The healthcare of patients with acute heart disease, especially if their condition is critical and involves an imminent threat to life, is a daily challenge for any hospital. Basic requirements for coping with these situations include a deep understanding of cardiac physiology, pathophysiology, and hemodynamics, as well as knowledge of the use of diagnostic tools such as echocardiograms and therapeutic measures, such as cardiovascular pharmacology and temporary pacemaker placement, and of the correct use of intra-aortic counterpulsation and ventricular assist devices, aspects that are all included in the training program designed for our specialty.1
In addition, from the organizational point of view, it seems logical that, during hospital stay, the management of the entire cardiologic process by a single service better ensures continuity of care, avoids delays and repeat examinations and, in short, is safer for the patient and more efficient for the system.
The objective of the present document is to analyze the current situation of acutely-ill and critically-ill cardiac patients in Spain and to define the official position of the Spanish Society of Cardiology (Sociedad Española de Cardiología [SEC]) with respect to their management, seeking excellence in patient care, teaching, and research, as the cardiologist is the specialist with the greatest responsibility for the attention they receive. We identify areas for improvement and proposals for change in order to make all the parties involved aware of this need, to safeguard excellence in training by promoting European accreditation in this subspecialty for interested cardiologists, and to work toward the progressive integration of acute and critical cardiovascular care (ACCC) units into cardiology departments.
HISTORY, CURRENT SITUATION, AND JUSTIFICATION OF THE POSITION OF THE SPANISH SOCIETY OF CARDIOLOGYThe changes that have taken place in cardiology in recent decades have been spectacular (probably more so than in any other medical specialty), necessitating a review old customs and habits. The mid-20th century witnessed the birth of coronary care units, whose only purpose was to treat the arrhythmias associated with acute myocardial infarction (AMI). It was during the 1970s that interest in the diagnosis and management of hemodynamic alterations developed, and pulmonary catheterization and aortic counterpulsation were introduced. In the 1980s, there was a change of paradigm, from “passive surveillance” and the treatment of complications to “highly active therapy”, which opts for early reperfusion and aims to limit the size of the AMI, initially using pharmacological methods and later early coronary interventional procedures. Taken together, all these measures have substantially reduced the number of early complications and markedly decreased the mortality rate.
As expected, the initial coronary care units evolved. The increase in the number of survivors of the complications of AMI, which, until then, had been fatal, led to the expansion of the duties of these units to include the care of patients with other heart diseases (acute heart failure, severe arrhythmias, decompensated valve disease, etc) or conditions that compromise intrathoracic circulation (especially those affecting the aorta and pulmonary thromboembolism), which require critical care. This greater diversity and complexity of cardiovascular diseases obliged the cardiologists of these units to become well versed in the management of support therapies such as mechanical ventilation, renal replacement, nutrition, and hypothermia. This converted the one-time coronary care units into ACCC units.
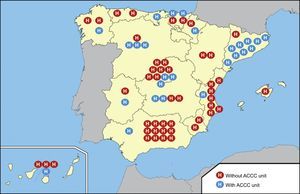
To prepare this document, we reviewed the situation in Spain in 2012, the last year for which there is published data on in-hospital mortality due to AMI in the hospitals participating in the RECALCAR (Recursos y Calidad en Cardiología [Resources and Quality in Cardiology]) registry (unpublished data from 2012). In accordance with the European consensus statement on the structure and organization of cardiac critical care units, it was established that a cardiology department be equipped with an ACCC unit when, systematically and without exception, it attends all cardiac patients requiring invasive mechanical ventilation. In 2012 (there have been certain changes since then), of the 72 cardiology departments accredited to train residents in our specialty, only 26 (36%) were responsible for an ACCC unit. The distribution of Spanish cardiology departments with ACCC units illustrates the marked geographic heterogeneity according to autonomous community (Figure).
While preparing this document, we analyzed the data of the RECALCAR registry (unpublished data from 2012 provided by Elola Asesores, Madrid, Spain) concerning the departments described above. From the point of view of patient care, the departments with ACCC units had greater activity, with a higher mean number of AMI discharges than the group without ACCC units (493 ± 158 vs 410±149; P=.03) and a higher number of medical residents per hospital per year (2.65±0.75 vs 2.07±0.89; P<.003). Thus, although they represented 36% of the cardiology departments that offered resident training, they accounted for 43% of the resident positions. The most striking finding of the analysis was that, in the centers where the cardiology department was in charge of the ACCC unit, the risk-adjusted in-hospital mortality due to AMI was significantly lower (6.96% vs 7.78%; P=.02). This reduction in the risk-adjusted mortality rate may be the first objective evidence of the benefits of these units.
This datum complements the finding of the first RECALCAR study,2 which did not analyze mortality according to the department responsible for the management of the acute phase of AMI. but according to which department arranged the hospital discharge. Discharge of AMI patients from areas other than the cardiology department was associated with a higher mortality rate. Together, these 2 factors support the idea that acutely ill cardiology patients benefit from integrated and continuous care provided by the cardiology department. The indispensable condition is that the excellence of patient care during the critical phase be guaranteed, which appears to have been clearly demonstrated in the departments currently responsible for providing that care.
