Cardiovascular disease is the main health problem in Europe and the rest of the world and is the leading cause of death and health care expenditure. By reducing mortality and ischemic event recurrence, prevention strategies play a fundamental role in patients who have had an acute coronary syndrome. Although these prevention strategies have focused with great success on high-risk individuals, they should also be used in the general population, which is showing an increase in the prevalence of obesity, diabetes mellitus, and other comorbidities that may reverse this trend toward reduced mortality. The present article consists of an up-to-date review of the main cardiovascular prevention measures, particularly the new developments of the last year, as well as the particularities of these measures when they are targeted at patients with a prior acute coronary syndrome.
Keywords
Increased understanding of cardiovascular risk factors and the use of both primary and secondary prevention measures have considerably reduced cardiovascular mortality during the last 40 to 50 years in developed countries. However, despite advances in prevention measures, cardiovascular disease continues to be the leading cause of death in developed countries and is one of the main causes of disability and health care expenditure. Moreover, although progress has been made in the treatment of acute coronary syndrome (ACS), its annual rates have been stable in the last decade. The impact of prevention measures is offset by an alarming increase in obesity and diabetes mellitus, population aging, and the appearance of other comorbidities, such as renal failure, which increase the risk of developing ACS, to the extent that this increase could reverse the downward trend in mortality observed in recent years, particularly in younger people.1 Thus, prevention, which is constantly evolving, should be a priority. This review presents an update of the main prevention measures aimed at patients with a prior ACS, focusing on the main developments of the last year.
SECONDARY PREVENTION STRATEGIES FOR ACUTE CORONARY SYNDROMEDevelopments in Risk Factor ControlObservational studies indicate that most recurrent cardiac events occur in survivors of an ACS, mainly within the first year of the ACS.2 For treatment of the acute phase of an ACS, dramatic advances have been made in patient care, reperfusion therapies, and medical treatment, which have considerably reduced in-hospital mortality. To further lower mortality and event recurrence in patients with a prior ACS, focus should be placed on optimizing secondary prevention therapies and treatment adherence among patients. In recent years, updates have been made to clinical practice guidelines on the treatment of myocardial infarction with and without ST-segment elevation,3,4 management of stable coronary disease,5 and strategies for the prevention or specific management of risk factors.6–10 All of these guidelines stress the importance of intensively treating risk factors. Both drug prescription and initiation of patient education should be performed during hospital admission, as patients tend to pay more attention to advice and recommendations in this setting. Moreover, treatment optimization has been shown to be less likely once patients are discharged. A study that reviewed treatments at discharge and after 1 year in 6748 patients with a myocardial infarction included in 2 American registries in 2003 and 200811 found that, although most patients were discharged with a prescribed secondary prevention recommendation (in this case, beta-blockers, angiotensin-converting enzyme [ACE] inhibitors, or angiotensin receptor blockers, and statins), only 1 in every 3 patient was within the suggested dosage target and only 25% of patients were prescribed an increae in dosage after discharge. Given that the protective effect of these medications is dose-related, failure to reach the target dose during admission or to increase it during patient follow-up is a limitation of prevention measures and, thus, treatment dose should be maximized before discharging patients that have had an ACS.
Lifestyle RecommendationsNonpharmacological secondary prevention measures are barely addressed in the European guidelines for the management of patients with myocardial infarction with or without ST-segment elevation or with stable coronary disease. In these guidelines, lifestyle and prevention recommendations are based on dyslipidemia management and cardiovascular disease prevention.8,12
DietA healthy diet reduces the risk of cardiovascular disease. The guidelines agree on the recommended approach: energy intake should be limited to the amount of energy needed to maintain or achieve an adequate body weight (body mass index < 25); saturated fat intake should be reduced (< 10% of the total fat consumed) and replaced with omega-3 polyunsaturated fatty acids, mainly derived from fish oil; 5 portions of fruit or vegetables a day and 3 of fish a week should be consumed; salt intake should be reduced to < 6g/day; alcohol consumption should be limited; and intake of nuts and cereals should be increased. The effectiveness of these recommendations has been demonstrated in the largest study performed to date, in which the Mediterranean diet supplemented with extra virgin olive oil or nuts reduced the incidence of serious cardiovascular events in patients at high risk of events but without previous cardiovascular disease.13
SmokingSmoking alters endothelial function, boosts cellular adhesion, and is a proinflammatory, prothrombotic, and prooxidative factor that promotes atherosclerosis and potentiates atherosclerotic plaque instability, for which it is even ascribed a proarrhythmogenic role. Patients with ACS who are smokers have double the probability of recurrent ischemic events than nonsmokers, indicating that smoking has a considerable prothrombotic effect. Observational studies demonstrate that patients who quit smoking have lower mortality in subsequent years than those who continue to smoke,14 showing that smoking cessation is potentially the most effective measure of all secondary prevention strategies and that considerable effort should be dedicated to achieving this objective. Patients should be offered advice, group therapy, or treatment combinations, such as nicotine replacement therapy, varenicline, or bupropion.
