Lesions located in an arterial bifurcation have traditionally been a challenge for percutaneous coronary intervention.1 At the time when balloon angioplasty was being used, these interventions were associated with increased risk of vascular occlusion, especially in the lateral branch, and also with a higher rate of restenosis. Suboptimal results in the main vessel, which sometimes had to be accepted for fear of losing the lateral branch, and the higher content of elastic fibers in these coronary segments seemed to explain these problems, at least partially. With the arrival of stents, treatment of bifurcations changed radically. After implanting a stent, we can “ensure” excellent immediate results in the main vessel and avoid problems arising from the delayed elastic recoil inherent to these lesions. However, the stent in the main vessel “cages” the lateral branch and may jeopardize the ostium due to displacement of the plaque or the carina itself.1 In turn, implanting a stent in the lateral branch is even more challenging. As can be seen in the Figure, implanting a stent in the lateral branch often entails significant technical problems that are compounded by the need to implant a stent in the main vessel. The fundamental problem arises in patients with major lateral branches, whose clinical outcome will depend on the results of the intervention.
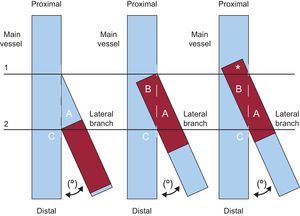
Schematic representation of a coronary bifurcation with angulation between branches (°) illustrating the problems arising from stent implantation in the most proximal portion of the lateral branch. The horizontal line 1 represents the initial exit (proximal) of the lateral branch, while the horizontal line 2 represents the location of the carina (C). In the left image, the stent (shown in red) fits the carina perfectly (horizontal line 2) without protruding into the main branch. The disadvantage of this approach is that any disease existing in the proximal part of the lateral branch (blue triangle A) will not be covered by the stent. In contrast, in the center image, the stent (in red) fits the origin of the lateral branch perfectly (horizontal line 1) and perfectly covers the entire proximal disease of this branch (red triangle A). The disadvantage of this strategy is that the medial part of this stent protrudes greatly over the main vessel (red triangle B). In routine clinical practice (right image), the most proximal part of the stent (*) can even be above the origin of the lateral branch (horizontal line 1). In these latter 2 situations, it is necessary to crush the entire medial and proximal part of the stent implanted in the lateral branch with another stent in the main vessel (not shown). Thus, the lateral branch ends up double-caged and, also, the area immediately proximal to the exit of the lateral branch has three metal layers (*) in the main vessel wall.
Bifurcation treatment outcome depends on many factors, among which we highlight the size of the vessels involved, the angle they form, whether the lateral branch ostium is affected, carina morphology and volume, and the distribution and characteristics of the atheromatous plaque determining luminal stenosis.1-4 Although many angiographic classifications have been proposed to categorize bifurcation lesions, until recently none had achieved universal acceptance because of their complexity and uncertain value in guiding the intervention. We must remember that the bifurcation itself complicates angiographic assessment of stenosis severity in the various arterial segments involved. Thus, despite using multiple projections, branch shortening and overlapping phenomena are common. In fact, bifurcations are a major source of variability in the SYNTAX (SYNergy between percutaneous coronary intervention with TAXus and cardiac surgery) score. Furthermore, the presence of bifurcations significantly penalizes the percutaneous coronary intervention results expected according to that scoring system. Undoubtedly, the most currently accepted classification internationally is that of Medina et al,3 first proposed in the pages of this journal 8 years ago. This classification is far better than all others, first, for its simplicity and logic, and second, because it describes graphically the fundamental anatomy of any bifurcation (ie, whether the main vessel before and after the branch, and finally the branch itself, are affected [1] or not [0]).3 While it is quite useful for guiding the percutaneous coronary intervention, we must remember that there is not a good relationship between an injury's angiographic appearance and the actual location of the atheromatous plaque. Only tomographic intracoronary imaging techniques can be used to visualize the presence and distribution of atheroma plaque with respect to the vascular lumen and the characteristics of the carina.5,6 Actually, a complete 3-dimensional reconstruction of the plaque and residual lumen is required to understand the complex anatomical substrate of each bifurcation. We also know that, in response to shear stress distribution generated by the flow splitter, imaging techniques more often demonstrate scant atheromatous effect at the carina, while plaque is characteristically located in the artery walls opposite the flow splitter.5,6 In addition, the morphology of the carina itself can help predict the consequences of its mechanical displacement. Finally, we have also learned that the histological composition of atherosclerotic plaques tend to be different in each location (again in relation to shear stress).6 In this regard, it has been suggested that tissue characterization techniques (either with virtual histology or with optical coherence tomography) may help guide bifurcation treatment.6
THERAPEUTIC STRATEGIESA decade ago, we had a proliferation of multiple strategies, more or less ingenious, that attempted to ensure a good end result in the main vessel and the lateral branch.1 With the “double stent” techniques, a good anatomical result is achieved in both vessels, even in the most complex bifurcations. However, these techniques are more laborious, and complex interventional techniques always end up paying the price of a higher rate of acute complications.1 Furthermore, sequential interventions with dilations at different levels, and ending the procedure with simultaneous end inflation of one balloon at each branch (kissing balloon) are usually required to ensure excellent results in both vessels. As we have seen so often in medicine, when multiple strategies are proposed but none of them prevails, we must conclude that we have not yet managed to solve the problem.1 In our case, apparently this is a “simple” mechanical issue. Or is it not so simple?
