The Working Group on Cardiac Catheterization and Interventional Cardiology presents its yearly report on the data from the registry of the activity in Spain corresponding to 2013.
MethodsThe centers introduce their data online voluntarily and the information is analyzed by the Steering Committee of the Working Group on Cardiac Catheterization.
ResultsIn 2013, 104 hospitals sent their data (72 public centers and 32 private). In all, 136 715 diagnostic studies were performed (120 358 coronary angiograms), with a slight decrease with respect to 2012, a reduction that was also observed in the rate, which was 2944 diagnostic studies per million population. A total of 65 912 interventional procedures were carried out during a phase of stability, for a rate of 1419 interventions per million population. Other techniques included the implantation of 99 417 stents and 1384 biodegradable intracoronary devices (64% of them drug-eluting devices). There were 18 337 procedures in acute myocardial infarction, for an increase of 7% with respect to 2012 and representing 27.8% of all the percutaneous coronary interventions. Radial access was the approach used in 71% of the diagnostic procedures and in 65% of the interventional procedures. The performance of renal denervation has nearly doubled with respect to 2012. For the first time, more than 1000 transcatheter aortic valve implantation procedures were carried out in 1 year, although the frequency increased only slightly (23%).
ConclusionsThere continued to be a slight increase in the activity in cardiac catheterization in association with ST-segment elevation myocardial infarction, whereas, with the exception of recently introduced, highly specific procedures, the use of the remainder of the procedures, among them transcatheter aortic valve implantation, leveled off.
Keywords
This year, in keeping with the custom that has been repeated each year since 1990, one of the most important tasks of the Steering Committee of the Working Group on Cardiac Catheterization and Interventional Cardiology was to gather data on the activity of as many cardiac catheterization laboratories as possible, for the purpose of preparing the annual registry of their activity. In recent years, the collection of these data has continued to improve little by little,1–22 greatly aided by their entry online. The data are cleaned by members of the steering committee and by all members of the working group, as the preliminary data are presented at their annual meeting, held this year on June 12th and 13th in Córdoba, in southern Spain.
The existence of an annual report on the activity in this area primarily enables the analysis of the changes from one year to another, an important aspect in that it reveals the extent of the implementation of percutaneous techniques in Spain. The analysis by hospital and by autonomous community establishes a framework for comparing the differences in the activity in absolute and relative terms, once they have been corrected for the population in each autonomous community, as established by census. Admitting the limitations of a registry based on voluntary activity reporting, the information obtained provides us with an overview of the situation in Spain, and enables us to relate it to that of other countries and evaluate the development of interventional cardiology in the different Spanish autonomous communities. Free access to these data helps us to map the distribution of the resources and evaluate the different trends in the use of diagnostic and therapeutic procedures.
Although, in general, the performance of percutaneous coronary intervention (PCI) has leveled off in recent years, changes have been detected in some of the variables included in the data collection. The most outstanding finding is the marked increase in the use of procedures performed in the setting of acute myocardial infarction (AMI) and under the European initiative, Stent for Life,23 the objective of which is to improve delivery of care in myocardial infarction, and which includes Spain as one of its “target” countries.24 Finally, the increase recorded in the use of transcatheter aortic valve implantation in recent years has shown an evident stagnation, both in the number of units implanted and in the number of centers at which this technique is being carried out.
This article presents the 23rd report on interventional activity in Spain and compiles the data from all the public hospitals and a significant number of private centers.
METHODSWe collected data on the diagnostic and cardiac interventional activity of the majority of Spanish hospitals. Data collection was voluntary and was not audited. In the case of conflicting data or values outside the trend observed in recent years in a given center, the responsible researcher at that center was consulted for the reevaluation of these data. Data were collected using a standard electronic questionnaire, accessible from the website of the Spanish Society of Cardiology Working Group on Cardiac Catheterization and Interventional Cardiology, to be completed online. The working group's steering committee analyzed the information obtained, in collaboration with the Persei group. The results are made public in this article, although a preliminary draft was presented as a slideshow at the working group's annual meeting.
