The concept of multimodality imaging has been developing rapidly in recent years due to the need to integrate information on anatomy (which defines coronary artery disease) with functional data (which reflects the effects of this disease on tissues) to enable the proper evaluation of patients with ischemic heart disease.
From the clinical point of view, it has been well established that a complete evaluation of a coronary lesion requires not only morphological information on the location of the stenosis, but also functional information on its impact. Van Werkhoven et al1 have demonstrated that the combination of anatomical and functional information can improve patient risk stratification. Thus, patients with ≥ 50% coronary occlusion associated with perfusion defects experienced a higher annual event rate during follow-up (9%) than patients with no significant coronary lesions or perfusion defects (1%).
While the severity of ischemia is related to the degree of stenosis, this relationship is not always linear. A number of factors apart from the degree of occlusion (assessed by coronary luminography) establish whether or not a given stenosis induces a myocardial perfusion defect. Among these factors, we stress the importance of the existence of collateral circulation and the phenomenon of arterial vasospasm, a functional mechanism that can overlap a mild fixed lesion, leading to significant occlusion. In addition, a nonsignificant arteriosclerotic plaque can become destabilized and produce serious or even total arterial occlusion. Moreover, the phenomenon of “ischemic preconditioning” could play a role in the discrepancy between anatomical and functional changes. Given all these circumstances, evaluation of the functional relevance of the coronary stenosis is recommended to guide revascularization strategies. If, in addition, this dual information can be obtained using noninvasive methods and can be presented jointly (by means of image fusion), the result facilitates optimal clinical decision-making, while also reducing the risk inherent in invasive diagnostic techniques.
Since the 1990s, stress and rest myocardial perfusion scintigraphy has been developed as an excellent noninvasive method to obtain the functional information required for the assessment of patients with ischemic heart disease. These myocardial perfusion images represent the integration of the regional myocardial blood flow and the metabolic activity of the cardiac muscle cells (molecular image). The use of a tomographic technique in the acquisition of these images facilitates the 3-dimensional presentation of both the stress and rest images, simplifying their comparison. A number of studies have demonstrated their relevance in the assessment of patients with ischemic heart disease, due to both their diagnostic value and their prognostic value during follow-up. In this respect, the event rate recorded during follow-up in patients with good functional capacity and absence of myocardial perfusion defects is low.2
Noninvasive computed tomography (CT) coronary angiography has been introduced more recently. However, as a result of the progressive technical advances made in scanners in recent years, this modality has gained widespread clinical acceptance.3 The latest generation of scanners have improved spatial and temporal resolution and have reduced the radiation dose. Thus, through a noninvasive approach, these scanners allow accurate and necessary anatomical information to be obtained and combined with the findings of other imaging modalities (multimodality imaging). However, the presence of coronary calcification still constitutes a limitation to the luminographic assessment of CT studies, as the partial volume artifact produced by coronary calcification can result in an overestimation of the severity of the lesion. In these equivocal cases, the availability of functional information increases diagnostic accuracy and improves the sensitivity and specificity of the examination.
In 2002, Cerqueira et al4 standardized the division of the left ventricular myocardium into 17 segments and, moreover, established a correlation with coronary anatomy. However, more recent studies have demonstrated that these designations vary, depending on the dominance of the arteries in a given patient.5 For example, segments 3, 9, and 15 can be assigned to the right coronary artery or to the anterior descending coronary artery; segments 4, 5, 10, and 11 to the right coronary artery or to the circumflex artery; and segment 12 to the anterior descending coronary artery or to the circumflex artery. This view of the segmentation of myocardial perfusion creates uncertainty about the identity of the culprit vessel in the absence of individualized anatomical information provided by CT or coronary angiography.
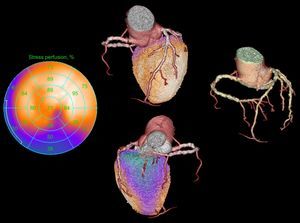
Thus, there is interindividual variability in the sites of myocardial ischemia and of coronary stenosis. In this respect, fusion of 3D images based on software able to merge perfusion information from single-photon emission computed tomography (SPECT) with anatomical information provided by CT offers diagnostic information that improves on simple identification of the culprit lesion. This information increases confidence in the diagnosis and contributes to a better classification of intermediate lesions and equivocal perfusion defects (Figure 1).
