The Cambridge Pulmonary Hypertension Outcome Review (CAMPHOR) is a patient-reported outcome measure of health-related quality of life and quality of life specific to individuals with pulmonary hypertension (PH). This questionnaire has demonstrated superiority over other instruments assessing similar domains. The objective of the present study was to adapt and validate the Spanish version of the questionnaire.
MethodsThe adaptation consisted of 3 stages: translation from English to Spanish using bilingual and lay panels, cognitive debriefing interviews with patients, and assessment of psychometric properties by means of a postal validation survey.
ResultsThe translation panels produced a version of the CAMPHOR that was considered suitable for use by Spanish PH patients. The relevance, comprehensiveness, and acceptability of this version were confirmed in interviews with PH patients. Finally, the validation survey (n = 70) revealed that the 3 CAMPHOR scales (Symptoms, Activities, and Quality of life) showed strong psychometric properties. The internal consistency (Cronbach α) coefficients of the scales were above 0.89, and the test-retest reliability was above 0.87. The convergent and known group validity of the CAMPHOR scales was also demonstrated.
ConclusionsThe Spanish version of the CAMPHOR is a valid and reliable instrument for the assessment of health-related quality of life and quality of life in Spanish PH patients. Therefore, it is recommended for use in future research and clinical practice in the Spanish population of PH patients.
Keywords
Pulmonary hypertension (PH) is a disorder of the pulmonary vasculature characterized by increased pulmonary vascular resistance. Commonly reported symptoms include shortness of breath, reduced exercise capacity, chest pain, edema, and syncope.1 The current clinical classification of PH consists of 5 groups characterized by different pathological features:2
- 1.
Pulmonary arterial hypertension.
- 2.
PH due to left heart disease.
- 3.
PH due to lung diseases and/or hypoxia.
- 4.
Chronic thromboembolic PH.
- 5.
PH with unclear multifactorial mechanisms.
Pulmonary hypertension is an incurable disorder; only eligible patients with chronic thromboembolic PH can be offered a cure by means of pulmonary thromboendarterectomy.3 Pulmonary hypertension leads to right ventricular failure and may cause premature death if untreated.4
The clinical presentation of PH has changed dramatically since disease-specific medications were introduced 2 decades ago. Before then, the median life expectancy after diagnosis was only 2.8 years and treatment was mostly directed at palliating symptoms.5 Subsequent pharmacological advances have continued to expand the arsenal of drugs designed specifically to treat PH and have made it possible to target multiple pathophysiological mechanisms implicated in the progression of the disease. Current treatment approaches have shown success in improving hemodynamic measures, exercise capacity, and survival times.6
Despite improvements in treatment and clinical management,1 the potential impact of PH on a person's life continues to be substantial. In addition to the physical and functional impact produced by the disease, the burden of treatment can also be considerable. Some of these treatments involve complex methods of administration and can sometimes result in complications and adverse effects. These include catheter infections resulting from intravenous administration,7 together with skin rashes and site pain resulting from subcutaneous infusion.8 Altogether, these aspects may further impact individuals’ emotional wellbeing and impose constraints on their social and family life. Several endpoints have been traditionally used in the assessment of clinical status in PH, including hemodynamic parameters, exercise capacity, and biological markers. However, such endpoints provide limited information on how patients actually feel.9 Patient-reported outcome measures, when carefully designed, can assess both the impact of the disease and the effectiveness of its treatment as perceived by patients. Further, patient-reported outcome measures may provide relevant information about health status that may be unnoticed by clinicians.10
