Congenital heart diseases (CHDs) are a complex spectrum of malformations that are difficult to detect and interpret during prenatal life due to the wide variability in their possible presentation among patients.1 Their complexity and heterogeneity are also a significant challenge during prenatal parental counselling due to the difficulty of explaining the child's condition to the family in a simple but comprehensive way. The various imaging techniques currently used for the fetal diagnosis and assessment of CHDs are computed tomography (CT), magnetic resonance imaging (MRI), and ultrasound.2
All of the above-mentioned techniques can also be used to obtain a 3-dimensional (3D) model of fetal hearts based on the true anatomy of the patient, which could perhaps be more effective in explaining the fetal malformation to parents during prenatal counselling. The application of CT scans is strongly limited by the exposure of the mother and fetus to X-rays, which makes this technique not routinely suitable in the prenatal setting. Regarding MRI, its long acquisition times significantly affect the quality of the images obtained because the operator cannot easily limit fetal movements (obtainable only by sedation of both the mother and the fetus).3
In our maternal-fetal medicine unit, we started applying a 3D printing protocol to echo images acquired with a Voluson E8/E10 machine (GE Healthcare, Chicago, IL, USA) using cardiac spatio-temporal image correlation (STIC)4 at the time of diagnosis of complex fetal CHDs. All the volumes are subsequently exported as a DICOM file and a virtual 3D object (as a stereo lithography file) is created using Mimics InPrint software (Materialise, Leuven, Belgium). Finally, the virtual model is transferred to a 3D printer and transparent resin is regularly used to print the hearts, both in real size and enlarged 5 times. The printing phase requires about 9hours, with a total time to complete the whole process of approximately 12hours.5
During the initial phase of our project, we were able to create 5 different virtual and printed models of fetal hearts with complex CHD (figure 1 and figure 2). All of these models were used during prenatal counselling to offer parents the possibility to hold their child's heart in their hand (real dimension printed heart) and to better comprehend the features of the CHD by showing a model magnified 5 times.
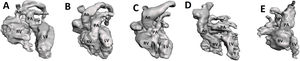
Stereo lithography reconstruction of fetal hearts obtained using spatio-temporal image correlation. A: D-transposition of the great arteries (D-TGA). B: complete atrioventricular septal defect. C: tetralogy of Fallot. D: D-TGA, ventricular septal defect and pulmonary stenosis. E: interrupted aortic arch (type B). Ao, aorta; LV, left ventricle; PA, pulmonary artery; RV, right ventricle, asterisk indicating the ventricular septal defect.
3D printed real dimensions models of fetal hearts with clear resin (front line) and matched 3D printed version of the same hearts magnified 5 times (back line). A: D-transposition of the great arteries (D-TGA) diagnosed at 30 weeks of gestation (WG). B: complete atrioventricular septal defect diagnosed at 27 WG. C: tetralogy of Fallot diagnosed at 25 WG. D: D-TGA, ventricular septal defect and pulmonary stenosis diagnosed at 22 WG. E: interrupted aortic arch (type B) diagnosed at 22 WG.
In vivo evaluation of all the fetal hearts (except that with D-transposition of the great arteries with associated ventricular septal defect and pulmonary stenosis, which has not yet undergone surgery) during the surgical intervention confirmed the accuracy of the images obtained during the prenatal period.
The use of ultrasound with the STIC technique allows images to be obtained even in a very early fetal stage and before the usual term imposed for pregnancy termination, which is around 23 weeks of gestation. This can be highly important in particularly complex CHDs where fetal abnormalities have serious implications for the child's life and the family's expectations. In these particular cases, the timing of prenatal counselling can be crucial and fetal 3D heart models can help to improve parents’ awareness of their child's disease and its severity, allowing them to take a more informed decision about the pregnancy course.
Based on these initial results, we believe that the use of 3D virtual and printed models obtained with ultrasound and STIC techniques during prenatal counselling can increase the quality of our clinical practice and help strengthen the relationship between physicians and families. 3D-based prenatal counselling has now been adopted as a routine practice in our Institution in selected cases but can be further extended to less complex CHDs in order to facilitate parents’ understanding of their child's condition, especially in patients who might require invasive procedures after birth. Hopefully, we will soon be able to create a comprehensive series of specimens that can be used as a retrospective library of similarly malformed hearts for parental counselling.
Further validation of these preliminary results with a larger number of cases is needed to evaluate the real benefits of this methodology. However, we believe that our study has 2 main messages: the first concerns the need for innovation in the use of ultrasound images suitable for 3D printing, and the second is related to the need for excellent collaboration with the Heart Team in providing parental counselling for CHD. The use of 3D printed hearts has proven to greatly improve this second aspect in our institution.