From the teaching point of view, we wish to mention certain relevant data derived from the Cardio MIR survey,3 which was distributed among Spanish cardiology residents, who responded to it anonymously and voluntarily:
- •
Somewhat over one-third of the residents were never assigned to on-call duty in a cardiology-dependent ACCC unit during their entire training period.
- •
For one-fourth of them, it was not customary to be involved in the treatment of critical heart disease or acute coronary syndromes during their residency.
- •
Up to 16% of the residents reported that they never performed simple techniques that are indispensable in their training, such as temporary pacemaker insertion, central venous catheterization, or pericardiocentesis, during their residency. The distribution of the performance of techniques varied widely from one autonomous community to another and there was a certain parallelism with the distribution of ACCC units under the direction of cardiology departments.
These results clearly indicate that a considerable proportion of the cardiology residents in Spain does not receive the training considered necessary in this setting. Unfortunately, the survey makes no mention of the management of more advanced techniques (mechanical ventilation, extracorporeal renal replacement therapies, nutrition of critically ill patients, hypothermia, etc), but the necessary circumstances can be imagined if we extrapolate the aforementioned data on simpler techniques.
Thus, most critically ill cardiovascular patients in Spain are not treated by cardiologists and most Spanish residents are not trained in departments attending patients of this type. This situation is contrary to the recommendations of cardiology societies in Europe and the United States and to standard practice in many other western European countries.
Therefore, the SEC considers that patient care in acute and critical cardiovascular disease should be undertaken and headed by the specialists with the broadest knowledge and training in this field, that is, by cardiologists. The team should guarantee excellence in the management of each and every phase of the process in close collaboration with the department of intensive care medicine and with any other specialty related to the care of critically-ill patients (anesthesiology, nephrology, pulmonology, etc).
OBJECTIVES AND PROPOSALS FOR CHANGEThe need to adapt cardiology departments to the changes in the type and management of acutely-ill and critically-ill patients compels the SEC to manifest and pronounce its commitment to the following objectives:
- •
To increase awareness among all cardiologists that their mission is to undertake the diagnosis and treatment of all cardiac patients, especially those who are in the acute phase and a critical condition.
- •
To safeguard excellence in training in acute and critical cardiac care, developing the subspecialty for cardiologists in charge of patient care in ACCC units.
- •
To promote the integration of ACCC units into the cardiology departments. It is necessary that the cardiological process be headed in its entirety by the cardiology department, according to an established protocol and maintaining effective coordination among its different sections and with any other department in the hospital that may be necessary.
- •
As in any other area, to promote research in heart disease of this type.
The first key objective is that all cardiologists be made aware of this need. In this document, we have provided objective arguments in terms of both patient care and training. Senior cardiologists should acknowledge and accept that developments in cardiology necessitate the introduction of changes that were unforeseen when they began their training 2 or 3 decades ago. Convention and inertia should not hamper advances that aid in the management of the new type of patient. Young cardiologists should know that, if they do not come into contact with acutely-ill and critically-ill patients, they are cultivating less than 50% of their specialty and missing the part that may have the greatest influence on the natural history of the diseases they must treat.
The second is excellence in training during the period of specialization and thereafter. Ideally, every cardiology department that trains residents should be in charge of the ACCC unit. Training goes far beyond the number of techniques performed by a resident. Immersion and continuous contact with acutely-ill patients are essential and are achieved by devoting as many on-call duties as possible to their care, active interaction with fellow-workers during handovers, and active participation in daily decision-making concerning these patients, regardless of the area in which the resident is rotating. Thus, the SEC considers it imperative that training in this field take place in a cardiology department with an ACCC unit. The minimum duration should be 6 months when carried out in the department itself and be prolonged to 9 months when it takes place elsewhere in the hospital. During those months, cardiologists-in-training should acquire autonomy in all basic and advanced techniques, as well as in making clinical decisions concerning critically-ill cardiovascular patients.
The adequate training for supervising an ACCC unit goes far beyond that acquired during residency. It is highly specific and requires the acquisition of deeper knowledge and broader skills. Once the medical resident program has been completed, it is essential to undergo complementary training, as in other areas of cardiology such as cardiac catheterization, electrophysiology, and imaging techniques. The SEC should promote the accreditation of its professionals, with the endorsement of the European Society of Cardiology, through the Acute Cardiovascular Care Association.4 Both the SEC and the Working Group on Ischemic Heart Disease and Acute Cardiovascular Care identify completely with the mission of the Acute Cardiovascular Care Association and join forces with this body in promoting the dissemination of knowledge in the field of the critically-ill cardiovascular patient through initiatives that include the organization of masters courses, specific courses, presentations, and roundtables during the Spanish congress, etc., serving as a bridge between professionals in different specialties involved in acute cardiac care, promoting research, generating and participating in clinical practice guidelines, expert recommendations and consensus statements, extending certification in “Acute Cardiovascular Care” issued by the Acute Cardiovascular Care Association, and promoting training in this subspecialty by offering grants to young cardiologists to fund their stays in centers of excellence equipped with ACCC units.