The Cambridge Pulmonary Hypertension Outcome Review (CAMPHOR) was the first patient-reported outcome measure specifically designed to evaluate health-related quality of life (HRQoL) and quality of life (QoL) in individuals with PH.11 Although related, these 2 constructs are based on 2 different theoretical models as approached by the CAMPHOR. That is, HRQoL taps into the presence of symptoms (physical and psychological) and functional limitations, and therefore constitutes a direct reflection of health status. Alternatively, the operationalization of QoL is based on the needs-based model, which proposes that life gains quality when a person is able to satisfy his/her needs. According to the needs-based model, symptoms and functional disability are not direct indicators of QoL, but are rather 2 factors that may influence QoL to the extent that they may interfere with need-fulfilment. Similarly, many other nonhealth factors (eg, finances, employment, social support) may also interfere with or promote need-fulfilment and influence QoL.12,13
The development of the CAMPHOR constituted an important advance in QoL research in PH. Previously, outcomes for patients with PH had relied on generic instruments (eg, the Short-Form 36 [SF-36], the Nottingham Health Profile [NHP]) and other instruments designed for related conditions (eg, the Minnesota Living with Heart Failure Questionnaire [MLHFQ], the Chronic Heart Failure Questionnaire [CHQ]).10 However, these instruments have shown poor responsiveness to change when used with PH patients, as they do not inquire about many aspects important to PH patients.10 In contrast, the CAMPHOR was created from in-depth interviews with PH patients to ensure that its content covered the full scope of the impact of the disease and was thus relevant to patients’ real experience. Moreover, the CAMPHOR scales were developed using Rasch analysis, an approach that has largely replaced the use of classic test theory in instrument development.11 The use of Rasch analysis ensures that the resulting scales are unidimensional and measure at the interval- rather than the ordinal-level. This attribute is particularly relevant to clinical trials, as it increases responsiveness and reduces the sample sizes required.14 Even though more comparative studies would be beneficial, the CAMPHOR has demonstrated superior psychometric properties to those of other instruments that have been used to assess outcome in PH, such as the SF-3615,16 and the NHP.11 The CAMPHOR was developed in the United Kingdom and has been adapted and validated for use in Canada (both in French and English),17 the United States,16 Australia/New Zealand,18 Germany/Switzerland/Austria,19 Sweden,20 the Netherlands,21 and Portugal.22
The present study describes the process of adaptation of the CAMPHOR for use in Spain. According to data from the Spanish Registry of Pulmonary Arterial Hypertension, the estimated prevalence of this disease in Spain is 16 cases per million adult inhabitants, while that of chronic thromboembolic PH is 3.2 cases. The data also show that patients are being identified at an earlier disease stage, which, along with improved PH therapy, has been associated with increased survival.23 These positive trends have allowed the expansion of therapeutic goals, and issues pertaining to the QoL of patients have become increasingly significant. However, assessment of the QoL of Spanish PH patients has been limited by the use of PH–non-specific QoL instruments.
MethodsProcedureThis study was part of 2 independent research projects approved by the Ethics Committees of the Autonomous University of Madrid and the Hospital 12 de Octubre, both in Madrid, Spain. The process of adaptation of the Spanish version of the CAMPHOR involved 3 stages: translation from English to Spanish, cognitive debriefing interviews with Spanish-speaking PH patients, and a postal validation survey.
Translation From English to SpanishThe dual panel methodology24 was employed for the translation stage. A bilingual panel of native Spanish speakers fluent in English without experience of PH was conducted to provide the initial translation. The translation was then refined by a lay panel of monolingual Spanish individuals of average to below-average educational achievement, who were representative of the target population. The purpose of the lay panel was to ensure that common everyday language and idioms were included in the translated measure.
Cognitive Debriefing InterviewsTwenty-three patients with PH (male, 39%; mean age, 52.3 ± 14.7 years) were recruited to take part in 1-to-1 cognitive debriefing interviews. The objective of these interviews was to test whether the Spanish version produced by the translation panels was comprehensive and easy to understand, and to identify any problems experienced by respondents. Interviewees were first asked to complete the CAMPHOR in the presence of an investigator who took note of any hesitation or difficulty. Next, respondents were asked about the comprehensibility of the items, whether the wording sounded natural in Spanish, and whether they thought there were any relevant aspects of living with PH that had not been included in the questionnaire.