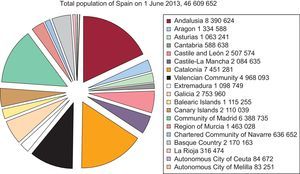
The calculations involving the population of Spain as a whole and that of each autonomous community were based on the estimates of the population of the Spanish National Institute of Statistics up to 1 June 2013, as published on its website.25 The Spanish population was estimated at 46 609 652 inhabitants (Figure 1). As in the immediately preceding years, the number of procedures per million population for the country as a whole were calculated on the basis of the overall population. This year, once again, the true number of coronary angiograms per million population was taken into account. This datum, rather than diagnostic procedures per million population, is comparable to the European recommendations and averages.
RESULTSInfrastructure and ResourcesA total of 104 hospitals that performed interventional procedures in adults participated in the present registry (5 fewer than the year before); this decrease occurred among private centers (Appendix). Data were received from 100% of the 72 public hospitals and from 32 (22%) private centers (of a total of 148). This represents a substantial segment of the activity carried out in Spain, in which the majority of the volume is attributable to centers with public funding. There are 206 catheterization laboratories, 138 (67%) of which are exclusively for cardiac catheterization and 53 (26%) have shared activity.
With regard to personnel, the 104 centers reported a total of 476 physicians involved in interventional activity in 2013 (355 of them accredited). Concerning the nursing staff, there were 560 registered nurses and 81 radiology technicians.
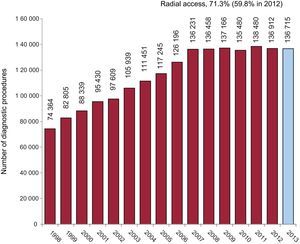
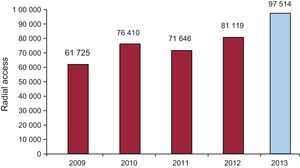
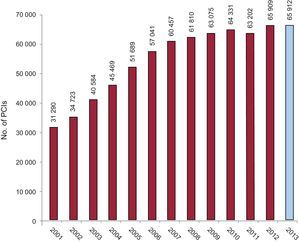
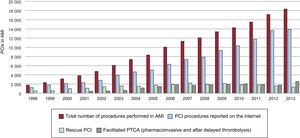
Diagnostic ProceduresA total of 136 715 diagnostic studies were carried out in 2013, a number that represents an imperceptible decrease of 0.1% with respect to the preceding year (Figure 2). Of these procedures, 120 358 were coronary angiograms, practically the same number as in 2012. It is notable that 97 514 diagnostic procedures involved radial artery access, representing 71.3% of the procedures. This approach is exhibiting very constant growth in recent years (Figure 3), with an especially relevant increment of 11.5% recorded between 2012 (59.8%) and 2013 (71.3%). On the national level, the average number of diagnostic studies in Spain in 2013 was 2944 procedures per million population, slightly lower than in preceding years when it was always reported as coronary angiograms per million population. Actually, coronary angiograms account for only 2592 per million population of all the diagnostic studies (2621 in 2012), much lower than the European estimates as early as 2006.25Figure 2 shows the numbers of diagnostic procedures performed each year in Spain since 1998.
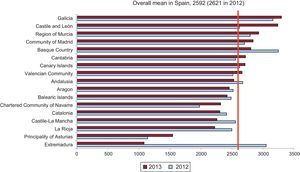
Figure 4 is a graph showing the distribution of diagnostic coronary angiograms per million population in each Spanish autonomous community. The mean was 2592 per million population, slightly lower than that recorded in 2012 (2621 coronary angiograms per million population).