Interesting data appeared in 2013 in the results of the PARADOX study15 regarding smoking and cardiovascular disease In this study, the effectiveness of clopidogrel monotherapy in patients with atherothrombotic disease varied depending on whether the patient smoked or not. The authors compared platelet reactivity between smokers and nonsmokers (never smokers or former smokers) who were taking clopidogrel or prasugrel. In nonsmokers taking clopidogrel, its metabolite was less active, resulting in greater platelet reactivity. The situation differed in patients taking prasugrel, as their platelet reactivity was lower, regardless of whether they smoked or not. Following the publication of this study, other cohorts, such as that of the CAPRIE study,16 were analyzed, showing the same smoking-dependent differential effect of clopidogrel. Although smokers have a higher risk of events than former or never smokers, clopidogrel therapy was associated with a reduction in ischemic events in smokers; this benefit was not seen vs: acetylsalicylic acid (ASA) in nonsmokers or former smokers. These findings indicate that clopidogrel can offer better protection against ischemic events and is superior to ASA in smokers with cardiovascular disease on antiplatelet monotherapy. Moreover, given that not all patients manage to quit smoking, despite advice, these results allow the establishment of more effective secondary prevention in patients who continue smoking and selection of ASA monotherapy for nonsmoking patients and clopidogrel monotherapy for smokers, once dual antiplatelet therapy is completed.
HypertensionThe main developments in hypertension management are reflected in updates to the European guidelines, published in 2013,10 and the American (Eighth Joint National Committee)17 guidelines. Treatment targets have been simplified in both guidelines, and blood pressure targets are fixed at < 140/90mmHg for almost all situations, with some exceptions, such as for diabetes mellitus and advanced age. The 5 main drug groups (diuretics, beta-blockers calcium antagonists, ACE inhibitors, and angiotensin receptor blockers) can be used for treatment initiation or maintenance, alone or in combination. These recommendations are also applicable to hypertensive patients with a prior ACS, with the exception that beta-blockers should be used in these patients. The recent American hypertension guidelines17 go further and recommend blood pressure control targets of < 150/90mmHg for those aged ≥ 60 years, only keeping the target of 140/90mmHg for those patients < 60.
HypercholesterolemiaTreatment targets have changed with the release of a new American hypercholesterolemia guideline7 and a more recent cardiovascular prevention guideline of the Joint British Societies.6 The American guidelines have removed the target treatment values. This recommendation is due to the lack of evidence to support the practice of progressively increasing statin dosage to achieve a specific target of low-density lipoprotein cholesterol (LDL-C) or non–high-density lipoprotein cholesterol (non–HDL-C) (obtained by subtracting HDL-C from total cholesterol), as the evidence comes from clinical studies designed with moderate- and high-intensity fixed-dose statin therapy. The British guidelines also recommend beginning secondary treatment with high-dose statin therapy dosin all patients without contraindications and irrespective of baseline cholesterol levels. However, this guideline maintains the ideal LDL-C and non–HDL-C values that should be achieved with treatment. Moreover, non–HDL-C is preferentially used as a treatment target, as the evidence shows that this parameter has a greater association with risk and treatment response than LDL-C, particularly in patients with type 2 diabetes mellitus in whom increased levels of atherogenic particles are not reflected in their LDL-C concentration. Finally, all patients with established cardiovascular disease should be treated during hospital admission with high-dose statins, regardless of their non–HDL-C values. The statin of choice is 80mg atorvastatin and the targets are non–HDL-C < 100mg/dL or LDL-C < 70mg/dL.