Postal Validation SurveyA postal survey was conducted to test the psychometric properties of the Spanish CAMPHOR. Data were collected from a sample of 70 patients (male, 20%; mean age, 49.2 ± 13.30 years), which included 8 of the 23 patients who took part in the cognitive debriefing interviews. Participants completed a questionnaire package on 2 occasions, approximately 2 weeks apart. A 2-week interval was selected because disease status is unlikely to change during this time and the participants’ responses are unlikely to be influenced by recall bias. In addition to the Spanish version of the CAMPHOR, the package included a demographic questionnaire and the Spanish version of the NHP,25 which was used as a comparator scale.
Most participants taking part in the postal validation survey were recruited from the National Association of Pulmonary Hypertension; a smaller subsample was also recruited from the Hospital 12 de Octubre, in Madrid. Altogether, the sample represented most regions of Spain. Patients were eligible to participate if they were 18 years old or older, were native Spanish speakers, and had a confirmed diagnosis of PH according to the World Health Organization Diagnostic Classification. Several exclusion criteria were also set: having undergone pulmonary thromboendarterectomy and an inability to understand what was required from participation or give informed consent.
Statistical AnalysesDescriptive StatisticsThe distributional properties of scores on the measures were explored by calculating medians, interquartile ranges, means ± standard deviations, and floor/ceiling effects (ie, the percentage of patients scoring the minimum and maximum possible scores, respectively).
Internal ConsistencyThe Cronbach α coefficient was used to assess the internal consistency of the CAMPHOR scales. This measures the extent to which the items of a scale are interrelated. Alpha values above 0.70 indicate that the items work together to form a scale.26
Test-retest ReliabilityThe Spearman rank correlation coefficient was used to assess the test-retest reliability of the CAMPHOR scales. The test-retest reliability of a measure is an estimate of the consistency of scores over time, assuming no change in condition has taken place. A correlation above 0.85 indicates that the instrument produces low random measurement error.27
Convergent ValidityConvergent validity can be determined by examining the level of association between scores on the scale of interest and those from a measure that assesses the same or related constructs. For the present investigation, CAMPHOR scores were correlated with NHP section scores using Spearman rank correlation coefficients.
Known Group ValidityKnown group validity assesses whether a measure is able to distinguish between groups of respondents that differ according to some known factor thought to influence their scores on the measure. The factors used for the present investigation were perceived general health (categorized as either “very good”/“good” or “fair”/“poor”), perceived disease severity (categorized as either “mild”/“moderate” or “severe”/“very severe”), and World Health Organization classification (functional classes I to IV). Due to the relatively small sample sizes, participants in functional classes III and IV were grouped together. Nonparametric tests for independent samples (ie, the Mann-Whitney U test for 2 groups or Kruskal-Wallis one-way analysis of variance for 3 or more groups) were used for these analyses.
MeasuresCambridge Pulmonary Hypertension Outcome ReviewThe CAMPHOR11 consists of 3 scales: Symptoms, Activities and QoL. The Symptoms scale assesses the presence of symptoms characteristic of PH. It contains 25 items with a dichotomous response format (“yes”/“no”), allowing scores to range from 0 to 25. The activities scale contains 15 items and evaluates whether participants can perform a series of activities of daily life. Each item has 3 response options: “Able to do on own without difficulty”, “Able to do on own with difficulty”, and “Unable to do on own”. Scores on this scale can range from 0 to 30. These 2 scales, Symptoms and Activities, assess HRQoL. The QoL scale has 25 items (answered “true” or “not true”) with scores ranging from 0 to 25, and assesses whether individuals are able to fulfill needs that may be affected by PH. Higher scores on the Symptoms, Activities, and QoL scales are indicative of increased symptoms, poorer physical functioning, and lack of ability to satisfy needs, respectively. Therefore, higher scores on the 3 CAMPHOR scales correspond to lower levels of HRQoL and QoL.
