To the Editor,
A 65-year-old woman visited our clinic with a complaint of lower limb edema. A chest X-ray revealed pleural effusion, and echocardiography showed normal left ventricular function, but right heart enlargement and pulmonary hypertension were present, and estimated pulmonary artery pressure was 70 mmHg. Investigation of the cause of the pulmonary hypertension and heart failure revealed left lower leg pigmentation and swelling. Gated time-of-flight angiography was performed because of auscultation of a vascular bruit, and the results showed marked dilatation down to the popliteal artery, with left lower limb arteries maintained at the same diameter as the abdominal aorta (Figure 1A). Contrast-enhanced computed tomography showed prominent arteriovenous dilatation and a complex arteriovenous fistula and mass formation below the knee (Figure 1B and 1C). The patient had a history of surgery for osteomyelitis of the left lower leg 50 years previously. The possible presence of an iatrogenic arteriovenous fistula was considered the probable cause of both the marked dilatation of the arteries and veins, and of the mass formation. Right cardiac catheterization revealed a cardiac output of 7 L/min. With the application of a left thigh tourniquet the cardiac output decreased to 4 L/min. Coil embolization was considered impossible because selective arteriography showed a large and complex arteriovenous fistula.1,2 Since the patient refused amputation,3,4 we selected drug therapy and monitored the course. Cases of long-term neglect of an acquired arteriovenous fistula resulting in prominent arteriovenous dilatation and mass formation are very rare.
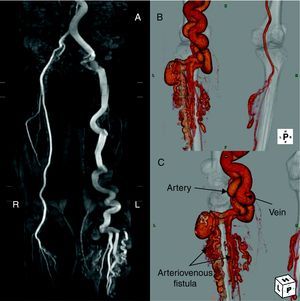
Figure 1. A: Marked dilatation of the left lower limb arteries maintained at the same diameter as the abdominal aorta. B and C: Prominent arteriovenous dilatation and a complex arteriovenous fistula and mass formation below the knee.
Corresponding author: so_ichi75@yahoo.co.jp