Regarding the diagnostic activity by center, 58 carried out more than 1000 coronary angiograms (1 more than in 2012) and 17 performed more than 2000 (1 more center than the preceding year). An average of 1314 diagnostic procedures were carried out per center, a rate very similar to that of recent records.18–22
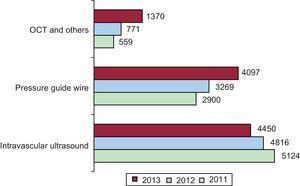
With respect to intracoronary diagnostic techniques, there is even a reduction in the use of intravascular ultrasound, although it is still the most widely employed approach. The use of the pressure guide wire continues to increase steadily –in 2013, considerably (25%), surpassing 4000 procedures in 1 year for the first time. The greatest percent increase is that reported for optical coherence tomography, which consolidated a substantial growth of 77.6% in 2013. Figure 5 shows the changes in the numbers of the different intracoronary diagnostic techniques with respect to the preceding 2 years.
Percutaneous Coronary InterventionsThe number of PCIs (65 912) remained very similar to that of the preceding year, despite there being reports from 5 fewer centers, thus consolidating the increase in 2012 with respect to 2011 (65 909 in 2012). The changes in the use of PCI over time are shown in Figure 6. The number of PCIs per million population was 1419 (vs 1434 in 2012 and 1373 in 2011). All the centers with diagnostic activity also offered PCI.
The ratio of PCI to coronary angiography remained at 0.55 (as it was in 2012; it was 0.51 in 2011). In 2013, 30% of the procedures were performed for multivessel disease (24.8% of all PCI in 2012), a circumstance that does not mean that more than one lesion was treated in the same procedure; there were no differences in the number of procedures performed ad hoc during diagnosis (74%).
Once again, the use of radial access in PCI increased (by 4.2%), for a prevalence of 64.4%, somewhat lower than that recorded in diagnostics.
The number of procedures involving unprotected left main coronary artery grew, with 2202 interventions in 2013 (1810 in 2012 and 1828 in 2011), and represented 3.3% of all PCIs (2.7% in 2012). This is probably a result of the publication of studies with long-term clinical follow-up showing a good outcome in the patients randomized to PCI if the disease has not spread to the rest of the coronary tree.
The registry includes 2751 procedures (3.9% of all PCIs) to treat lesions that the operator had considered to be chronic total occlusions. Adjuvant drug therapy consisting of glycoprotein IIb/IIIa inhibitors and antithrombotic agents (other than unfractionated heparin) was used in 18.3% of the procedures; the agents most widely employed were abciximab (in 10% of the PCI) and bivalirudin (in 5.4%).
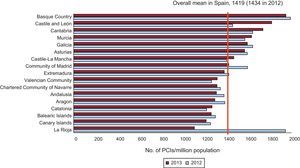
The distribution of the 1419 PCIs per million population in Spain by autonomous community is shown in Figure 7. With regard to the distribution by center, as usual, it is bimodal. At 25 centers, fewer than 250 PCIs are performed each year; a large number of the private institutions are in this category. At 47 centers, between 500 and 1000 are carried out annually. In 2013, there were still 18 high-volume centers, the same as in 2012.
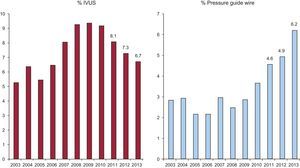
Once again, the intracoronary diagnostic techniques (intravascular ultrasound and the pressure guide wire), used mainly in the evaluation of the severity of intermediate lesions or of the outcome of the intervention, moved in clearly opposite directions; intravascular ultrasound was used in 6.7% of the interventions (a reduction of 7.6% with respect to 2012), whereas use of the guide wire increased to 6.2%, for a highly respectable increment of 25% (Figure 8).
In 2013, for the first time, the registry introduced immediate outcome variables in PCI, which were filled out in 71% of the cases. In all, 98% of the procedures (including those performed in AMI) were considered to result in final angiographic success with no complications; severe complications (death, AMI, or the need for emergency cardiac surgery) were reported in 1.2% and death during the procedure in only 0.5%.