Nottingham Health ProfileThe NHP28 is a generic self-report measure of perceived health status. It contains 38 items assessing health problems across 6 different sections: energy level, pain, emotional reactions, sleep quality, social isolation, and physical mobility. A dichotomous response format (“yes”/“no”) is used, and responses are converted to a percentage to allow section scores to range from 0 to 100, with higher scores indicating worse health status. In addition, embedded within the NHP is the index of Distress, a measure of illness-related distress. The NHP index of Distress has 24 items and produces scores ranging from 0 to 24.
ResultsTranslation From English to SpanishThe bilingual panel consisted of 3 women and 2 men, aged between 27 and 39 years. Even though they were able to provide translations for the instructions and items in the measure, several options for some items were forwarded to the lay panel for them to make a choice. Some changes were made by the bilingual panel to make the measure more appropriate for the Spanish population, such as instructing the patient to “cross” instead of “tick” the answer box. Colloquial English phrases were translated in a way that ensured conceptual equivalence in Spanish. Further, the panel opted for masculine forms in relevant words instead of dual sex forms, as this is the correct grammatical usage in Spanish.
The lay panel included 2 women and 4 men, aged between 19 and 59 years. Members of the panel were able to select the most appropriate options out of those proposed by the bilingual panel. The panel agreed with the bilingual panel members on the use of masculine forms throughout the measure. Minor changes were made to ensure that the translations were clear and comprehensible to the Spanish population. For the QoL scale, the lay panel decided to change the response options proposed by the bilingual panel (from “cierto”/“no cierto” to “verdadero”/“falso” – both meaning “true”/“false”) as it was thought that the latter was more commonly used in Spain.
Cognitive Debriefing InterviewsOverall, the PH patients interviewed considered the Spanish version of the CAMPHOR to be relevant, comprehensive, and easy to understand. Most of the translation sounded natural in Spanish. As a result of the interviews, 2 items were changed. For item 21 on the Symptoms scale, the word “raramente” was changed to “muy pocas veces” – both mean “rarely” but the latter is more commonly used. Similarly, for item 15 on the QoL scale, “largas distancias” (large distances) was changed to “lejos de mi casa” (away from my house), as the interviewees felt that the latter was easier to understand. This updated questionnaire was used in the postal survey. A sample of items from the Spanish and United Kingdom versions of the CAMPHOR can be found in Table 1.
Sample of Items From the Spanish and United Kingdom Versions of the Cambridge Pulmonary Hypertension Outcome Review
| Escala de síntomas (25 ítems) | Symptoms scale (25 items) |