Polar map from stress myocardial perfusion scintigraphy (left), 3D reconstruction of the coronary computed tomography scan with high calcium burden in the 3 vessels (right), and anterior and posterior single-photon emission computed tomography/computed tomography fusion images that permit the correct evaluation of the culprit vessel (right coronary artery, center).
The current technological progress also joins forces with efforts to aid the direct performance of multimodality imaging through the design of hybrid scanners that integrate 2 technologies in a single unit. In nuclear cardiology, the new hybrid systems for SPECT/CT, positron emission tomography (PET)/CT, and PET/magnetic resonance (MR) have sufficient imaging quality and sufficiently powerful software to enable the integration of this information in multimodality hybrid images obtained with the same scanner. However, because of the high cost of these systems (both their purchase and maintenance), their use is restricted to a small number of centers. Moreover, the still limited experience in the interpretation and clinical value of these hybrid images relegates their use mainly to research, and consequently that this information is not a determining factor in clinical decision-making.
Another important technological advance is the commercial availability of different programs for the fusion of images from different complementary studies. The speed and automation with which they function have facilitated their application in daily practice, as the processing required with the initial systems was extremely time-consuming.6
The first clinical reports involving multimodality fusion with nuclear cardiology images date back to the beginning of the year 2000,7,8 with the integration of scintigraphic images of myocardial perfusion and conventional invasive biplane coronary angiographic images, acquired at Emory University (Atlanta, Georgia, United States). This multimodality approximation prior to the use of CT was not further developed because of the complexity of the digitization of biplane coronary angiographic studies.
In Europe, the group at University Hospital Zurich, in Switzerland,6 pioneered the use of studies involving the fusion of myocardial perfusion SPECT and coronary CT, producing a large number of publications and review articles. According to Gaemperli et al,9 in addition to being intuitively convincing, SPECT/CT fusion images provide added value in the form of diagnostic information on the functional relevance of coronary artery stenoses. For this reason, those authors recommend multimodal image fusion in clinical practice.
The use of fusion images improves sensitivity (17% increase) and, particularly, the specificity of the diagnosis of significant10 coronary artery disease compared with analysis of myocardial perfusion alone, or even with evaluation of perfusion and coronary CT separately, leading to a change in the initial interpretation in 28% of cases. Moreover, in patients with multivessel disease and a heavy coronary calcium burden (in which analysis of the anatomical lesion is complicated), image fusion improves the interpretation of coronary CT and also allows identification of the causative lesion11 (Figure 1). In a recent study, Schaap et al12 evaluated the value of hybrid SPECT/CT images, comparing them with analysis based on SPECT or CT alone, in 205 patients with significant coronary artery disease (diagnosed on the basis of the presence of ≥ 50% coronary occlusion according to invasive coronary angiography or because the fractional flow reserve was less than 0.80). These authors concluded that the yield of SPECT/CT fusion images was superior to analysis using SPECT or CT alone in the diagnostic study of patients with suspected significant coronary artery disease.
Fusion images have been shown to be valuable not only in the diagnosis of coronary artery disease, but also to have prognostic implications. In 324 patients followed-up for a median of 2.8 years, Pazhenkottil et al13 demonstrated that a matched defect on a hybrid image is a strong predictor of major adverse cardiovascular events (MACE) during follow-up.
Given the scientific evidence accumulated in recent years, the use of multimodality fusion images of myocardial perfusion and coronary CT is now defined in the guidelines of the European Association of Nuclear Medicine14 (EANM) and the guidelines of the Society of Nuclear Medicine and Molecular Imaging/American Society of Nuclear Cardiology/Society of Cardiovascular Computed Tomography15 (SNMMI/ASNC/SCCT) in the United States. Both guidelines recommend the use of hybrid images in patients at intermediate risk for coronary artery disease, since the diagnostic and prognostic information they provide is superior to that offered by myocardial perfusion SPECT or coronary CT alone.
