Keywords
INTRODUCTION
Patent ductus arteriosus is a common condition in pediatric cardiology, accounting for around 7% of all congenital heart diseases in this population. The defect generally occurs on the left side, even when the aortic arch is right-sided.1 Other anomalies are often found in this condition, such as atrial septal defect, ventricular septal defect, and absent or hypoplastic pulmonary arteries. The association of a right-sided aortic arch with an ipsilateral patent ductus arteriosus (PDA) as an isolated lesion is rare. In this article we describe three such cases, in which percutaneous closure of the defect was achieved with Amplatzer devices.
CLINICAL CASE REPORTS
Our series is comprised of three female patients (Table) with no symptoms of dysphagia or stridor. The 2 adult patients presented fatigue on moderate exertion and had undergone unsuccessful attempts at surgical closure of the ductus arteriosus at other institutions on two occasions each. The diagnosis of right-sided aortic arch and ipsilateral PDA had not been defined by echocardiography before the first unsuccessful attempt at surgical closure using a left lateral thorocotomy. Following this attempt, angiography was performed in both patients and the diagnosis was defined. Nevertheless, in the second surgical procedure using a median sternotomy, the right-sided ductus arteriosus remained unidentified. The third patient, who was 9 years old, was asymptomatic. On physical examination, all patients presented continuous murmur in the right second intercostal space and a wide pulse pressure. At our centers, color Doppler echocardiography showed a right-sided aortic arch and ipsilateral ductus arteriosus with a continuous left-to-right shunt and considerable aortopulmonary gradients (50-70 mm Hg), with left ventricular dilation.
Cardiac catheterization to close the defect by percutaneous techniques was performed in all cases. The procedures were carried out under conscious sedation in the adults and general anesthesia in the girl. Aortography in left lateral, and right and left anterior oblique views confirmed the presence of a right-sided aortic arch with mirror-image supraaortic vessels and a Krichenko type A3 ductus emerging from the distal, ventral portion of the arch, with filling of the right pulmonary artery. In the 9-year-old girl, the entire course of the ductus was visualized, allowing adequate determination of the minimum diameter of the defect on the pulmonary side (Figure 1). In contrast, angiography in several views could not adequately define the minimum diameter in the 2 adults, due to the orientation of the ductus and, probably, to the patients' size. Therefore, to determine this parameter with precision, measurement with a sizing balloon (AGA Medical Corporation, MN, USA) following previously described techniques4 was decided (Figure 2). Additionally, due to the difficulty of anterograde catheterization of the ductus, retrograde crossing of the ductus was performed in all cases and the guidewire was snared in the pulmonary artery to establish a femoral arteriovenous loop. Thus, in the 2 adults, a sizing balloon was advanced through an anterograde route to the descending aorta, where it was slightly inflated with equal amounts of contrast medium and saline solution (Figure 2C). Under digital recording, the sizing balloon was advanced over the guidewire through the defect toward the pulmonary artery. Following measurement of the minimum diameter of the pulmonary PDA, the defect was closed using the classic anterograde technique.5 An Amplatzer duct occluder was implanted in the first 2 patients. In the third case, even though the ductus was type A, a muscular ventricular septal defect occluder was chosen because the patient had a shallow aortic ampulla and a short course. The follow-up aortic and pulmonary angiographies showed that the devices were satisfactorily positioned, without protruding into the pulmonary artery, and there was no residual shunting (Figures 1B and 3). No pressure gradients were recorded in the aorta or the pulmonary branches following implantation.
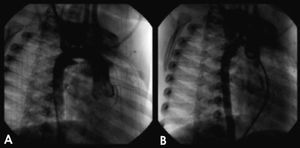
Figure 1. Case 1. Angiographic images in a right anterior oblique view before and after implant placement. A: the right-sided aortic arch is seen and an ipsilateral Krichenko type A ductus arteriosus, with a minimum diameter of 2 mm. B: complete closure of the defect following deployment of a 6-4 Amplatzer duct occluder.
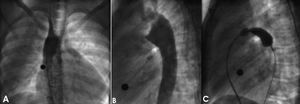
Figure 2. Case 2. Aortography before implantation and measurement of the stretched diameter of the defect. A: in the right anterior oblique view, a mirror image of the aortic arch is evident. B: the left lateral view shows the anatomy of the defect. Although the ductus was a Krichenko type A, it was not possible to precisely determine the minimum diameter of theside pulmonary side. C: determination of the minimum diameter with a sizing balloon.
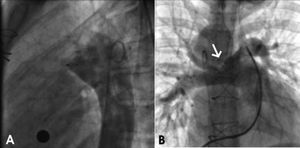
Figure 3. Case 2. Angiography following implantation. A: aortography in a left lateral view. The Amplatzer duct occluder 8-6 is well positioned, with no residual shunting. B: pulmonary angiography in a right oblique view shows the final position of the device within the ductus, which inserts in the right branch (arrow). The device does not protrude into the vessel
All 3 patients were discharged within the first 24 hours following the procedure without complications. The echocardiography examinations at hospital discharge and at 3 months showed complete occlusion of the defect and absence of aortic and pulmonary artery gradients.