A new field is opening up in the treatment of hypercholesterolemia with the development of a new class of drugs that significantly reduces cholesterol concentrations. This treatment involves monoclonal antibodies directed against proprotein convertase subtilisin/kexin type 9, a protease that binds to the hepatic receptor of LDL and promotes its degradation, thereby inhibiting its action and reducing hepatic LDL receptor turnover, which improves LDL uptake and elimination. The following advantages are obtained: its action does not involve cholesterol synthesis, eliminating the secondary hepatic and muscular effects of statins, and it is subcutaneously administered every 2 to 4 weeks. Currently, clinical trials have begun with 3 molecules: evolocumab (Amgen),18 alirocumab (Regeneron Pharmaceuticals), and bococizumab (Pfizer). Three clinical studies of evolocumab have recently reported favorable results. In the DESCARTES study19 of patients recently diagnosed with hypercholesterolemia, evolocumab 420mg every 4 weeks was compared with placebo (added to the baseline statin therapy). Evolocumab therapy significantly reduced cholesterol (by 49% in those treated with high-dose statins and by 62% in patients treated with low-dose statins). Similar reductions were achieved in another 2 studies with this molecule in patients with mixed hyperlipidemia (LAPLACE-2 study [LDL-C Assessment with PCSK9 MonoclonaL Antibody Inhibition Combined with Statin ThErapy-2]) and with statin intolerance (GAUSS-2).20 In the second study, ezetimibe reduced LDL by about 37% to 39% in patients with statin intolerance, whereas evolocumab reduced LDL by between 55% and 56%. Although these results are promising, we must wait until the end of the FOURIER (Further Cardiovascular Outcomes Research With PCSK9 Inhibition in Subjects With Elevated Risk) study in which evolocumab vs placebo is being added to statin therapy in 22 500 patients to reduce the primary composite endpoint of cardiovascular death, myocardial infarction, hospitalization with unstable angina, stroke, or coronary revascularization. The results of the study are expected in 2018.
Developments in Antiplatelet Therapy Following Acute Coronary SyndromeAfter an ACS, indefinite antiplatelet therapy with low-dose ASA (75-100mg) is the drug treatment of choice; clopidogrel (75 mg) is the alternative for patients with ASA intolerance. As dual therapy with ASA, the latest European and American guidelines firmly support the new P2Y12 receptor inhibitors, and clopidogrel is reserved for patients who cannot receive ticagrelor or prasugrel (IA recommendation). This recommendation is justified by detailed examination of the results of the TRITON TIMI-3821 and PLATO22 studies, which showed the superiority of prasugrel and ticagrelor, respectively, vs clopidogrel.
Various studies have analyzed the optimal duration of dual antiplatelet therapy. In a meta-analysis of 4 clinical trials that included 8231 patients who underwent an angioplasty with a drug-eluting stent (61% following an ACS), extending dual antiplatelet therapy duration beyond 12 months significantly increased the risk of severe bleeding without reducing mortality, myocardial infarction, or stroke, vs control (3–12 months of dual antiplatelet therapy).23 More definitive data regarding the optimal duration of dual antiplatelet therapy following an ACS will be provided by the DAPT (Dual Antiplatelet Therapy) study,24 which has included 26 000 patients treated with metallic or drug-eluting stents and with dual antiplatelet therapy. At 12 months, patients without events were randomized to placebo or continued with thienopyridine for 18 additional months. The estimated completion date for the study is May 2014.
The European ACS guidelines3–5,25–27 continue to recommend dual antiplatelet therapy for 12 months for ACS with and without ST-segment elevation and irrespective of coronary stent implantation. However, the recent guidelines of the Joint British Societies,6 although also recommending 12 months of therapy following an ACS, establish a minimum duration of 1 month for patients treated with a conventional metallic stent and 6 months for those treated with a drug-eluting stent.
A new development that has been tested in antiplatelet strategies involves drugs that inhibit the platelet thrombin receptor, although a clear benefit remains to be found as one such drug, vorapaxar, failed to reduce ischemic events and increased rates of bleeding.28,29
Anticoagulant TherapyThe ATLAS ACS 2-TIMI 51 study30 analyzed the addition of low-dose rivaroxaban to dual antiplatelet therapy (mainly ASA with clopidogrel) in patients with a prior ST-segment elevation myocardial infarction. The rivaroxaban dose that optimized the benefit/risk ratio was 2.5mg/12h, with a reduction in cardiovascular mortality vs placebo (2.5% vs 4.2%), although with an increase in severe bleeding rates, including intracranial hemorrhage (0.6% vs 0.1%).