StentsThe implantation of 99 417 units was recorded in 2013, 307 more than in 2012, although we understand that this variable is highly dependent on the total number of centers that report their data. After 2 stable years, the ratio of stents per patient increased very slightly, from 1.5 to 1.51 (1.56 in 2010 and 1.63 in 2009). It may seem that the prevalence of the use of the drug-eluting stent remains completely stable at 61.5% (61.8% in 2012), corresponding to 61 120 units, but we should remember that this is a pure ratio of the total number of drug-eluting stents to the total number of stents, and that fully biodegradable devices (1384 devices reported in 2013) represented 2.1%. Thus, in a strict sense, the total prevalence of drug-eluting devices would reach 63.6% (the percentage implanted in each autonomous community is provided below). With respect to the use of self-expanding intracoronary devices and those specifically designed for the treatment of bifurcations, neither differed much with respect to the preceding year, with 79 and 267 procedures, respectively. The prevalence of direct stent implantation was nearly 30%, as in previous years, similar to the findings in recent studies or data sets dealing with “real world” lesions.26
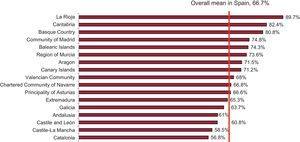
The implementation of drug-eluting stents continued to show wide differences among autonomous communities. Given that, in some of the communities with fewer centers, the lack of data on drug-eluting stents may have a great impact on the ratio in that community, we have attempted to debug or clean this datum, eliminating from the calculation those centers that did not provide details on this variable. This would explain the fact that the overall mean is 66.7% (in our opinion, closer to reality). Communities like La Rioja, Cantabria, and the Basque Country are among those in which the rate of utilization is highest (> 80%) and Castile-La Mancha and Catalonia, those in which the use was least prevalent (< 60%) (Figure 9).
Distribution of antiproliferative drug-eluting stents as a percentage of the total number of stents implanted according to autonomous community. The percentage was calculated by taking the ratio of the number of coated stents (drug-coated) to the total number of procedures. Data from hospitals that included the total number of stents but not that of drug-eluting stents were excluded.
The use of rotational atherectomy increased slightly in 2013, with 1254 cases (1194 in 2012 and 1225 in 2011), distributed among 71 centers. There were no reports of cases of directional atherectomy or intracoronary brachytherapy, techniques that have fallen into disuse and will be excluded from the registry from now on. The use of the cutting balloon was somewhat more common, with 2103 cases (1982 in 2012 and 1916 in 2011), although the model of scoring balloon was not specified. The continued increase in the use of thrombectomy catheters was also recorded, although it was less marked, with 9370 cases, 3.6% more than in 2012 (9041 cases), despite the publication of studies in which the results of thrombus aspiration were negative.27 Our findings indicate that these devices were employed in 67% of primary PCIs.
Percutaneous Coronary Interventions in Acute Myocardial InfarctionThe 18 337 PCIs performed in patients with AMI is a further increase of 7% with respect to 2012 (17 125). As of 2013, they represented 27.8% of all PCIs. In all, 11 258 (61.4%) of these procedures involved radial access, vs 56% in 2012 and 49% in 2011.
Within the range of PCI strategies employed in the acute phase of AMI, this year we differentiated between angioplasty performed immediately (671 cases) and that carried out 3hours to 24hours after the administration of fibrinolytic therapy (1902 cases), as they are conceptually different, as is the case of rescue angioplasty (1359 cases). Thus, although the sum of the modes in which therapy is provided shows a clear increase and rescue, a slight reduction, there may be a relationship with this redefinition of the variables. In any case, the strategy that continues to grow, although less markedly, is primary angioplasty, with 13 899 cases (up from 11 766 in 2011 to 13 690 in 2012). Primary PCI represents 21% of all angioplasty procedures and 76% of all PCIs performed in AMI (Figure 10).
