In late 2019, a new disease called coronavirus disease 2019 (COVID-19) emerged in China. The infection quickly spread to the rest of the world and a pandemic ensued. Spain has been one of the hardest-hit countries in terms of the number of cases and deaths. The entire health system has been put under stress and there has been a shift in the care of many diseases, including cardiovascular disease. There have been significant drops in the number of admissions for acute myocardial infarction (AMI) not only in Spain,1 but also in other countries such as the United States and Italy.2 A similar situation exists in relation to the number of primary angioplasties.3 The reasons for these drops are controversial. One of the hypotheses suggests that mortality from COVID-19 would constitute a competing risk.4 Many of the patients who experienced an AMI event would have died as a result of COVID-19 without the opportunity for the event to occur. Our study aim was to establish whether there is a relationship between deaths from COVID-19 in each of the Spanish Autonomous Communities (ACs) and the number of primary percutaneous coronary interventions (PCIs) recorded during the pandemic. We conducted a sensitivity analysis to compare the relationship between the excess total mortality recorded and variation in primary PCIs, given that an unknown number of patients without a confirmed diagnosis of COVID-19 probably died from this disease but were not counted.
To this end, we obtained data on primary PCIs recently published by the working group on the Infarction Code of the Interventional Cardiology Association of the Spanish Society of Cardiology (ACI-SEC), whose methodology has already been described.3 Briefly, primary PCIs performed in 73 Spanish interventional cardiology centers were compared in 2 time periods, the first before the start of the pandemic (February 24 to March 1, 2020) and the second after the start (March 16 to 22, 2020). These centers represent 90% of all Spanish centers performing this type of activity. We calculated the number of procedures per million population in each period and the difference between them to obtain the variation between the 2 periods (table 1). Data on mortality and excess mortality due to COVID-19 were obtained from the records of the Ministry of Health, the Carlos III Health Institute (ISCIII), and the Mortality Monitoring System (MoMo) of the ISCIII.5 Linear and nonlinear models were used to determine the association between mortality due to COVID-19, excess of total mortality, and variation in the rate of primary PCI per million population. R2 and significance levels were obtained for both models.
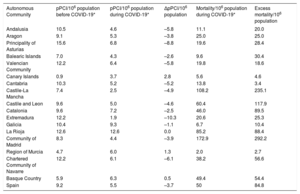
Primary PCI per million inhabitants, mortality, and excess mortality by Spanish autonomous community
| Autonomous Community | pPCI/106 population before COVID-19* | pPCI/106 population during COVID-19* | ΔpPCI/106 population | Mortality/106 population during COVID-19* | Excess mortality/106 population |
|---|---|---|---|---|---|
| Andalusia | 10.5 | 4.6 | –5.8 | 11.1 | 20.0 |
| Aragon | 9.1 | 5.3 | –3.8 | 25.0 | 25.0 |
| Principality of Asturias | 15.6 | 6.8 | –8.8 | 19.6 | 28.4 |
| Balearic Islands | 7.0 | 4.3 | –2.6 | 9.6 | 30.4 |
| Valencian Community | 12.2 | 6.4 | –5.8 | 19.8 | 18.6 |
| Canary Islands | 0.9 | 3.7 | 2.8 | 5.6 | 4.6 |
| Cantabria | 10.3 | 5.2 | –5.2 | 13.8 | 3.4 |
| Castile-La Mancha | 7.4 | 2.5 | –4.9 | 108.2 | 235.1 |
| Castile and Leon | 9.6 | 5.0 | –4.6 | 60.4 | 117.9 |
| Catalonia | 9.6 | 7.2 | –2.5 | 46.0 | 89.5 |
| Extremadura | 12.2 | 1.9 | –10.3 | 20.6 | 25.3 |
| Galicia | 10.4 | 9.3 | –1.1 | 6.7 | 10.4 |
| La Rioja | 12.6 | 12.6 | 0.0 | 85.2 | 88.4 |
| Community of Madrid | 8.3 | 4.4 | –3.9 | 172.9 | 292.2 |
| Region of Murcia | 4.7 | 6.0 | 1.3 | 2.0 | 2.7 |
| Chartered Community of Navarre | 12.2 | 6.1 | –6.1 | 38.2 | 56.6 |
| Basque Country | 5.9 | 6.3 | 0.5 | 49.4 | 54.4 |
| Spain | 9.2 | 5.5 | –3.7 | 50 | 84.8 |
Δ, variation; COVID-19, coronavirus disease 2019; pPCI: primary percutaneous coronary intervention.
The comparison showed that between the 2 periods the number of primary PCIs dropped in most ACs. There were marked differences in mortality and excess mortality between the ACs (table 1).
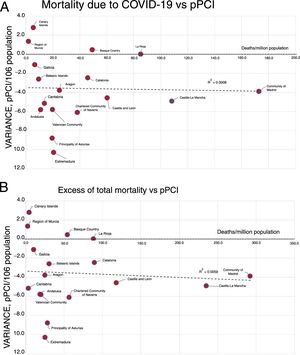
Neither of the models found a statistically significant association between mortality due to COVID 19 and variation in the primary PCI rate in the ACs (linear model: R2=0.008; P=.918; nonlinear model: logarithmic R2=0.068; P=.314; quadratic R2=0.07; P=.954; cubic R2=0.147; P=.744). The same strategy was used to determine associations between the excess of total mortality and variation in the PCI rate. Neither of the models found a statistically significant association between the variables (linear model: R2=0.0059; P=.771; nonlinear model: logarithmic R2=0.057; P=.356; quadratic R2=0.007; P=.952; cubic R2=0.021; P=0.963).
Mortality and variation in primary PCIs were plotted in the ACs (figure 1A). Although the Community of Madrid and Castile-La Mancha had the most deaths, they had drops in the primary PCIs rate that were similar to those in other ACs with lower mortality, such as Aragon or Cantabria, but lower than those in other ACs with much lower mortality, such as the Principality of Asturias or the Chartered Community of Navarre. No statistically significant association was found between the excess of total mortality and variation in the PCI rate (figure 1B).
A, Relationship between mortality due to COVID-19 and variation in the rate of pPCI/106 population. B, Relationship between excess mortality due COVID-19 and variation in the rate of pPCI/106 population. COVID-19, coronavirus disease 2019; pPCI: primary percutaneous coronary intervention.
The results suggest that it is unlikely that mortality from COVID-19, as a competing risk, explains the observed drop in the PCI rate or in admissions for AMI, although we cannot completely exclude this possibility. The real causes underlying this observation remain to be determined. It has been suggested that this finding may be due to a real reduction in AMI incidence or that fear of contagion in an overloaded health system would have discouraged AMI patients from seeking care.6 It is imperative to clarify this point in order to determine the real reasons for this situation and to avoid its repetition in the future.