Considering the anatomy and the angle between the vessels, T- or V-type stent techniques have been used, in which stent overlap in the main vessel is minimal. In turn, the culotte, kissing-stent, and crush techniques (intentional crushing of the proximal portion of one of the stents) attempt to provide a satisfactory response to the challenge of covering the entire lesion with metal (main branch, carina, and proximal portion of the lateral branch). These sophisticated techniques are always associated with a more or less mechanical distortion of the stents implanted. In fact, in the most proximal portion of the bifurcation, at the primary vessel, there is usually more than one layer of metal against the vessel wall (with some techniques, up to 3 layers of overlapping metal). Complex double-stent techniques have been associated with an increased number of acute complications and delayed clinical and angiographic outcomes that are no better than those obtained with simpler strategies.1,7-9 However, we must also remember that, in day-to-day clinical settings, complex techniques are used precisely in the most adverse situations, or as rescue strategies when simpler techniques have failed.
Currently, a simple strategy is recommended, avoiding in-branch (provisional) stents whenever possible. The most popular option is implanting a stent in the main arm, and if the lateral branch is seriously diseased, dilating it with a balloon. Dilatation of the lateral branch can be performed before or after stent implantation in the main branch. Although this technique is associated with worse immediate angiographic outcomes in the lateral branch, multiple randomized studies have shown it to provide similar (or even better) long-tem results than complex or double-stent techniques.7-9
Moreover, the inherent anatomical complexity of coronary bifurcations has boosted the development of devices specifically designed for its treatment. These stents, commonly known as “dedicated” stents, have sophisticated structural designs that accurately adjust to changes in gauge and the whimsical angles that define these bifurcations.10 Other times, the structure is designed to facilitate double-stent techniques. However, the dedicated stent is more difficult to use and requires a complex learning curve to ensure adequate results.10 Moreover, despite its undeniable appeal, there are still no clinical outcomes that conclusively support its superiority over conventional stents. Finally, most stent models currently available are still not drug-eluting, and this certainly limits their appeal for these lesions with high risk of restenosis.
The arrival of drug-eluting stents signifies a very important step forward in the treatment of bifurcation lesions. Its use dramatically reduces the rate of restenosis in the main vessel and in the lateral branch. However, drug-eluting stents have also failed to produce superior results from complex or double-stent techniques when compared to simple “provisional stent” techniques with a single drug-eluting stent in the main vessel. More recently, the emergence of completely resorbable vascular devices has sparked interest. Initially, these devices were not considered suitable for those types of lesions because the larger profile of the structural elements could favor occlusion of the lateral branches. Additionally, their plastic composition makes them more susceptible to structural damage when it becomes necessary to dilate through their cells. However, by disappearing completely from the vessel wall, these devices would “free” initially caged branches, and would also avoid the delayed risk associated with overlap or deformation of their structural elements. Currently, the value of these devices in patients with bifurcation lesions is being intensively investigated.