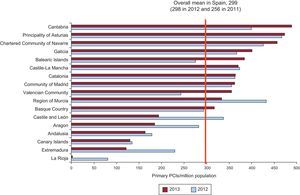
The distribution of PCI in AMI according to Spanish autonomous community shows a pattern similar to that of previous years; nevertheless, we should not fail to point out that the best data are reported by communities that have an organized program of continuous care in AMI. Thus, those that recently have adopted one have improved their position, whereas some communities with few centers and problems with data collection are highly sensitive to changes with respect to preceding years, and these are difficult to interpret (Figure 11).
Regarding the number of procedures per center, 44 reported the performance of more than 200 PCIs in AMI per year (5 more than in 2012), whereas 23 reported fewer than 50 (1 less than in 2012).
Noncoronary Interventions in AdultsThe records show a reduction in the use of aortic valvuloplasty with respect to 2012 (258 cases in 2012 and 201 in 2013); although the cases of mitral valvuloplasty also decreased from 254 in 2012 to 240 in 2013, it continues to be the procedure most frequently performed. In 2013, transcatheter aortic valve implantation surpassed the barrier of 1000 interventions (n=1041). Its growth is slow: there were 426 cases in 2009, 655 in 2010, 770 in 2011, and 845 in 2012. Of the latter group, 448 interventions were performed with self-expanding prostheses, 590 with balloon-expandable prostheses, and 3 with other techniques.
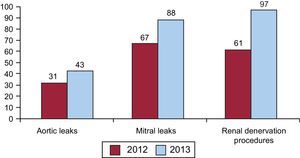
The numbers of patients treated for adult congenital heart disease were very similar to those of preceding years, with 293 closures of atrial septal defects (292 cases in 2012), whereas patent foramen ovale closure was performed in 201 cases (265 in 2010, 195 in 2011, and 188 in 2012). It is surprising that there was a reduction in other closure procedures, such as that involving left atrial appendage, when compared to 2012, with only 43 procedures. We should point out the increase in closure of paravalvular leaks, both mitral (88 cases, 67 in 2012) and aortic (43 cases; 31 in 2012), in accordance with the extensive experience of Spanish groups.28–30 Finally, it is important to note that renal denervation was carried out in 97 cases, an increase over the 61 procedures in 2012, despite the fact that the results of the Symplicity HTN-2 trial31 have yet to be made known (Figure 12).
DISCUSSIONThe majority of the activity reported in 2013 continued to show a clear leveling off in certain percutaneous techniques, both diagnostic and interventional. However, expansion was observed in some areas: constant growth was confirmed in the area of angioplasty (especially primary) in the management of AMI, and in the adoption of certain techniques such as closure of paravalvular leaks and renal denervation. As a diagnostic and interventional aid, there was a notable increase in the use of the pressure guide wire, as opposed to intravascular ultrasound, which continued to lose ground with respect to other imaging techniques, such as optical coherence tomography. Concerning coronary devices, there were signs of an incipient but growing use of biodegradable devices and a slight trend toward an increase in the use of drug-eluting stents. The trend in transcatheter valve implantation maintained a level of growth which, while modest, was greater than in 2012.
With respect to European standards, Spain continued to rank below average in the numbers reported for many techniques, a circumstance that is especially striking in the case of PCIs per million population and transcatheter aortic valve implantation, which leveled off at rates per patient that were markedly lower than in the rest of Europe.32
Diagnostic activity continued to decrease slightly; however, perhaps a more eloquent finding is the fact that the analysis of the data revealed that the true rate was 2592 coronary angiograms per million population, clearly far below the most recently published European data which set this level at 4030 per million, but referred to the rate for 2005.33 With respect to the interventional activity, a certain stabilization is detected in the overall number, but this is due to the sustained growth in interventional procedures in AMI which, in 2013, increased by 7% with respect to 2012. In contrast to preceding years, in which it seemed that the number of cases of “complex” percutaneous coronary revascularization had leveled off, in 2013 there was an increase in the cases requiring percutaneous treatment of unprotected left main coronary artery, probably influenced by studies showing promising results.34–37 In contrast, the number of stents implanted, the stent to patient ratio, and the number of special devices used in cases of this type, such as rotational atherectomy or the cutting balloon, are highly stable. The publication of the FREEDOM trial34 and the presentation of the long-term results of the SYNTAX trial,35 published in 2013,36 have probably discouraged the treatment of multivessel disease in patients with complex anatomy, especially diabetics. A more widespread use of the pressure guide wire has also been reported, probably for decision-making, as recommended by the FAME study,38 a circumstance that may reduce both the number of PCIs and the number of lesions treated and of stents used. The implementation of long stents (> 30mm) in cardiac catheterization laboratories may also have contributed to maintaining a low ratio of stents to patient.
