Alcoholic cardiomyopathy (ACM) is a condition of toxic origin that causes gradual changes in the structure and function of the heart, resembling those seen in idiopathic dilated cardiomyopathy (CMP). ACM occurs in persons who consume large amounts of alcohol (>100g/d in men, > 80g/d in women) over a long period of time (at least 5 years, usually around 15 years) in the absence of other significant heart disease.1–3 In western countries, this condition accounts for approximately one third of all cases of acquired dilated CMP. ACM may affect up to one third of all consumers of large amounts of alcohol.2 As the overall alcohol consumption of the Spanish population has not decreased in recent years, neither has the incidence of ACM, and alcohol intake continues to be an important risk factor for both ACM and cardiovascular disease.3 Moreover, the harmful effects of alcohol may be added to those of other cardiovascular risk factors, such as hypertension, diabetes mellitus, and hypercholesterolemia. It has also been reported that, because of the toxic systemic effect of alcohol and its metabolites, other organic diseases related to alcohol use, such as liver cirrhosis, alcoholic dementia, and protein-calorie malnutrition, increase the risk of developing ACM.3
For many years, the potential reversibility of ACM has been a subject of medical interest. Already in the IV century BC in Greece, Hippocrates observed that patients with “hydropsy”, the clinical equivalent of congestive heart disease, improved when they stopped drinking alcohol, a recommendation that has persisted to this day. However, we need to look back to the XIX century in German beer drinkers to find clear clinical descriptions of ACM reversibility with abstinence from alcohol. In t, for a very long time people doubted that alcohol consumption, in itself, was the cause of dilated CMP. It was suggested that contaminants in the beer such as cobalt and arsenic used as defoaming agents brought about this condition, and not the ethanol. Another proposal was that ACM could be caused by the protein-calorie malnutrition, thiamine deficiency (western Beriberi), or the deficits in selenium, magnesium, or phosphorus that are often associated with chronic alcohol consumption.4
Some 30 years ago, several clinical and experimental studies verified that ethanol was the cause of this toxic dilated CMP, and that there was a clear dose-dependent effect related to the cumulative alcohol consumption over the lifetime of each person.2 This generated the concept of total lifetime alcohol intake (LAI) per kilogram of body weight as an approach to better estimate the personal risk of developing ACM. Thus, the natural history of ACM has been defined as a chronic disease that initiates with a subclinical phase in which the only change observed is left ventricular diastolic dysfunction.5 This is followed by the systolic dysfunction phase, with a gradual decrease in left ventricular ejection fraction (LVEF). In this phase, events related to congestive heart failure and arrhythmias appear, and there is a clear increase in mortality in persons who continue to consume large amounts of alcohol.6 Binge drinking is particularly detrimental over the course of ACM, as it can trigger acute cardiac events of this type (holiday heart syndrome).3 It was also seen that women are more prone to develop ACM than men7 and that some genetic polymorphisms such as angiotensin-converting enzyme DD genotype increase the risk of developing this condition.3,6
With regard to the pathogenesis of ACM, it is currently considered to be a direct toxic effect of alcohol through multifactorial and synergistic mechanisms. These include Ca2+-dependent signal transduction changes affecting myocardial contractility, the antioxidant and proinflammatory effects of alcohol and acetaldehyde, changes in the synthesis of structural and contractile proteins, and apoptosis induction, with consequent cardiomyocyte loss and replacement by subendocardial and interstitial fibrosis1,4 (Figure 1). Furthermore, alcohol inhibits cardiomyocyte repair and replication mechanisms, which worsens myocardial remodeling.3 Finally, a recent study suggested that certain myokines (FGF-21, METRNL, IGF-1, myostatin) may play a role in modulating ethanol-induced myocardial injury and myocardial repair mechanisms.8
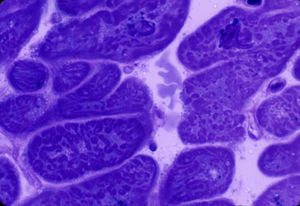
Left ventricular myocardial biopsy. Patient with chronic alcoholic cardiomyopathy. There is marked cellular and nuclear hypotrophy, destructuring of the sarcomeric pattern of cardiomyocytes, and interstitial fibrosis. Electron microscopy of a semithin section × 600 magnification, stained with toluidine blue.
Based on these data, it is it is reasonable to conclude that all ACM patients should completely abstain from alcohol.2–4 However, in general, these patients have an elevated LAI (> 20kg of ethanol/kg of body weight) and are alcohol-dependent. Despite undergoing specific detoxification programs, not all patients achieve lasting alcohol abstinence. Around one third continue drinking large amounts of alcohol despite recommendations to abstain, which leads to high mortality, at an annual rate of more than 10%. Another subgroup (30%-40%) is only able to reduce previous alcohol consumption to moderate doses (<60g/d). In ACM patients who persistently abstain from alcohol intake, a fast, significant improvement has been observed in LVEF.9 However, patients with severe left ventricular dysfunction (LVEF <15%) do not experience improvements over time despite abstinence.6,10 In this phase of the condition, there is abundant myocytolysis and myocardial fibrosis, with no possibility of functional or structural reversal.3,4
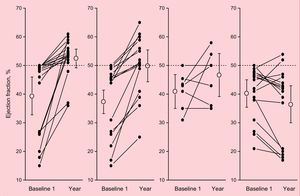
In this scenario, a recommendation of controlled consumption at low doses has been contemplated for ACM patients who are unable to completely abstain from alcohol intake. Hence, a previous study by our group in a series of ACM patients assessed the LVEF changes at 4 years according to the level of maintained consumption. Nicolás et al.10 found that ACM patients whose LVEF showed the greatest improvement were those achieving complete abstinence. One year later, the mean LVEF had even normalized. In addition, they found that LVEF worsened over time in patients who continued consuming alcohol at high doses (> 80g/d). However, those who controlled their intake at low doses (< 60g/d) without binging showed a significant improvement similar to that seen in abstainers (Figure 2). The authors concluded that abstinence is the best recommendation for ACM patients, but if total abstinence is not achieved, controlled alcohol consumption (< 60g/d), avoiding binging, is an adequate strategy to follow. Guzzo-Merello et al.11 reported comparable findings in another study, carried out over 59 months: Survival rates and recovery of ventricular function were similar between ACM patients who reduced alcohol consumption and abstainers. In that study, the clinical course of patients with ACM was more favorable than that of patients with idiopathic dilated CMP. Fauchier et al.12 also observed a similar long-term LVEF increase between ACM patients who stopped drinking and those who controlled their alcohol intake. However, not all authors concur with the recommendation of controlled consumption in this population. Some, such as Gavazzi et al.,13 found an LVEF improvement only in complete abstainers; hence, there is some controversy in this respect. Another point to note is that ACM patients practicing controlled alcohol intake are at a risk of relapsing to high-dose alcohol consumption.