RELEVANCE OF SOME TECHNICAL ASPECTSWhen the lateral branch is large, all investigators recommend protecting it with a guide to ensure subsequent access.1 After the stent is implanted in the main vessel, the lateral branch guide is temporarily “trapped” between the stent and the vessel wall. However, in the event of occlusion, this guide shows the exact location of the branch and maintains a favorable exit angle for easy access. If a lateral branch intervention is required, a guide must be introduced through it, but this time from the middle of the stent in the main vessel.1 In fact, the exact entry site of the guide to the lateral branch is important. Thus, studies with optical coherence tomography indicate that results are much better, with less stent distortion, when entry to the lateral branch is conducted through a cell relatively distal to the stent in the main vessel.11
As treatment of the lateral branch may not be easy, it seems reasonable to make sure it is indicated. Many “caged” branches have ostial lesions that appear angiographically severe, but are not functionally significant.12 This is due, first, to the difficulty in assessing these aforementioned ostial lesions, and second, to the fact that the stent itself can generate difficult-to-interpret linear images. In this context, pressure-guide studies analyze the physiological impact of these ostial lesions. It is often verified that these lesions are not functionally significant; therefore, they require no treatment.12
Other technical aspects also have practical implications. A frequent question is whether to predilate the lateral branch before implanting the stent in the main vessel or whether, on the contrary, it is preferable to treat the lateral branch only after implanting the stent in the main branch. It has been noted that the first strategy could avoid the need for further treatment of the branch or facilitate its final treatment after implanting the stent in the main vessel. Other authors, however, consider that lateral branch predilatation usually causes dissections that may hinder the passage of the guide or complicate its final treatment.
CURRENT STUDIESIn a paper published in Revista Española de Cardiología, Song et al13 introduce an interesting study analyzing the effects of lateral branch “predilatation” in coronary bifurcation lesions treated with a simple provisional stent technique. In all cases, the lateral branch was affected. This study is part of the COBIS (COronary BIfurcation Stent) registry, sponsored by the Korean Society of Interventional Cardiology, involving 16 centers. The primary objective was to compare the rate of “failure of the target vessel” (combined assessment of cardiac death, myocardial infarction or target vessel revascularization) among patients who underwent lateral branch predilation before stent implantation in the main vessel (N = 175) and those who did not (N=662).13 The group with predilatation (21% of the total) had a higher prevalence of diabetic patients and complex lesions. Furthermore, this group had more severe lateral branch stenosis, and kissing-balloon end dilatation was performed more frequently. Patients with pre-dilatation required a change to a double-stent strategy more frequently, but scored higher angiographic success in the lateral branch. Acute lateral branch occlusions were very rare, and similar in both groups. However, after a 2 -year clinical follow-up, the target vessel failure rate was significantly higher (double) in the predilatation arm (14.3% vs 6.8%; P=.002) due to the increased need for revascularization (12.0% vs 5.6%; P=.003).13 Most of these reinterventions were performed in the main vessel. Furthermore, branch predilatation was identified as an independent predictor of target vessel failure. To rule out that these results may be due to the presence of confounding factors, a conventional multivariate adjustment was made, followed by another analysis comparing 2 selected subpopulations (135 pairs of similar patients) selected after adjusting their characteristics to the propensity score methodology (which tries to avoid biases induced by the treatment received). The results of both analyses were consistent. Finally, the findings were also consistent when several anatomical subgroups of particular relevance were analyzed. There was only 1 significant interaction between the type of intervention and the result obtained in the presence of calcium in the lateral branch, further worsening the results obtained when predilation was performed. The strength behind this work is based on a centralized analysis with quantitative angiography, where 8 different arterial segments were analyzed in each bifurcation. Finally, we must stress that clinical follow-up was completed for all patients, and that allocation of adverse events was conducted by an independent committee.13
The study is of undoubted practical interest, and suggests that in bifurcation lesions considered for a provisional stent strategy, lateral branch predilatation should be avoided. However, for a proper interpretation of the study, it is necessary to consider some methodological considerations.13 First, this is a retrospective analysis of patients listed in the COBIS registry. We know that, regardless of the quality of the database used, it is very difficult to establish, a posteriori, the real reasons for lateral branch predilatation. It is also possible that some parts of the process were not recorded, thus hindering further analysis. However, the elegant and comprehensive statistical adjustment, performed in order to account for the influence of clinical and anatomical variables that could have acted as confounding factors, is methodologically very solid and, in principle, able to dispel these doubts. However, we cannot completely rule out that other unmeasured variables may have influenced final results. In other words, surgeons may have really wanted to predilate the lateral branch in the most complex bifurcations, and it may be this fact, and not predilatation per se, that explains the worst delayed outcomes obtained in this cohort of patients. Greater severe stenosis at lateral branch origin and increased need for kissing balloon and double end-stent in this subgroup could point in that direction. Moreover, in the current analysis up to 25% of patients in the registry COBIS registry were excluded for various reasons (inappropriate images, initial occlusion of the lateral branch, elective double-stent technique), indicating that the population is a selected sample and, therefore, may not be representative of patients with bifurcation treated in daily practice. Finally, it is surprising that an initial treatment on the branch before stent implantation in the main vessel penalizes to such an extent the delayed revascularization of the main vessel, but the authors have no hypothesis to convincingly explain this phenomenon.
