In 2016, between 1810 and 1890 traffic accident fatalities occurred in Spain1,2; additionally, of the 140 390 resulting injuries, 9755 required hospitalization. The main causes of traffic accidents are violation of traffic rules, lack of attention, and poor vehicular state. Illness causes less than 0.5% of accidents resulting in injuries3,4 and rarely results in injury to someone other than the driver.5,6 Nonetheless, unwell drivers have an increased relative risk of accidents, which reaches a maximum of 2.01 for some mental illnesses. For cardiovascular diseases, the relative risk ranges from 1.03 for individuals with hypertension to 1.52 for those with ischemic heart disease.7,8
Legislators developing regulations must balance both individual and societal safety with a respect for individual freedom. Driving is a right of considerable value for patients, both due to its social importance and due to its role in physical, mental, and occupational rehabilitation.9 Therefore, driving should only be restricted when essential for a person's integrity and collective safety. Once both aspects–safety and individual rights–have been considered, these regulations, once approved, apply to all citizens and are particularly important for physicians and patients.
Driving does not involve considerable physical effort. Car driving constitutes an energy consumption of 1 to 2 METs for a person weighing 70kg, equivalent to walking at a slow pace or sewing. Truck or bus driving involves a consumption of between 2.5 and 4 METs, equivalent to riding a bicycle at 10km/h.10 Therefore, driving as an activity can only be physically limited in patients with symptoms that appear at rest or with minimal exertion. The risk due to driving is not due so much to symptoms of angina or dyspnea as to the risk of arrhythmias and syncope,9 which is even higher in patients with more severe heart disease.11 Assessment of cardiac patients in terms of driving should focus on the risk of loss of attention, which is typically associated with the worst functional classes.
The Canadian Society of Cardiology applied a risk estimation formula to its guidelines for driving.12 This formula has been adopted in the expert group report on cardiovascular disease and driving in the European Union,13 which forms the basis for a new directive.14 The formula includes the time at the wheel, the type of vehicle, the risk of sudden incapacitation, and the probability that this incapacitation will result in harm. In the legislation, the first 2 variables and part of the last are considered after the restrictions are subdivided according to 2 driving groups: group 1, low-size and -weight vehicles (cars); group 2, large-size and -weight vehicles, typically for professional and commercial use.14 The time spent driving, potentially important in professionals such as commercial travelers, is not included as a risk factor and must be considered in the medical evaluation. The group of experts carefully evaluated the other component of the equation–the risk of sudden incapacitation–in light of new understanding of cardiovascular medicine and uses it as the basis of its report and the new European regulations.
Directive 2016/1106 of July 7th, 2016, from the European Commission of the European Union (EU)14 amends Directive 2006/126/EC,15 fulfilling the instructions of the Driving Permit Committee of the EU to adapt the law to the latest information on cardiovascular diseases and their management. To develop the directive, the Committee populated a working group on cardiovascular disease and driving with cardiologists from various EU countries. The experts were tasked with developing a consensus document detailing the conditions that do not impede driving, when a driving license cannot be issued or renewed, and when renewal terms can be shortened or must depend on medical reevaluation. The document was completed in 201313 and forms the basis of the new directive of 2016,14 which must be transposed to the legislation of all EU member countries. Since its publication in the Spanish Boletin Oficial del Estado (Official State Bulletin), the regulation has had an impact on the restrictions possibly affecting our patients and, crucially, our clinical practice because it introduces the need for certain tests and periodic reviews and for patient guidance.
The new regulation16 represents a marked change from the previous one, included in the Spanish General Regulation of Drivers of 2009,17 the previous legislation governing this area. New problems are included, such as stents and some specific cardiomyopathies, and the previously considered knowledge is updated. It leaves the door open to future changes in practice by considering a wide range of new therapeutic options, such as circulatory assistance. Because it is mandatory, the regulation must be known by all cardiologists and medical evaluators, but it is also useful as a guideline in daily clinical practice and in terms of patients’ rehabilitation and return to work goals. Generally, and compared with the regulation hitherto in force, the new legislation shortens the length of the driving ban after acute episodes and interventions, extends the validity periods, and reduces some requirements related to left ventricular ejection fraction (LVEF) and functional class. Because the new criteria consider many diseases in depth, specialists must be familiar with the regulation and consider the information in the clinical report (specific heart disease, established treatment, presence or absence of syncope, LVEF, functional class) used by medical evaluators to make decisions on an individual's ability to drive. In some cases, due to the complexity of the disease, the participation of the cardiologist and communication with the evaluating physician are necessary for the final decision.
