We report the case of a 52-year-old man, ex-smoker, with no other cardiovascular risk factors, who was admitted for heart failure of 2 weeks’ duration. Chest x-ray showed cardiomegaly and bilateral alveolar edema. Electrocardiogram showed sinus tachycardia with left bundle branch block. The initial blood test suggested evolving myocardial infarction.
The patient received inotropic therapy, intravenous diuretic drugs, and noninvasive mechanical ventilation. Echocardiogram showed left chamber dilatation and severe ventricular dysfunction with anterior akinesia. Cardiac catheterization revealed nonrevascularizable severe 3-vessel coronary artery disease.
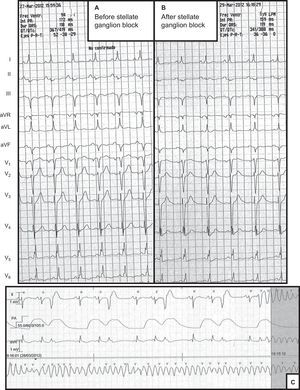
He was admitted to the coronary care unit, where he made slow but favorable progress. On the 10th day of admission, he underwent polymorphic ventricular tachycardia that was treated by defibrillation. No ischemic, electrolytic, or metabolic triggers or QT prolongation were identified that could explain the arrhythmia (Figure). Intravenous amiodarone was started, and within 12 h there were 13 episodes of ventricular tachycardia that were treated by defibrillation, intra-aortic balloon pump, endotracheal intubation, and mechanical ventilation. Beta blockers and lidocaine infusion were administered intravenously. Within 12 h there were multiple episodes of nonsustained ventricular tachycardia and 10 persistent episodes that were treated by defibrillation. Ablation was rejected due to extreme clinical instability.
Local anesthesia was applied to the left stellate ganglion as an additional measure of sympathetic block. Percutaneous puncture was performed using the anterior approach at the level of C6. Initially, 10 mL of 0.25% bupivacaine was injected, but the effectiveness of the block could not be assessed via the presence of Horner syndrome because the patient was under sedation and analgesia. There was an immediate response followed by the disappearance of arrhythmic events within the next 6 h. Subsequently, the persistent episodes reappeared, which were considered to be related to the diminishing effect of the local anesthetic used to create the sympathetic block. To address this, a new echocardiography-guided puncture was performed and the catheter inserted using a pediatric epidural needle to deliver a continuous infusion of 0.2% ropivacaine at 8 mL/h. Within the next 24 h the patient had 4 sustained ventricular tachycardias, representing an 82% reduction in events. Additional intravenous beta blockers were administered, antiarrhythmia drugs were maintained, and the infusion of ropivacaine was increased to 10 mL/h, with complete cessation of sustained arrhythmias.
After 4 days, the infusion of ropivacaine was withdrawn, without reappearance of the ventricular tachycardia. Hemodynamic stability was achieved, which permitted the removal of the intra-aortic balloon pump and extubation. Oral amiodarone and beta blockers were begun. Hospital stay was prolonged due to nosocomial ventilator-associated pneumonia and ischemia in the right lower limb, which was the insertion site of the intra-aortic balloon pump. A cardiac resynchronization therapy-implantable cardioverter-defibrillator was implanted on the 40th day and the patient was discharged home after 60 days of hospitalization. Ablation was rejected at admission due to the poor state of the patient, as well as the risks inherent to the procedure, its variable efficacy, and its dependence on the experience of the center. At 8 months follow-up, the patient had not had another arrhythmic event.
We define electrical storm as more than 3 episodes of ventricular tachycardia or ventricular fibrillation within 24 h. Treatment involves aggressive therapies, such as intra-aortic balloon pump, sedation, mechanical ventilation, and, occasionally, ablation of the arrhythmia substrate.
Sympathetic hyperactivity favors the onset and maintenance of ventricular arrhythmias.1 In the 1970s, sympathetic block in the management of ventricular arrhythmias was proposed for the treatment of congenital long QT syndrome resistant to treatment with beta blockers.2 In 1983, Lombardi et al.3 showed that increased sympathetic tone in the setting of coronary ischemia reduces the ventricular fibrillation threshold, and thus sympathetic block in this setting would reduce adverse ventricular events.
Nademanee et al.4 described the addition of left stellate ganglion block to sedation and antiarrhythmic treatment in patients with acute myocardial infarction without cardiogenic shock or acute pulmonary edema. They found that in 49 patients with acute myocardial infarction, a sympathetic block procedure that included the left stellate ganglion was associated with lower mortality, which was maintained at 1 year of follow-up. Mahajan et al.5 reported the use of the left stellate ganglion block in acute ischemic heart failure in an isolated case. Bourke et al.6 subsequently described a highly selected group of 14 retrospectively identified patients with very frequent or constant ventricular arrhythmia who underwent sympathetic block. Sympathetic block was performed using thoracic epidural anesthesia or video-assisted thorascopic left cardiac sympathetic denervation. The authors observed a significant reduction in the number of arrhythmia episodes.6
This case shows that sympathetic block achieved by the combined use of beta blockers and the infusion of local anesthetic via catheter to the stellate ganglion is a therapeutic alternative in electrical storm. This should be the subject of further studies with larger cohorts of patients.