Are there other current studies on this subject? A randomized study conducted quite recently in Spain was designed specifically to analyze the effects of lateral branch pre-dilatation.14 In this controlled study, Pan et al included a total of 372 patients with bifurcation lesions (187 assigned to lateral branch predilation and 185 without predilation). The branch ostium should have been significantly affected and be > 2.25mm in diameter, and the initial strategy was always provisional T stent in the lateral branch. At the end of the procedure, either sequential dilation or a kissing balloon was performed, at the discretion of the surgeon. The primary purpose of assessment (presence of TIMI [Thrombolysis In Myocardial Infarction] 0-1 flow in the lateral branch immediately after stent implantation in the main vessel) was significantly lower (1% compared to 10%, P<.001) in the group with predilatation. However, the occurrence of acute complications was similar in both groups, indicating that the vascular occlusion was transient; in fact, the need for a stent in the lateral branch (4% compared to 3%) was very low. Interestingly, after stent implantation in the main vessel, 1 in 3 branches of the group with predilatation still had stenosis<50% and TIMI 3 flow, and did not require further treatment (significant difference compared with the group without predilatation). From a clinical point of view, both strategies were associated with excellent progression and survival free of adverse events (death, myocardial infarction, vessel revascularization); after 2 years of follow-up, it was also similar (92% of the predilatation group compared to 90% in the group without predilatation).14 These excellent clinical outcomes contrast with the high rate of events reported in the study by Song et al.13
A direct comparison of these 2 studies is very risky due to their different design and methodology, but can be revealing. The study of Song et al13 confirms the importance of observational studies to formulate new hypotheses. These studies tend to include more patients, who are usually less selected, and their findings can be better extrapolated to daily clinical practice. However, only randomized studies that prospectively evaluate a direct question can provide a definitive answer to guide our clinical decisions. It is difficult to know whether the differences between the 2 studies is due to poor adjustment of baseline characteristics in the Korean retrospective and observational study,13 or to a more restrictive selection of patients in the prospective and randomized Spanish study.14 In any case, in the event of discrepancies (which, in principle, these studies seem to have between them), it is better to heed the results of the randomized study, but always remembering the characteristics of included patients.
FINAL CONSIDERATIONSIt is clear that we know how to treat bifurcation lesions.1 However, these lesions remain a therapeutic challenge, and present an increased risk of complications. It also seems clear that the provisional stent strategy, using only one drug-eluting stent in the main vessel, is the first choice of treatment for most of these patients.1 Although systematic predilation of the lateral branch cannot be recommended, this strategy seems to be associated with lower branch occlusion during the procedure and less need for further treatment after stent implantation in the main vessel, but without long-term clinical differences. Therefore, this decision must be left to the surgeons’ judgment, according to the characteristics of the lesion, the type of planned intervention, and their experience. An interesting modification of this strategy is to use a drug-eluting balloon (instead of a conventional balloon) to treat the lateral branch. However, the potential value of this novel therapy will remain speculative as long as it is not properly analyzed in controlled studies. We must also be alert to the continuous advances in the field of drug-eluting stents,15 especially those intended exclusively for bifurcations, which may soon allow for complete reconstruction of more complex lesions, with increased safety and effectiveness. Again, their systematic application in medicine16 must be based on controlled studies to confirm their superiority over simpler strategies.
CONFLICTS OF INTERESTNone declared.