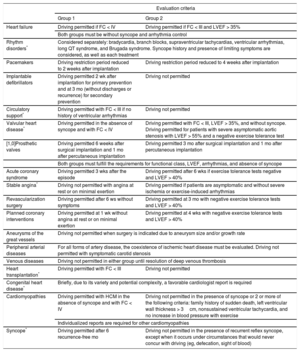
The requirements for driving related to different diseases and procedures included in the regulation are summarized in Table 1. In general, the requirements are more stringent for group 2 drivers (professionals) than for group 1 drivers (cars and motorcycles). When several problems concur, the most restrictive rule prevails. An individual report issued by a cardiologist is often required, and the renewal and revision times are different for each disease. The reader can obtain more information by consulting the European Commission Directive,14 Order PRA/375/2018, of April 11, which modifies Annex IV of the Spanish General Regulation of Drivers,16 and the much more extensive scientific document supporting them in the expert report of the European Working Group on Driving and Cardiovascular Disease.13
Order PRA/375/2018, of April 11th, Which Modifies Annex IV of the Spanish General Regulation of Drivers, Approved by Royal Decree 818/2009 on May16
| Evaluation criteria | ||
|---|---|---|
| Group 1 | Group 2 | |
| Heart failure | Driving permitted if FC < IV | Driving permitted if FC < III and LVEF > 35% |
| Both groups must be without syncope and arrhythmia control | ||
| Rhythm disorders* | Considered separately: bradycardia, branch blocks, supraventricular tachycardias, ventricular arrhythmias, long QT syndrome, and Brugada syndrome. Syncope history and presence of limiting symptoms are considered, as well as each treatment | |
| Pacemakers | Driving restriction period reduced to 2 weeks after implantation | Driving restriction period reduced to 4 weeks after implantation |
| Implantable defibrillators | Driving permitted 2 wk after implantation for primary prevention and at 3 mo (without discharges or recurrence) for secondary prevention | Driving not permitted |
| Circulatory support* | Driving permitted with FC < III if no history of ventricular arrhythmias | Driving not permitted |
| Valvular heart disease* | Driving permitted in the absence of syncope and with FC < IV | Driving permitted with FC < III, LVEF > 35%, and without syncope. Driving permitted for patients with severe asymptomatic aortic stenosis with LVEF > 55% and a negative exercise tolerance test |
| [1,0]Prosthetic valves | Driving permitted 6 weeks after surgical implantation and 1 mo after percutaneous implantation | Driving permitted 3 mo after surgical implantation and 1 mo after percutaneous implantation |
| Both groups must fulfill the requirements for functional class, LVEF, arrhythmias, and absence of syncope | ||
| Acute coronary syndrome | Driving permitted 3 wks after the episode | Driving permitted after 6 wks if exercise tolerance tests negative and LVEF > 40% |
| Stable angina* | Driving not permitted with angina at rest or on minimal exertion | Driving permitted if patients are asymptomatic and without severe ischemia or exercise-induced arrhythmias |
| Revascularization surgery | Driving permitted after 6 ws without symptoms | Driving permitted at 3 mo with negative exercise tolerance tests and LVEF > 40% |
| Planned coronary interventions | Driving permitted at 1 wk without angina at rest or on minimal exertion | Driving permitted at 4 wks with negative exercise tolerance tests and LVEF > 40% |
| Aneurysms of the great vessels | Driving not permitted when surgery is indicated due to aneurysm size and/or growth rate | |
| Peripheral arterial diseases | For all forms of artery disease, the coexistence of ischemic heart disease must be evaluated. Driving not permitted with symptomatic carotid stenosis | |
| Venous diseases | Driving not permitted in either group until resolution of deep venous thrombosis | |
| Heart transplantation* | Driving permitted with FC < III | Driving not permitted |
| Congenital heart disease* | Briefly, due to its variety and potential complexity, a favorable cardiologist report is required | |
| Cardiomyopathies | Driving permitted with HCM in the absence of syncope and with FC < IV | Driving not permitted in the presence of syncope or 2 or more of the following criteria: family history of sudden death, left ventricular wall thickness > 3cm, nonsustained ventricular tachycardia, and no increase in blood pressure with exercise |
| Individualized reports are required for other cardiomyopathies | ||
| Syncope* | Driving permitted after 6 recurrence-free mo | Driving not permitted in the presence of recurrent reflex syncope, except when it occurs under circumstances that would never concur with driving (eg, defecation, sight of blood) |
FC, functional class; Group 1, private driving; Group 2, commercial driving; HCM, hypertrophic cardiomyopathy; LVEF, left ventricular ejection fraction.
The new rule regulating the driving permissions of people with cardiovascular diseases16 is the first in both Spain and the EU to be the result of a systematic study of the evidence by a group of experts. Although the evidence may be scarce at times, this approach was considered essential to give objective value to the regulation. Despite the delay between the conclusion of the first expert document in 201313 and its transposition to the legal guideline,16 we believe that it maintains an up-to-date value, both because of the exhaustive work involved and because it considers the most innovative therapeutic approaches. Complex conditions, such as congenital heart disease or various types of cardiomyopathy, require specific advice due to the variety of their presentations, which makes them difficult or impossible to tabulate. Syncope will be a problem until both its etiology and the risk of recurrence during driving become clear. Despite the provision of more detailed tables, a rigorous clinical assessment and communication between specialists and medical evaluators will still be necessary. There will be some differences among the specific rules of the different countries of the EU: because the directive is a minimum standard, some countries might be more restrictive, although never less than indicated in the directive. Finally, the legal rules summarized here should act as a guide for daily consultation because our patients need to know when they can drive a vehicle again, either privately or to earn a living, safe in the knowledge that not only do they meet the legal requirements, but that they do so without threatening anyone's safety.
CONFLICTS OF INTERESTNone declared.
.