Keywords
Coronary spasm is a constriction of the muscular cap of the epicardial coronary arteries that causes myocardial ischemia. It is considered to be the principal mechanism of dynamic stenosis of the coronary arteries and it has been associated with effort angina, unstable angina, myocardial infarct, syncope, and sudden death.1,2
The classic method for diagnosing vasospasm is the administration of intracoronary ergonovine during diagnostic coronary angiography when the coronary arteries have been shown to be normal. For some years, stress echocardiography during the intravenous administration of ergonovine has been utilized in this context.3 Although its safety has been questioned,4 its low incidence of complications in a large group of patients has recently been demonstrated.5 To confirm this, nevertheless, we need multicenter studies with large numbers of patients, as has already been done for stress echocardiography with other drugs.6 The criteria for a positive echocardiography with ergonovine test is, as with echocardiography associated with any other type of stress, the demonstration of disturbances in contractility that did not exist on baseline examination.
On the other hand, there are some indirect signs of ischemia during stress echocardiography, such as changes in the filling flow,7 ventricular dilatation,7 or diastolic mark.8 It has also been suggested that transitory mitral insufficiency could be an indirect sign of ischemia.7
We present the case of a woman with angina and acute pulmonary edema with normal coronary arteries on angiography, in whom echocardiography with ergonovine provoked severe mitral insufficiency.
CLINICAL CASE
A 75-year-old woman with a history of arterial hypertension and dyslipemia. She was diagnosed with effort angina and had negative clinical ergometry and positive electrical tests performed later while under beta-blocker treatment. The patient went to the hospital secondary to the sudden appearance of angina and resting dyspnea. On evaluation, the patient was tachypneic and sweaty. Heart rate was 85 beats/minute and arterial pressure was 145/75 mm Hg. On cardiac auscultation, a pansystolic murmur was noted in the apex and on pulmonary auscultation crepitus was heard in the lower half of both lung fields. The ECG showed a 2 mm decline in the ST segment in I to VL and from V3 to V6. Chest x-ray revealed bilateral alveolar butterfly-wing infiltrate. After the administration of intravenous nitroglycerine and diuretics the patient improved. The baseline echocardiogram showed preserved ventricular function, no regional changes in contractility, and slight mitral insufficiency. Cardiac catheterization revealed normal coronary arteries on angiography and a normal left ventricle. A stress echocardiogram with ergonovine was performed. After the first intravenous dose (0.025 mg), the patient showed angina and dyspnea. Arterial pressure was 80/50 mm Hg. The ECG reflected changes similar to those on the admission ECG (Figure 1). Mitral insufficiency became severe (Figure 2). Although we looked carefully, no regional contractility changes were noted. After administration of intravenous nitroglycerine and fluidotherapy, the symptoms were reversed and the mitral insufficiency decrease to slight. From that time on, the patient has been asymptomatic with diltiazem treatment. Echocardiography with ergonovine performed at 3-month followup was negative. The patient did not have angina, dyspnea, ECG changes, or an increase in mitral insufficiency.
Fig. 1. The image on the left is the baseline electrocardiogram. On the right is the electrocardiogram after the administration of intravenous ergonovine, similar to the ECG on admission. A decline in the ST segment I to VL and V3 to V6.
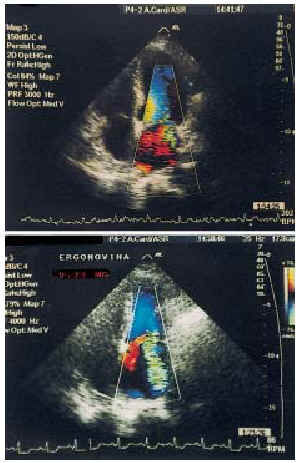
Fig. 2. Above, the echocardiography image (apical, 4-chamber) of mitral insufficiency at baseline. Below, it can be seen that the mitral insufficiency becomes severe after the administration of 0.025 mg of intravenous ergonovine.
DISCUSSION
In patients with ischemia heart disease, transitory mitral insufficiency is a sign that suggests that irrigation is being affected by a papillary muscle. When there are severe lesions, the myocardium can become hibernated and cause persistent mitral insufficiency. It has been shown, in these cases, that revascularization decreases persistent mitral insufficiency.9 Ischemic mitral insufficiency tends to be secondary to the effect of the posterior papillary muscle as it is habitually irrigated by branches of a sole principal artery, differing from the anterior artery, whose branches depend on 2 of the principal arteries. Studies of echocardiography with ergonovine have shown the precision and safety of this technique in the diagnosis of coronary spasm.5 The usefulness of the technique for guiding revascularization treatment has also been suggested in patients in whom calcium-antagonist medication is not effective.10
In the case we describe here, the association of angina with acute pulmonary edema suggests 1 of 2 possibilities: a spasm of a principal artery that provoking severe ventricular dysfunction or a spasm of a secondary branch precipitating dysfunction of a papillary muscle and severe mitral insufficiency. The absence of changes in contractility and the increase in mitral insufficiency during ergonovine administration confirm the second possibility. Acute pulmonary edema secondary to a hypertensive crisis was reasonably ruled out by arterial pressure at the time of admission. Even with elevated arterial pressure upon admission, the echocardiography results eliminated this possibility.
Although coronary spasm is generally associated with an increase in the ST segment because it causes transmural ischemia, we believe the decline in the ST segment in this case is due to theoretical transmural ischemia in a small part of the posterior region, provoking dysfunction of the posterior papillary muscle.
From a practical point of view, ergonovine echocardiography does not provide information regarding what treatment to follow. In any case, the treatment of choice is calcium antagonists. Nevertheless, echocardiography was decisive in the explanation of the mechanism by which the acute pulmonary edema was produced. This case illustrates the possibility that stress echocardiography with ergonovine may be helpful in identifying the clinical mechanism in a patient with normal arteries.
Correspondence: Dr. J.A. San Román.
Instituto de Ciencias del Corazón (ICICOR).
Hospital Universitario.
Ramón y Cajal, 3. 47011 Valladolid. España.
E-mail: jsancal@nexo.es