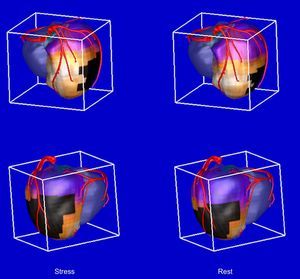
However, the cumulative experience in our center, where we use image fusion to evaluate the culprit artery and the extent of myocardium at risk (Figure 2), also leads us to be critical of the indiscriminate use of the different cardiac imaging techniques. In this respect, in patients with stable ischemic heart disease who have undergone myocardial perfusion SPECT as a first noninvasive study and with a clear indication for the performance of invasive coronary angiography based on the results of SPECT, the performance of a CT scan and the acquisition of SPECT/CT fusion images do not appear to be indicated, as the results would not change the approach adopted for therapeutic management.
Fusion of single-photon emission computed tomography/coronary computed tomography images in the evaluation of myocardium at risk, extent of the perfusion defect, and myocardial viability (courtesy of E.V. García, Emory University). Upper images: left anterior oblique views. Lower images: left posterior oblique views. Left: stress study. Right: rest study. Black area overlying the image, blackout region that exceeds the normal reference ranges for myocardial perfusion in these segments.
There is still little experience in the multimodality fusion imaging of myocardial perfusion and cardiac MR, especially because of the limited availability of hybrid PET/MR scanners and the nonexistence of SPECT/MR systems. From the cardiovascular point of view, PET/MR could be an excellent tool for the assessment of myocardial viability (glucose metabolism with fluorodeoxyglucose [18F-FDG PET] and late gadolinium enhancement in MR) and for the combined study of areas of fibrosis and inflammatory activity, as in the case of myocarditis or sarcoidosis. In the latter, the differentiation between the acute phase and chronic phase of sarcoidosis is highly useful in guiding patient treatment and in influencing the prognosis of the disease (as cardiac involvement is the major marker of adverse events during patient follow-up). Another application of PET/MR image fusion would be the study of cardiac masses. Cardiac MR imaging, together with CT, is currently one of the gold standards for the noninvasive differential diagnosis and local staging of cardiac tumors. An additional perspective on tumor metabolism could probably aid in the evaluation of the grade of malignancy and in the detection of occult tumor sites.
Clinical experience in the use of PET/CT systems for the evaluation of regional myocardial blood flow in patients with suspected coronary artery disease is greater, as a single study suffices for the examination of coronary anatomy and myocardial perfusion and the quantification of absolute tissue blood flow (mL/min/g of myocardial tissue). Another application that is highly relevant in clinical practice is the study of vasculitis and infective endocarditis. In these conditions, the joint presentation of anatomical information from cardiac CT with the functional image of local glucose metabolism (which indicates the presence of inflammation and/or infection) is essential to evaluate the site, grade, and extent of the inflammation/infection (Figure 3), as well as the possible complications. This examination is highly useful, especially in patients with heart valve prostheses, vascular tubes, and/or cardiac devices (pacemakers, defibrillators, etc), in whom ultrasound examination has greater limitations and is associated with a higher rate of false negatives. Finally, there is increasing scientific evidence that PET/CT image fusion may play an important role in the characterization of vulnerable arteriosclerotic plaques at risk of rupture.
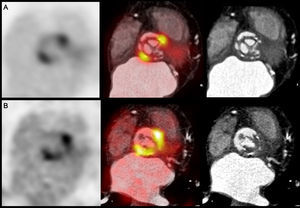
Positron emission tomography with fluorodeoxyglucose (18F-FDG PET) and cardiac computed tomography in the evaluation of prosthetic endocarditis. A: 18F-FDG PET slices, PET/CT fusion, and cardiac CT at the level of the aortic valve prosthesis, showing intense focal glucose hypermetabolism in the periannular region. B: 18F-FDG PET slices, PET/CT fusion, and cardiac CT at the supravalvular level, where the existing vegetations and the larger periannular area of 18F-FDG uptake can be observed.
None declared.