DISCUSSION
The reported incidence of right-sided aortic arch ranges from 0.04% to 0.14%.1,2 This anomaly is determined by persistence of the right dorsal aorta with regression of the left dorsal aorta, and can present in association with patent ductus arteriosus in several variants, some of which can produce vascular rings with esophageal or tracheal compression.6 Even though the aortic arch is located at the right, the most frequent position of the ductus is at the left, arising from the left subclavian artery and connecting with the pulmonary artery on the same side.1 This modality is generally associated with congenital cyanotic cardiac disease, in which ductus patency is favorable for the patient's survival. Similarly, the majority of cases (98%) of right-sided aortic arch and ductus arteriosus are associated with intracardiac anomalies, such as atrial septal defect and absence or hypoplasia of the pulmonary artery.7-9 It is very unusual to find this association in the absence of heart disease, such as the cases described in this report.
Until the development of percutaneous therapy for the ductus arteriosus, the classic treatment has been surgery; right posterolateral thoracotomy is recommended to better visualize the ductus and adjacent structures, such as the right main bronchus.7 Use of a left thoracotomy or sternotomy limits the possibility of achieving surgical closure, as was illustrated by the 2 cases in our series in which surgical treatment was attempted without success.
The clinical experience with percutaneous closure of the ductus arteriosus has been extensively described over the last years and, in keeping with the size of the ductus, various devices have been used, such as Gianturco coils, controlled-release coils, Grifka occlusion devices, Nit-Occlud coils and Amplatzer devices.10-12 In the rare association reported in this review, only 2 similar cases with percutaneous closure have been described. The first was reported by Bermúdez-Cañete et al within a series of 26 cases of percutaneous PDA closure using the Rashkind PDA Occluder.13 Among the patients included in that study, the authors mention one with a right-sided aortic arch and a residual ipsilateral ductus following surgical ligature, in which retrograde catheterization of the ductus with posterior application of the arteriovenous loop technique was also used for anterograde implantation of the device. This technique has been used in cases in which the ductus is in an unusual position and orientation, and in those with a tortuous course, leading to difficulties for anterograde catheterization, as occurred in our small series. The other case in the literature was described by Rao et al, who reported 2 cases of right-sided aortic arch and ductus arteriosus,14 one of which corresponded to the same type as our series, and was successfully occluded with implantation of a 38-5-5 Gianturco coil. The other case mentioned in Rao's article corresponded to a different type, in which the ductus originated in an aberrant left subclavian artery from the descending aorta.
Because of the orientation and position of the ducti, together with the size of two of our patients, it was difficult to precisely assess the minimum diameter of the defects by angiography in standard views. This made it impossible to select the most suitable device to use. Therefore, based on previous experience,4 we decided to use the stretched diameter of the defect, in order to minimize the possibilities of a poor choice, residual shunts or embolization.
Among the devices used for percutaneous closure of the ductus arteriosus, the Amplatzer PDA has proven to be very safe and effective, with occlusion rates of 99.7%.12 Moreover, the fact that the device can be recovered and repositioned makes it particularly useful in unusual anomalies, such as those presented. However, in the literature, no cases have been described in which this device is used for percutaneous closure of a right-sided ductus arteriosus associated with an ipsilateral aortic arch. The use of a device designed for interventricular defects in one of our patients was based on caution, since we judged that the ductus had a shallow aortic ampulla and a short course in several angiographs, in which the exact anatomy of the defect remained inconclusive. These double-disk Amplatzer devices are recommended for large ducti associated with pulmonary hypertension and with this type of anatomy.3 In the other 2 patients, who had a well-defined, wide aortic ampulla, the Amplatzer Duct Occluder was easily implanted, properly positioned, and achieved complete occlusion of the defect. In conclusion, percutaneous closure of a right-sided ductus in the presence of an ipsilateral aortic arch with Amplatzer devices is feasible, safe, and effective. This technique is preferable to surgical closure. Nevertheless angiographic visualization of the entire course of the ductus can be difficult, particularly in adults. Hence, for proper selection of the device to use, we recommend determination of the stretched diameter of the ductus with a sizing balloon.
Correspondence: Dr. C. AC. Pedra.
Sección Médica de Intervenciones en Cardiopatías Congénitas.
Instituto Dante Pazzanese de Cardiología.
Avda. Dr. Dante Pazzanese, 500. 04012-180 São Paulo. SP. Brasil.
E-mail: cacpedra@uol.com.br
Received August 28, 2006.
Accepted for publication October 10, 2006.