Alcoholic cardiomyopathy reversibility according to the patients’ consumption over time. Alcoholic cardiomyopathy patients who remain abstinent show better left ventricular ejection fraction (LVEF) recovery than the other groups. LVEF in patients who continue consuming large amounts of alcohol (> 80g/d) show a poorer clinical course. Of note, patients who did not achieve abstinence, but managed to decrease alcohol intake to < 60g/d (considered to be controlled consumption) showed an improvement similar to that of abstainers. (Reproduced with the permission of Nicolás et al.)10.
We believe that the recent article by Amor-Salamanca et al.14 in Revista Española de Cardiología, assessing the prognostic impact and related predictive factors of LVEF recovery in patients with ACM, helps to clarify this situation. The authors monitored the long-term clinical course of 101 ACM patients for a mean of 82 months. A significant LVEF increase was seen in 42% of patients (absolute increase > 10% and final LVEF > 40%), and these patients had a better prognostic course than those without LVEF recovery. The predictive factors of LVEF recoverydefined by the authors were QRS duration < 120ms, beta-blocker treatment, and no requirement for diuretics, all of which seem logical. QRS duration < 120ms has been related to higher LVEF values and longer survival in dilated CMP patients, and with fewer episodes of heart failure with decreased LVEF.15 Beta-blocker treatment is clearly related to improved LVEF and a smaller number of arrhythmias in dilated CMP. The fact of not needing diuretics is associated with better baseline left ventricular function, as the signs of cardiac congestion only appear in advanced phases of ACM.4 Curiously, alcohol consumption was not a predictive factor of LVEF improvement in this study, although the LVEF did not recover in any of the 6 patients who maintained excessive intake. This may have been because the study population did not include patients who consumed large amounts of alcohol (> 200g/d), in contrast to other studies.2,10 Furthermore, alcohol consumption was not measured in grams, but instead, in intervals, which decreased the power of this parameter in the statistical analysis. As to the ACM patients who maintained moderate alcohol intake, this study also found that the percentage with LVEF recovery was similar to that of abstainers (44% vs 45% respectively). This led the authors to conclude that there is a relationship between LVEF recovery and the prognostic course of ACM patients, and that LVEF recovery is similar between moderate drinkers and abstainers.
We should like to point out 2 aspects in the study by Amor-Salamanca et al.14 that we consider crucial to reversing ACM. The first is that abstinence is the best strategy to achieve functional recovery, but when abstinence is not attained, controlling alcohol intake is also useful. However, it is not beneficial to recommend moderate drinking in ACM patients with alcohol dependence, as they have a nonnegligible risk of relapsing to high-dose consumption. Hence, we believe that the physician's recommendation of abstinence should always prevail over that of controlled consumption.3,6 This leads us to a widely mentioned norm applicable to this situation “less alcohol is best for the heart”.3 The second aspect to mention is the following: As left ventricular dysfunction is the most important functional marker of ACM, LVEF recovery is the best parameter for monitoring ACM patients over time.
Estimating the prognostic course is important in ACM, not only in clinical terms, but also to evaluate potential treatment interventions, such as cardiac resynchronization with implantable automatic defibrillator placement or inclusion in a heart transplant program. According to the findings of the study by Amor-Salamanca et al.,14 a cutoff point of 40% for LVEF recovery could be the limit indicating a favorable prognosis, as mortality in CMP patients with LVEF > 40% is very low. Therefore, a reasonable objective for all ACM patients would be to achieve LVEF recovery to > 40%. It is known that treatment with beta-blockers and angiotensin-converting enzyme inhibitors//angiotensin II receptor agonists is useful for improving heart function.11 We also consider that, although diuretic use was found to be a negative predictive factor in this study, it identifies patients in more advanced phases of ACM and therefore, diuretic use should not be withdrawn in the congestive phase of this condition. Lastly, although sufficient evidence is still lacking to recommend their use, new strategies have been proposed to attain functional recovery in ACM patients. These include the use of cardiomyokines or myocardial growth and regulation factors, as well as various techniques for myocardial cell regeneration. These approaches will have to be considered in the future to improve the prognostic course of patients whose LVEF does not recover up to at least 40% with the usual measures.8
CONFLICTS OF INTERESTJ. Fernández-Solà is the principal investigator in Proyecto 2015 33/31 La Marató and is integrated in the program SGR 2017/Generalitat de Catalunya and in CIBEROBN, Instituto de Salud Carlos III.
.