Selective and nonselective His-bundle pacing (HBP) has proven to have morbidity and mortality outcomes comparable or superior to those of conventional endocardial right-ventricular pacing and cardiac resynchronization therapy (CRT).1
Left bundle branch area pacing (LBBAP) is a feasible and safe alternative option in candidates for antibradycardia therapy or CRT and has also obtained similar outcomes to conventional pacing.2 The objective of this study was to compare electrocardiographic and pacing parameter outcomes between HBP and LBBAP at implantation and at 3 months.
A retrospective review was conducted of a prospectively studied cohort of consecutive patients scheduled for antibradycardia therapy and CRT who underwent cardiac device implantation by the same electrophysiologist and with the same learning curve in each group. HBP alone was performed during the first study period (January through December 2018) and LBBAP alone during the second study period (January through December 2019).
HBP was performed as described in the literature.3 For the LBBAP procedure, we based our criteria on those of Huang et al.4: left bundle pacing was defined as the presence of qR or rsR’ morphology in V1 and deep septal pacing as the presence of qs in V1.5
The QRS complex was recorded before and after implantation by another operator using a digital recording system at a speed of 100mm/s. Table 1 shows the success criteria for each technique.
Patients’ baseline characteristics and success criteria
| Success criteria * | HBP group | LBBAP group | |
|---|---|---|---|
| bQRS <120ms | <120 ms | ≤ 130 ms | |
| bQRS ≥ 120ms | Narrowing ≥ 20% or paced QRS <130 ms | Narrowing ≥ 20% or paced QRS <130 ms | |
| ABT | 51 (58.6) | 29 (64.4) | 22 (52.4) |
| CRT | 36 (41.4) | 16 (35.6) | 20 (47.6) |
| Variable | Total group (n=87) | HBP group (n=45) | LBBAP group (n=42) | P |
|---|---|---|---|---|
| Age, y | 76 (64-81) | 75.5 (62.5-82.5) | 76 (64.2-81) | .7 |
| Sex male, % | 53 (60.9) | 28 (62.2) | 25 (59.5) | .8 |
| HT | 67 (77) | 40 (89) | 27 (64.3) | <.01 |
| DM | 37 (42.5) | 21 (46.7) | 16 (38.1) | .42 |
| Heart disease | 46 (53) | 18 (40) | 28 (66.7) | <.05 |
| LVEF, % | 60 (35-60) | 60 (34.5-60) | 52.5 (34.7-60) | .47 |
| Depressed LVEF | 38 (43.7) | 17 (37.8) | 21 (50) | .25 |
| Dilated RA | 39 (44.8) | 21 (46.7) | 18 (42.9) | .72 |
| Dilated LA | 67 (77.3) | 34 (75.6) | 33 (78.6) | .74 |
| Previous device | 13 (15) | 8 (17.8) | 5 (11.9) | .44 |
| Sinus atrial rhythm | 69 (79.3) | 32 (71.1) | 37 (88.1) | .051 |
| PR interval, ms | 196 (178-234) | 192 (160-220) | 200 (180-238) | .28 |
| BBB | 49 (56) | 25 (55.5) | 24 (57.1) | .91 |
| QRS complex, ms | 145.5±44 | 148.3±48 | 142.5±38 | .54 |
| Wide QRS complex | 55 (63.2) | 28 (62.2) | 27 (64.3) | .84 |
| Therapy indication | .25 |
ABT, antibradycardia therapy; BBB, bundle branch block; bQRS, baseline QRS; CRT, cardiac resynchronization therapy; DM, diabetes mellitus; HBP, His-bundle pacing; HT, hypertension (high blood pressure); LA, left atrium; LBBAP; left bundle branch area pacing; LVEF, left ventricle ejection fraction; RA, right atrium.
The data are presented as No. (%), mean±standard deviation, of median [interquartile range].
Ninety procedures were performed (46 underwent HBP and 44 LBBAP) in 87 patients. Left bundle branch pacing was performed in 18 patients (40.9%) in the LBBAP group, and deep septal pacing in 26 (59.1%). Table 1 shows the patients’ baseline characteristics.