| Tengo poca energía | My stamina levels are low |
| Me canso con rapidez | I get tired very quickly |
| Me siento muy débil | I feel very weak |
| Cuando camino me quedo sin aliento | When I walk I get out of breath |
| Me quedo sin aliento al subir un escalón | I get breathless going up one step |
| Incluso sin hacer nada me quedo sin aliento | I get breathless without doing anything |
| Me siento muy decaído | I get very down |
| He olvidado lo que significa disfrutar | I’ve forgotten what it's like to enjoy myself |
| A menudo me siento angustiado | I often feel anxious |
| Escala de actividades (15 ítems) | Activities scale (15 items) |
| Vestirme | Get dressed |
| Caminar distancias cortas en terreno llano | Walk short distances on level ground |
| Estar de pie durante un corto periodo de tiempo | Stand for a short time |
| Levantar objetos pesados | Lift heavy items |
| Escala de calidad de vida (25 ítems) | Quality of life scale (25 items) |
| Mi enfermedad condiciona mis relaciones personales | My condition puts a strain on my close relationships |
| No puedo hacer cosas de manera improvisada | I can’t do things on the spur of the moment |
| Siento que mi cuerpo no me responde | It feels like my body has let me down |
| Me siento como una carga para los demás | I feel as if I am a burden to people |
| No soy capaz de participar en actividades con la familia y los amigos | I’m unable to join in activities with my family and friends |
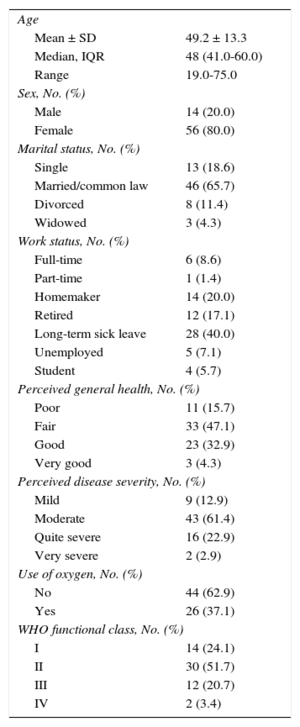
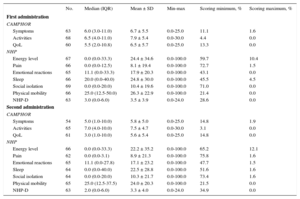
Detailed demographic and clinical information about the participants is shown in Table 2. High floor effects (participants scoring the minimum) were observed in the NHP section scores, suggesting that generic measures are not suitable for assessing HRQoL and QoL in individuals with PH. Further information regarding the descriptive statistics of the questionnaire scores is shown in Table 3.
Demographic and Clinical Characteristics of the Postal Survey Participants (n = 70)
| Age | |
| Mean ± SD | 49.2 ± 13.3 |
| Median, IQR | 48 (41.0-60.0) |
| Range | 19.0-75.0 |
| Sex, No. (%) | |
| Male | 14 (20.0) |
| Female | 56 (80.0) |
| Marital status, No. (%) | |
| Single | 13 (18.6) |
| Married/common law | 46 (65.7) |
| Divorced | 8 (11.4) |
| Widowed | 3 (4.3) |
| Work status, No. (%) | |
| Full-time | 6 (8.6) |
| Part-time | 1 (1.4) |
| Homemaker | 14 (20.0) |
| Retired | 12 (17.1) |
| Long-term sick leave | 28 (40.0) |
| Unemployed | 5 (7.1) |
| Student | 4 (5.7) |
| Perceived general health, No. (%) | |
| Poor | 11 (15.7) |
| Fair | 33 (47.1) |
| Good | 23 (32.9) |
| Very good | 3 (4.3) |
| Perceived disease severity, No. (%) | |
| Mild | 9 (12.9) |
| Moderate | 43 (61.4) |
| Quite severe | 16 (22.9) |
| Very severe | 2 (2.9) |
| Use of oxygen, No. (%) | |
| No | 44 (62.9) |
| Yes | 26 (37.1) |
| WHO functional class, No. (%) | |
| I | 14 (24.1) |
| II | 30 (51.7) |
| III | 12 (20.7) |
| IV | 2 (3.4) |
IQR, interquartile range; SD, standard deviation; WHO, World Health Organization.
