, the CASA II (Carvedilol Safety Assessment II)15 study obtained an initial mean decrease in functional class from 2.2 to 1.8, and the BISEX13 study described a reduction from 2.4 to 1.8. Even the study reporting the poorest tolerance (Galatius et al16) found that patients able to tolerate BB had a significant improvement in functional class, although, as already mentioned repeatedly, patients sometimes experience a temporary deterioration in the first few weeks that is alleviated with appropriate measures. The improvement in functional class is usually attained before the final dose is reached. In this study, 59.1% of patients had achieved the functional class they presented at the end of the study by 6 weeks after the start of treatment, 64.8% by 8 weeks, 79.5% by 10 weeks, and 85.2% by 12 weeks.
Although the aim of the present study, based on its design and sample size, was not to compare carvedilol and bisoprolol, some differences were observed and obviously can only be used to suggest working hypotheses for future studies. For instance, patients treated with bisoprolol were more likely to achieve the maximum recommended dose, attain a higher mean dose, and have a statistically greater improvement in functional class. There were no differences in the percentage of adverse events, even though such events were more common in the first few weeks among patients treated with carvedilol, in whom asthenia and dizziness were also significantly more common. These differences could be explained by the lack of randomization. In fact, significant differences were seen in the patients' baseline characteristics: patients treated with carvedilol had an initially lower EF and systolic blood pressure, which could explain the poorer tolerance and higher incidence of adverse effects such as asthenia and dizziness.
In terms of limitations, the study was a prospective, observational study in which, owing to the characteristics of the primary endpoint, patients could not be randomized because the scientific evidence makes BB comparison to placebo inadmissible and unethical. This means that conclusions regarding secondary endpoints such as adverse events are not irrefutable even though they are virtually identical to the results of the main placebo-controlled studies and various meta-analyses. Some bias in the selection of more compliant patients by the physicians taking part in this study cannot be excluded. In addition, echocardiograms were not analyzed by a core laboratory, although each patient underwent the baseline and final echocardiography examinations at the same site. Lastly, participating doctors were highly motivated to achieve the expected results, an aspect which merely underscores the importance of motivation and dedication in achieving BB doses and beneficial effects in most patients.
CONCLUSIONS
Most BB-related adverse effects are mild, resolve with no need to change the treatment, and occur in the first few weeks. Only 3.4% of patients required withdrawal of treatment, and 75% of patients achieved the recommended target dose.
Based on the results of our study, the family physician, if adequately trained and motivated, can safely use BB in patients with stable heart failure, following consultation with the referral cardiologist.
ABBREVIATIONS
BB: beta-blockers
EF: ejection fraction
This study was the recipient of a grant for research training and doctoral dissertations from the Fundació Gol i Gorina (Institut Català de la Salut) for the principal investigator.
Correspondence: Dr. J.M. Verdú Rotellar.
Pl. de la Infància, s/n. Barcelona. España.
E-mail: verdujm@gmail.com
Received November 25, 2008.
Accepted for publication June 17, 2009.