Another question, which should be addressed specifically and is beyond the scope of this document, is the training and specialization of nursing professionals to staff the ACCC units, which is as essential as that of the physicians. The SEC will reach an agreement with the Spanish Association of Nursing in Cardiology to arrange for the accreditation of nursing personnel in ACCC units. The 2 societies will adopt a common stance, which they should convey to the health authorities, advising against allowing nurses who lack this accreditation to opt for positions in an ACCC unit. Finally, the SEC, either directly or through its regional societies, will seek an agreement with the governments of the Spanish autonomous communities so that this accreditation be taken into account in the worker selection process.
The third objective, the progressive integration of ACCC units into cardiology departments, should be understood to be a statement of intent over the mid-term that would only affect those departments with workloads that justify it. It is not feasible for all the cardiology departments to supervise an ACCC unit. Indisputably, small departments that are short on staff and on patients cannot take charge of an ACCC unit. Even so, in this scenario, every cardiologist should collaborate actively with the intensive care unit and be a key participant in making certain decisions and in complying with requests for additional studies, while acting as link to cardiology departments with ACCC units equipped with diagnostic and therapeutic tools that might be necessary for use in certain patients.
The SEC considers that the requirements demanded by the Spanish Council of Medical Specialties to grant accreditation for training medical residents in cardiology guarantee the minimum workload and staff that define those cardiology departments that should take charge of an ACCC unit, for the benefit of its patients and its residents. However, in many departments, even those with a heavy workload, this does not occur. We mentioned above that the departments with an ACCC unit show marked variability in their distribution from one Spanish autonomous community to another, but the fact that a given autonomous community has hospitals using different models suggests that this is not only a political and administrative question. Rather, it suggests that the situation is also influenced by the level of awareness among professionals and by their determination to take on this responsibility and convey it to their respective administrators. In Spain, there are several examples of cardiology departments that have incorporated an ACCC unit in recent years owing to the impetus of those responsible, who took advantage of favorable circumstances (structural changes, changes in management or in department heads, etc). The SEC considers that the creation of these new ACCC units should be a priority for those departments that train cardiology residents but still do not have such a unit. This incorporation should be progressive and take place in collaboration with intensive care units.
In the meantime, the SEC recommends taking 2 simpler measures that are easier to apply in the short-term in those departments with a sufficient workload that still do not have an ACCC unit:
- 1.
Implementing an intermediate cardiac care unit; the rational basis, infrastructure, equipment, and admission criteria for these units were defined in an article published in 2007.5 Through the Working Group on Ischemic Heart Disease and Acute Cardiovascular Care, the SEC will design a general project for setting up an intermediate cardiac care unit. This project will be made available to all the cardiology department heads who request it so that, once the situation of their departments has been evaluated, they can submit it to their hospital administrators. The SEC will name 1 or more professionals who will serve as advisors during this process, if so requested.
- 2.
To improve patient care, those responsible for cardiology departments without an ACCC unit should come to an understanding with those responsible for the departments of intensive medical care with respect to organizational models that would enable intensivists and cardiologists to share the care of patients with acute heart disease. These departments should maintain a fluid relationship with cardiology departments that have ACCC units to avoid delays in the emergency transfer of certain patients (need for a ventricular assist device, heart transplants, etc).
The healthcare of patients with acute and critical cardiovascular disease is a fundamental aspect of the development of the specialty of cardiology. Our mission as cardiologists is to assume the diagnosis and treatment of cardiac patients in all the phases of their disease. We should pursue excellence in the management of these patients in ACCC units integrated into cardiology departments and attended by adequately trained cardiologists.
In hospitals whose volume of cardiac patients is too small to justify the creation of an ACCC unit, cardiologists should not be mere performers of cardiological tests, but should actively collaborate in the evaluation and management of these patients together with general intensive care specialists.
In departments that do not have an ACCC unit but with a large enough patient volume, the priority should be to undertake their workload. In the meantime, cardiologists should become involved in the management of acutely-ill patients alongside intensivists and should contemplate the development of intermediate cardiac care units as a first step toward setting up an ACCC unit.
CONFLICTS OF INTERESTNone declared.
We thank Dr. Rosa María Lidón (president of the Working Group on Ischemic Heart Disease and Acute Cardiovascular Care) and Dr. Héctor Bueno (president of the Acute Cardiovascular Care Association) for reviewing the text and for their valuable opinions. We also wish to thank Dr. Javier Elola (Elola Consultores Madrid, Spain) for his efforts regarding the data of the RECALCAR database that we requested (financed by an unconditional grant from Laboratorios Menarini).