Descriptive Statistics of Cambridge Pulmonary Hypertension Outcome Review Scores
| No. | Median (IQR) | Mean ± SD | Min-max | Scoring minimum, % | Scoring maximum, % | |
|---|---|---|---|---|---|---|
| First administration | ||||||
| CAMPHOR | ||||||
| Symptoms | 63 | 6.0 (3.0-11.0) | 6.7 ± 5.5 | 0.0-25.0 | 11.1 | 1.6 |
| Activities | 68 | 6.5 (4.0-11.0) | 7.9 ± 5.4 | 0.0-30.0 | 4.4 | 0.0 |
| QoL | 60 | 5.5 (2.0-10.8) | 6.5 ± 5.7 | 0.0-25.0 | 13.3 | 0.0 |
| NHP | ||||||
| Energy level | 67 | 0.0 (0.0-33.3) | 24.4 ± 34.6 | 0.0-100.0 | 59.7 | 10.4 |
| Pain | 66 | 0.0 (0.0-12.5) | 8.1 ± 19.4 | 0.0-100.0 | 72.7 | 1.5 |
| Emotional reactions | 65 | 11.1 (0.0-33.3) | 17.9 ± 20.3 | 0.0-100.0 | 43.1 | 0.0 |
| Sleep | 66 | 20.0 (0.0-40.0) | 24.8 ± 30.0 | 0.0-100.0 | 45.5 | 4.5 |
| Social isolation | 69 | 0.0 (0.0-20.0) | 10.4 ± 19.6 | 0.0-100.0 | 71.0 | 0.0 |
| Physical mobility | 66 | 25.0 (12.5-50.0) | 26.3 ± 22.9 | 0.0-100.0 | 21.4 | 0.0 |
| NHP-D | 63 | 3.0 (0.0-6.0) | 3.5 ± 3.9 | 0.0-24.0 | 28.6 | 0.0 |
| Second administration | ||||||
| CAMPHOR | ||||||
| Symptoms | 54 | 5.0 (1.0-10.0) | 5.8 ± 5.0 | 0.0-25.0 | 14.8 | 1.9 |
| Activities | 65 | 7.0 (4.0-10.0) | 7.5 ± 4.7 | 0.0-30.0 | 3.1 | 0.0 |
| QoL | 61 | 3.0 (1.0-10.0) | 5.6 ± 5.4 | 0.0-25.0 | 14.8 | 0.0 |
| NHP | ||||||
| Energy level | 66 | 0.0 (0.0-33.3) | 22.2 ± 35.2 | 0.0-100.0 | 65.2 | 12.1 |
| Pain | 62 | 0.0 (0.0-3.1) | 8.9 ± 21.3 | 0.0-100.0 | 75.8 | 1.6 |
| Emotional reactions | 65 | 11.1 (0.0-27.8) | 17.1 ± 23.2 | 0.0-100.0 | 47.7 | 1.5 |
| Sleep | 64 | 0.0 (0.0-40.0) | 22.5 ± 28.8 | 0.0-100.0 | 51.6 | 1.6 |
| Social isolation | 64 | 0.0 (0.0-20.0) | 10.3 ± 21.7 | 0.0-100.0 | 73.4 | 1.6 |
| Physical mobility | 65 | 25.0 (12.5-37.5) | 24.0 ± 20.3 | 0.0-100.0 | 21.5 | 0.0 |
| NHP-D | 63 | 2.0 (0.0-6.0) | 3.3 ± 4.0 | 0.0-24.0 | 34.9 | 0.0 |
CAMPHOR, Cambridge Pulmonary Hypertension Outcome Review; IQR, interquartile range; NHP, Nottingham Health Profile; NHP-D, Nottingham Health Profile index of Distress; QoL, Quality of Life; SD, standard deviation.
Cronbach α coefficients were above 0.80 for the 3 CAMPHOR scales, indicating high levels of internal consistency. The 3 CAMPHOR scales showed excellent test-retest reliability (above 0.85), demonstrating low levels of random measurement error (Table 4).
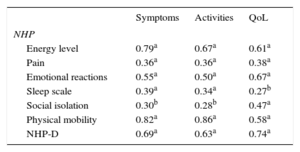
Convergent ValidityTable 5 shows the correlations between the CAMPHOR scores and those on the NHP sections at Time 1. The CAMPHOR Symptoms scale correlated strongly with the energy level and physical mobility sections of the NHP, showing the importance of these symptoms in influencing the QoL of individuals with PH. As expected, the CAMPHOR Activities scale correlated most strongly with the NHP physical mobility section. It is noteworthy that QoL scores were associated with both the physical and psychological aspects of PH.