Other Drugs Used in Secondary Prevention- •
Beta-blockers. Evidence supports treatment with beta-blockers for up to 1 year as secondary prevention following an ST-segment elevation myocardial infarction, but there is no available evidence in other patient groups or for a longer duration. For patients with ventricular dysfunction or heart failure, beta-blockers are indicated with ACE inhibitors/angiotensin receptor blockers and aldosterone antagonists.
- •
ACE inhibitors/angiotensin receptor blockers. The value of these drugs as a secondary prevention measure for reducing cardiovascular events is controversial in patients without heart failure. A recent meta-analysis31 that analyzed 26 randomized studies containing a total of 108 212 patients without heart failure found that treatment with ACE inhibitors or angiotensin receptor blockers reduces the combined risk of cardiovascular death, myocardial infarction, and stroke, but ACE inhibitors are the drugs of choice.
- •
Colchicine. The usefulness of colchicine for the prevention of cardiovascular events has been demonstrated in patients with stable coronary disease.32 Treatment with colchicine 0.5mg/day together with antiplatelets, statins, and other secondary prevention measures reduced the composite endpoint of ACS, out-of-hospital cardiac arrest, or ischemic stroke (5.3% vs 16%).
In the guidelines, rehabilitation/prevention programs are recommended for patients at moderate-to-high risk or those with multiple risk factors. The value of these programs is sufficiently demonstrated, but the availability of cardiovascular rehabilitation units is generally low in Spain.33 Of all of the secondary prevention recommendations after an ACS, cardiac rehabilitation displays the lowest adherence, despite having shown reductions of 41% in mortality and of 32% in rehospitalizations.34 The benefit is also economic, because rehabilitation saves 30 500 euros per patient in the first year (predominantly due to a faster return to work) and up to 14 500 euros per year and per patient in subsequent years.
CONCLUSIONSFor patients with an ACS, effective treatments are currently available, which have managed to drastically decrease mortality in the acute phase; however, optimization of those secondary prevention treatments that have demonstrated a risk reduction is prudent (Table). To achieve a greater risk reduction, attention must be paid to prevention measures and particularly to the development of cardiac rehabilitation programs, which are currently the least used measures, despite their clear benefits.
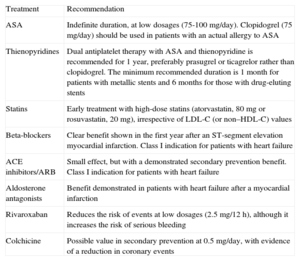
Summary of the Main Secondary Prevention Drugs
| Treatment | Recommendation |
| ASA | Indefinite duration, at low dosages (75-100 mg/day). Clopidogrel (75 mg/day) should be used in patients with an actual allergy to ASA |
| Thienopyridines | Dual antiplatelet therapy with ASA and thienopyridine is recommended for 1 year, preferably prasugrel or ticagrelor rather than clopidogrel. The minimum recommended duration is 1 month for patients with metallic stents and 6 months for those with drug-eluting stents |
| Statins | Early treatment with high-dose statins (atorvastatin, 80mg or rosuvastatin, 20 mg), irrespective of LDL-C (or non–HDL-C) values |
| Beta-blockers | Clear benefit shown in the first year after an ST-segment elevation myocardial infarction. Class I indication for patients with heart failure |
| ACE inhibitors/ARB | Small effect, but with a demonstrated secondary prevention benefit. Class I indication for patients with heart failure |
| Aldosterone antagonists | Benefit demonstrated in patients with heart failure after a myocardial infarction |
| Rivaroxaban | Reduces the risk of events at low dosages (2.5 mg/12 h), although it increases the risk of serious bleeding |
| Colchicine | Possible value in secondary prevention at 0.5 mg/day, with evidence of a reduction in coronary events |
ACE, angiotensin-converting enzyme; ARB, angiotensin receptor blockers; ASA: acetylsalicylic acid; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol.
None declared.
Section sponsored by AstraZeneca