Despite the increase in emergency interventional procedures in myocardial infarction in Spain, we continue to be far from the rest of Europe in terms of intervention rates per population, since the 1419 PCIs per million population is far below the most recently published European data (1601 PCIs per million population in 2005).33
Perhaps one of the most encouraging statistics revealed by the registries in recent years, especially this version corresponding to 2013, is the improvement in the number of primary PCI procedures, which is clearly related to the application of the Stent for Life initiative of the European Society of Cardiology.23 Another notable aspect is the fact that 60% of the emergency interventional procedures involve radial access.
Although transcatheter aortic valve implantation has grown less than expected, for the first time more than 1000 of these interventions were performed in a single year.
LimitationsFrom the moment of its conception, the registry has been voluntary and there are no obligatory variables, a fact that may influence the interpretation of the data. The risk of biases derived from a partial completion of some of the variables of the registry cannot be ruled out.
CONCLUSIONSIn 2013, despite the general persistence of a leveling off, there have been some interesting changes in the numbers of both the diagnostic and therapeutic procedures. The use of angioplasty, especially primary, in AMI continues to show progressive growth, both through the incorporation of more autonomous communities into primary PCI programs and because of the marked increase in the number performed in certain centers. The Stent for Life program, a priority objective for both the European Society of Cardiology and the Spanish Society of Cardiology, as well as our own working group, may have helped to improve care for coronary patients, but the numbers show that there is still a long way to go.
There remain differences between autonomous communities with regard to coronary interventional procedures, particularly those involving myocardial infarction, as well as in the use of drug-eluting stents.
With respect to noncoronary interventional procedures, the use of transcatheter aortic valve implantation continues to grow, albeit slowly, and the treatment of paravalvular leaks and the technique of renal denervation show significant increases.
CONFLICTS OF INTERESTNone declared.
The Steering Committee of the Working Group on Cardiac Catheterization and Interventional Cardiology wish to thank the directors and staffs of cardiac catheterization laboratories all over Spain, as well as those responsible for data collection, for their work.
| Public centers | Private centers | |
| Andalusia | Complejo Hospitalario Torrecárdenas | Hospiten Estepona |
| Complejo Hospitalario Universitario de Jaén | Clínica El Ángel | |
| Complejo Universitario Carlos Haya | ||
| Hospital Clínico Universitario Virgen de la Victoria | ||
| Hospital Universitario San Cecilio | ||
| Hospital de Jerez de la Frontera | ||
| Hospital Juan Ramón Jiménez | ||
| Hospital Universitario de Valme | ||
| Hospital Universitario Puerta del Mar | ||
| Hospital Universitario Puerto Real | ||
| Hospital Universitario Reina Sofía | ||
| Hospital Universitario Virgen de las Nieves | ||
| Hospital Universitario Virgen del Rocío | ||
| Hospital Universitario Virgen Macarena | ||
| Aragon | Hospital Clínico Universitario Lozano Blesa | |
| Hospital Universitario Miguel Servet | ||
| Principality of Asturias | Hospital Central de Asturias | Centro Médico de Asturias |