Correlation Coefficients Between Cambridge Pulmonary Hypertension Outcome Review and Nottingham Health Profile Scores at Time 1
| Symptoms | Activities | QoL | |
|---|---|---|---|
| NHP | |||
| Energy level | 0.79a | 0.67a | 0.61a |
| Pain | 0.36a | 0.36a | 0.38a |
| Emotional reactions | 0.55a | 0.50a | 0.67a |
| Sleep scale | 0.39a | 0.34a | 0.27b |
| Social isolation | 0.30b | 0.28b | 0.47a |
| Physical mobility | 0.82a | 0.86a | 0.58a |
| NHP-D | 0.69a | 0.63a | 0.74a |
NHP, Nottingham Health Profile; NHP-D, Nottingham Health Profile index of Distress; QoL, quality of life.
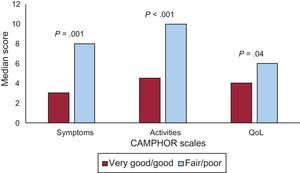
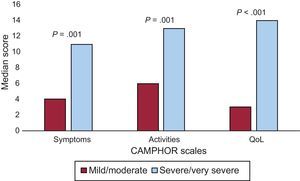
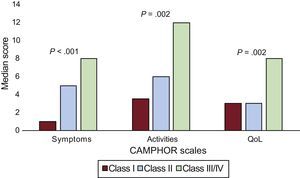
Figure 1, Figure 2, and Figure 3 show the results of the known group validity analyses. Participants who rated their health as “very good”/“good” reported significantly lower levels of symptoms and disability as well as higher levels of QoL than participants who rated their health as “fair”/“poor” (Figure 1). Similar differences were found between participants who perceived their PH to be “mild”/“moderate” vs those who perceived their PH as “severe”/“very severe” (Figure 2). In terms of the WHO classification, participants in functional classes III/IV showed the highest scores in all CAMPHOR scales, indicating more symptoms and disability and lower QoL (Figure 3).
This study shows that the adaptation of the CAMPHOR for use in Spain was successful. The Spanish translation was well accepted by interviewees and worked well in the postal survey. The psychometric quality of the measure proved high in the validation study.
The availability of the Spanish CAMPHOR will likely have a positive impact on both research and clinical practice in the Spanish PH population. The CAMPHOR has been shown to be a useful tool in outcome evaluation and cost/benefit analysis, due to its good responsiveness to change in QoL status.29 The measure should also facilitate communication and joint decision-making in everyday clinical practice between patients and clinicians. It has been previously reported that some endpoints may not accurately capture the way patients actually feel,30 and treatment may not result in the same level of benefit across patients. Therefore, the broad scope of aspects covered by the CAMPHOR may assist clinicians in the management and monitoring of patients.
LimitationsThis study should be interpreted in light of some limitations. First, the sample of participants recruited for the study presented with relatively mild disease, with 75% in World Health Organization functional classes I and II. Second, most participants were members of a patient association and, consequently, they may have differed from nonmembers. Further studies are required to explore the true impact of PH on Spanish patients using the CAMPHOR and relevant clinical outcomes.
ConclusionsThe results presented in this study attest to the validity and reliability of the Spanish CAMPHOR. Given that the good psychometric properties found here match those obtained in other adaptation studies, it is likely that the measure will prove valuable in clinical practice and research.
FUNDINGFinancial support for this study was obtained from Ferrer through an unrestricted grant.
CONFLICTS OF INTERESTNone declared.
- –
Despite improvements in therapy and clinical management, pulmonary hypertension continues to be a disease with the potential to have a major impact on quality of life.
- –
Quality of life has become an increasingly important endpoint in PH clinical studies and clinical practice.
- –
The Cambridge Pulmonary Hypertension Outcome Review was specifically designed to assess HRQoL and quality of life in individuals with PH.
- –
The Spanish version of the Cambridge Pulmonary Hypertension Outcome Review is a valid and reliable instrument for the assessment of HRQoL and quality of life in Spanish patients with PH.
- –
The Cambridge Pulmonary Hypertension Outcome Review has demonstrated superiority over other instruments that have been previously used to assess QoL among PH patients.
This research would not have been possible without the collaboration of the National Association of Pulmonary Hypertension.