To the Editor:
Peripartum cardiomyopathy is a rare, but severe, cause of heart failure. We present the magnetic resonance imaging findings of a patient diagnosed with peripartum cardiomyopathy.
A 30-year-old woman with no history of heart disease was admitted to our hospital for congestive heart failure symptoms a month and a half after an uncomplicated delivery. Echocardiography showed moderate dilatation of the left ventricle (end-diastolic diameter, 64 mm; end-systolic diameter, 46 mm) along with generalized hypokinesia and left ventricular ejection fraction of 32%; the left atrium was slightly dilated and the right chambers, at the upper limit of normal. Moderate-to-severe mitral and tricuspid regurgitation was observed in structurally normal valves. The estimated systolic pulmonary arterial pressure was 46 mm Hg. After stabilization, cardiac magnetic resonance imaging confirmed moderate dilatation of the left ventricle with ejection fraction 37%, as well as generalized hypokinesia of the right ventricle with severely depressed general systolic function (ejection fraction, 25%). Myocardial gadolinium late-enhancement study showed extensive linear mesocardial deposits at the septal level. Coronary angiography showed no coronary lesions. Based on a diagnosis of peripartum cardiomyopathy, the patient was transferred to the heart failure unit. After a year and a half of follow-up, the patient remained in NYHA functional class I-II with improved left ventricular ejection fraction (45% when last recorded).
The patient met the 4 criteria accepted for the diagnosis of peripartum cardiomyopathy: development of heart failure in the final month of pregnancy or within 5 months after delivery, absence of an identifiable cause for the onset of heart failure, absence of primary cardiac disease in the final month of pregnancy, and demonstrable systolic ventricular dysfunction according to the classic echocardiography criteria.1
Many theories attempt to explain the onset of this disease, although the most widely accepted hypothesis suggests that the condition originates in myocarditis.2 The diminished immune response that occurs during pregnancy would favor the development of the infectious process along with a late inflammatory response.
The definitive diagnosis of myocarditis is based on endomyocardial biopsy (Dallas criteria).3 Nevertheless, this test has limitations due to low sensitivity (in the acute stage, myocardial involvement shows a patchy distribution and is not risk-free).4
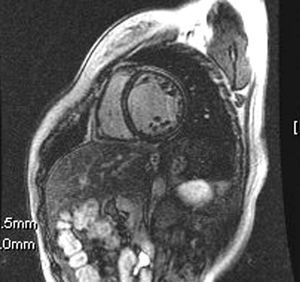
Cardiac magnetic resonance imaging has been recently developed for the diagnosis of myocarditis, both in the acute phase and in later phases.4 In the acute phase, gadolinium late-enhancement is evident in the epicardial area (initial hours or days), predominantly on the lateral aspect of the left ventricle and with a patchy distribution. In more advanced phases, gadolinium enhancement is more homogeneous along the entire ventricular wall. In our patient, contrast enhancement in the late phase during the chronic stage was extensive and showed septal predominance (Figure). These findings are consistent with those described in myocarditis series, which would indicate a common pathophysiological process for both entities. Gadolinium late-enhancement would indicate an increase of inflammatory activity in this condition. Although similar findings have been observed in patients with dilated cardiomyopathy,5 the recovery of ventricular function after discharge led us to consider peripartum cardiomyopathy, instead of dilated cardiomyopathy, which becomes clinically evident during the stress of pregnancy and puerperium.
Figure. Short-axis view after gadolinium administration, which shows myocardial late-enhancement which was linear at the septal intraparietal and probable lateral subepicardial level.