| Hospital de Cabueñes | ||
| Cantabria | Hospital Universitario Marqués de Valdecilla, Santander | |
| Castile and León | Hospital Clínico Universitario de Salamanca | |
| Hospital Clínico Universitario de Valladolid | ||
| Complejo Asistencial Universitario de León (CAULE) | ||
| Hospital Universitario de Burgos | ||
| Castile-La Mancha | Hospital General de Ciudad Real | |
| Hospital General Universitario de Albacete | ||
| Hospital General Universitario de Guadalajara | ||
| Hospital Virgen de la Salud | ||
| Catalonia | Ciutat Sanitària i Universitària de Bellvitge | Centre Cardiovascular Sant Jordi |
| Hospital Clínic i Provincial de Barcelona | Hospital General de Catalunya | |
| Hospital de la Santa Creu i Sant Pau | Hospital Quirón Barcelona | |
| Corporació Sanitària Parc Taulí | Hospital Universitari Mútua de Terrassa | |
| Hospital General Universitari Vall d’Hebron | Hospital Universitario Quirón-Dexeus | |
| Hospital Universitari Dr. Josep Trueta | ||
| Hospital Universitari Germans Trias i Pujol | ||
| Hospital Universitari Joan XXIII | ||
| Hospital Universitario Arnau de Vilanova de Lérida | ||
| Valencian Community | Hospital Clínico Universitario de Valencia | Clínica Medimar, Alicante |
| Hospital de la Ribera, Alzira | Hospital Clínica Benidorm | |
| Hospital General de Alicante | Hospital del Vinalopó-UTE Torrevieja | |
| Hospital de Denia | Hospital IMED Elche | |
| Hospital General de Castellón | Hospital IMED Levante-Benidorm | |
| Hospital General Universitario de Elche | Hospital Perpetuo Socorro | |
| Hospital General Universitario de Valencia | Hospital San Jaime Torrevieja USP | |
| Hospital Universitario Dr. Peset | ||
| Hospital Universitario La Fe | ||
| Hospital Universitario San Juan de Alicante | ||
| Extremadura | Hospital de Cáceres | |
| Hospital Universitario Infanta Cristina | ||
| Galicia | Complexo Hospitalario Universitario A Coruña | |
| Complexo Hospitalario Universitario de Santiago | ||
| Complexo Hospitalario Universitario de Vigo | ||
| Balearic Islands | Hospital Universitario Son Espases | Clínica Juaneda |
| Clínica Rotger | ||
| Clínica USP Palmaplanas | ||
| Policlínica Miramar | ||
| Canary Islands | Hospital de Gran Canaria Dr. Negrín | |
| Hospital Universitario de Canarias, Tenerife | ||
| Hospital Universitario Insular de Gran Canaria | ||
| Hospital Universitario Nuestra Señora de Candelaria | ||
| Hospiten Rambla | ||
| Community of Madrid | Hospital Central de la Defensa Gómez Ulla | Clínica Nuestra Señora de América |
| Hospital Clínico San Carlos | Hospital La Moraleja (SANITAS) | |
| Hospital de Torrejón | H. Madrid Montepríncipe y Sanchinarro | |
| Hospital Universitario La Paz | Sanatorio La Milagrosa | |
| Hospital General Universitario Gregorio Marañón | ||
| Hospital Puerta de Hierro | ||
| Hospital Ramón y Cajal | ||
| Hospital Universitario 12 de Octubre | ||
| Fundación Jiménez Díaz | ||
| Hospital Universitario de la Princesa | ||
| Hospital Universitario Fundación Alcorcón | ||
| Region of Murcia | Hospital Universitario Santa María del Rosell | Hospital San Carlos, Murcia |
| Hospital Universitario Virgen de la Arrixaca | Hospital Virgen de la Vega | |
| Chartered Community of Navarre | Hospital de Navarra | Clínica Universidad de Navarra |
| Basque Country | Hospital de Basurto-Basurtuko Ospitalea | Clínica IMQ Zorrotzaurre |
| Hospital de Cruces | Policlínica Guipúzcoa | |
| Hospital de Galdakao-Usansolo | ||
| Hospital Txagorritxu | ||
| La Rioja | Complejo de Salud San Millán-Hospital S. Pedro |