A successful outcome was obtained in 85% (77/90) of the implantations: 80.4% (n=37) in the HBP group and 90.9% (n=40) in the LBBAP group (P=.23). Among the 13 failures, 4 were in the LBBAP group and 9 were in the HBP group. Fluoroscopy time was shorter for LBBAP than for HBP (10 vs 17min, P <.001).
Similar complication rates were recorded at the 3-month follow-up between the HBP group (13%, n=6) and the LBBAP group (6.8%, n=3) (P=.48). Lead-related complications were observed in 5 (10.6%) in the HBP group (loss of capture in 2, macrodisplacement in 1, and a significant increase in pacing threshold in 2) vs 1 (2.3%) in the LBBAP group (macrodisplacement, P=.2).
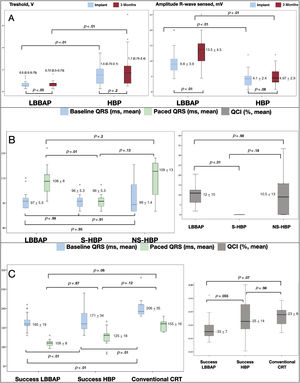
Nonselective HBP was obtained in 28 (75.7%) of the 37 patients and selective HBP in 9 (24.3%). The pacing threshold was lower and the sensed R-wave amplitude was higher in the LBBAP group at implantation and after 3 months. Threshold and amplitude were increased in both groups at 3 months vs baseline. The difference was statistically significance in the LBBAP group (figure 1A).
A: progress of pacing parameters. Left: pacing threshold in volts. Right: sensed R-wave amplitude in milivolts. At implantation and at 3 months. B: QRS width analysis in baseline QRS <120ms cases. Baseline QRS (blue box), paced QRS and QCI. C: QRS width analysis in baseline QRS ≥ 130ms cases. Baseline QRS, paced QRS and QCI. CRT, cardiac resynchronization therapy; HBP, His-bundle pacing; LBBAP; left bundle branch area pacing; NS-HBP: nonselective His bundle pacing; S-HBP: selective His bundle pacing.
In the 29 successful cases with a baseline QRS of <120ms (14 in HBP and 15 in LBBAP), the paced QRS was significantly increased (97.3±7.1 vs 105.5±10.3ms; P <.001) and the mean QCI was 8.7±10.5%, with a slightly lower increase in the HBP group (5.2±10.2% vs 12±10%; P=.08). Better results were obtained with selective HBP than with nonselective HBP or LBBAP (figure 1B).
In the 48 successful cases with a baseline QRS of ≥ 130ms (25 in LBBAP and 23 in HBP), 23 had right bundle branch block, 19 had left bundle branch block, and 6 had QRS paced by a previously implanted device. There was a trend (P=.055) toward a greater reduction of QCI with LBBAP vs HBP and an even greater reduction vs conventional CRT in failed cases (figure 1C).
Among the patients with left bundle branch block (12 in HBP and 11 in LBBAP), the success rate was 100% in the LBBAP group vs 66.7% in the HBP group (P=.09). Among successful cases, the paced QRS width was lower in the LBBAP group (112±9 vs 127±26ms; P=.16), although this difference was not statistically significant (figure 1). Among the patients with right bundle branch block (14 in HBP and 13 in LBBAP), the success rate did not differ between the HBP (85.7%) and LBBAP (84.6%) groups (P=1), but paced QRS was lower (106±7 vs 122±16ms; P <.01).
The main findings of this study were that narrower QRS complexes and better pacing outcomes were obtained at implantation and at 3 months with LBBAP than with HBP. Yiran Hu et al.6 described a similar success rate between LBBAP and HBP, although our population also included CRT indication. The radiological exposure time was shorter with the LBBAP technique because it does not require a search for the His-bundle electrogram (essential in HBP).
In conclusion, LBBAP achieves a narrower paced QRS, lower threshold, improved R-wave detection, and shorter fluoroscopy time with a similar complication rate compared with HBP.
CONFLICTO DE INTERESESM. Molina-Lerma and M. Álvarez have received honoraria from Medtronic. All other authors list no disclosures.
This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.