Keywords
INTRODUCTION
Very late stent thrombosis (VLST), that which occurs more than a year after implantation, has recently been described and studied because of the growing use of first generation drug-eluting stents (DES). The incidence usually ranges between 0.4% and 0.6% per year, and the major mechanism involved in the pathophysiology of VLST of a DES is incomplete endothelialization.1,2 Very late stent thrombosis of bare-metal stents (BMS) is a very uncommon complication outside the context of brachytherapy and the underlying pathophysiological mechanisms are little known.3 Our objective is to provide an in-depth evaluation of the pathophysiological knowledge of this complication by describing the intravascular findings revealed by intravascular ultrasound (IVUS) and its histological correlation of the samples collected after manual thrombectomy in 5 patients with definitive thrombosis after implantation of a BMS. Likewise, we provide a brief review of the literature dealing with the IVUS findings related to VLST following implantation of a BMS.
METHODS
We studied 5 patients with an acute coronary syndrome acute coronary syndrome and ST segement elevation secondary to VLST of a BMS. All of them underwent an emergency primary percutaneous coronary intervention. Once the angioplasty guidewire had passed through the thrombotic lesion, manual thrombectomy was performed using the Export device (Medtronic). In 1 case, the catheter did not pass through the lesion and balloon dilatation was performed. An IVUS study was carried out after thrombectomy in 4 patients and following balloon dilatation in 1. We used the IVUS findings to guide the interventional procedure, which ended with implantation of a stent-in-stent in 4 patients and dilatation with a noncompliant balloon alone in 1. Abciximab was administered in every case and the outcome was satisfactory, with Thrombolysis in Myocardial Infarction (TIMI) grade 3 flow and optimal myocardial perfusion.
For the histological study, the samples were fixed in 4% formaldehyde for at least 7 days and embedded in paraffin; 4.3-µm sections were obtained and stained with hematoxylin and eosin. Recent thrombus was defined as that composed of platelets and polymorphonuclear cells agglutinated by fibrin and mixed with the red blood cells. In the most highly developed thrombus, we observed a more compact agglutination of the polymorphonuclear cells, in which the nuclei are fragmented and the platelets replaced by fibrin.4 A fragment of an atherosclerotic plaque was defined as the part of the necrotic core with calcium and the presence of macrophages with lipids in the cytoplasm.
RESULTS
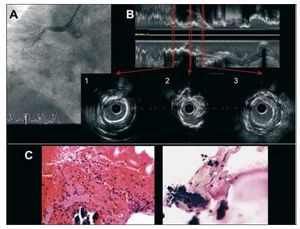
Table 1 shows the clinical, intravascular, and... and histological findings in each patient. All were men, with a mean age of 69 (11) years, and were receiving indefinite antiplatelet therapy. The lesion was located in the mid-segment of right coronary artery in 2 cases, in the proximal segment of the first diagonal branch in another 2 and in the middle segment of left anterior descending artery in the fifth. The mean time elapsed between the initial procedure and the thrombotic event was 7 (4) years. The angiographic finding was complete stent occlusion in all the patients. The IVUS revealed: de novo atherosclerosis with severe circumferential and surface calcification at the level of the stent, with ulcer and remains of the fibrous capsule indicative of plaque rupture (Figure 1) and a complex plaque with an intraluminal thrombus on the distal edge of the stent, with moderate instent proliferation (Figure 2). In another patient, we observed underexpansion of the stent with mild proliferation and, finally, in the other 2 patients, a severe neointimal proliferation predominated (Figure 3).
Figure 1. Corresponds to patient no. 1 in Table 1. A: angiogram showing complete occlusion at the level of the middle segment of right coronary artery. B: intracoronary ultrasound image with longitudinal reconstruction and transverse section. Section no. 1 shows in-stent circumferential surface calcification. Section no. 2 shows a ruptured plaque with remains of the fibrous capsule and, finally, section no. 3 shows mild neointimal proliferation. C: thrombus frargments with polymorphonuclear cells with preserved nuclei and remains of an atheromatous plaque (H-E, x200). The calcium is seen as bluish amorphous material around which we observe macrophages with cytoplasm microvacuolated by the presence of lipids, corresponding to a ruptured atheromatous plaque (H-E, x400).
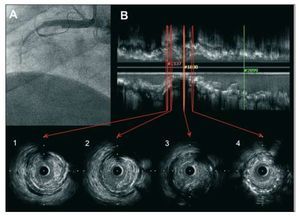
Figure 2. Corresponds to patient no. 2 in Table 1. A. angiogram showing complete occlusion at the level of the middle segment of right coronary artery. B: intracoronary ultrasound image with longitudinal reconstruction and transverse sections. Sections 1 to 3 show a complex plaque with rupture and thrombotic material on the distal stent edge. Section 4 shows moderate neointimal proliferation.
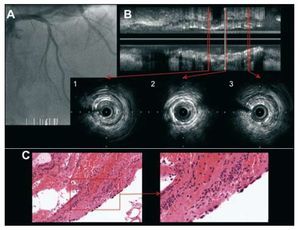
Figure 3. Corresponds to patient no. 4 in Table 2. A: angiogram showing complete occlusion in proximal segment of first diagonal branch. B: intracoronary ultrasound image with longitudinal reconstruction and transverse sections. The transverse sections show severe neointimal proliferation with distal underexpansion of the stent. C: fragments of old thrombus with lysis of the nuclei of the polymorphonuclear cells and surface endothelialization (H-E, x200). At greater magnification, we see endothelial cells of the in-stent neointima (H-E, x400).
The histological findings were concordant with those of IVUS. In every case, there was a recent thrombus; in 2 cases, an old thrombus predominated; in 1 case, the remains of an atheromatous plaque were removed; and, in another case, we found the remains of neointimal proliferation.
DISCUSSION
The 2 pathophysiological mechanisms of VLST in a BMS suggested in this study are the development and progression of de novo atherosclerosis within the stent or on its edges, as well as in-stent neointimal proliferation. These factors differ from the mechanisms involved in late or very late DES thrombosis. The major local mechanism associated with VLST in DES are incomplete and delayed endothelialization of the stent, alone or in combination with chronic inflammation and a hypersensitivity reaction that results in positive arterial remodeling and incomplete apposition.5,6 Other factors reported for VLST in DES are underexpansion and penetration of the stent into the necrotic core, mainly in patients with acute coronary syndrome.5,6
Very late stent thrombosis is a rare complication in BMS and very few cases have been reported.3,7-12 Table 2 shows the 8 cases that we have found that describe the use of IVUS. Our series with the description of the IVUS and histological findings is the largest reported to date. In all the cases that appear in the literature, the underlying mechanism is neointimal proliferation, except in 2 in which the mechanism described is stent malapposition. In our series, neointimal proliferation was the major finding in 3 patients, in 2 of whom we observed severe neointimal proliferation, whereas in the third, it was mild. The stenosis produced by progressive neointimal proliferation can promote the formation of an in-stent thrombus. Another explanation that we consider more improbable, although it has been reported, is regression of the neointima and its possible fracture and the subsequent thrombus formation.13
The other mechanism that we describe is the progression of atheroclerosis within the in-stent neointima or on the edges. In the literature, we have found no description of plaque rupture due to IVUS within the neointima, although there is 1 case with angiographic and histological documentation using material collected by means of thrombectomy.14 Our series includes a case with plaque rupture in the context of de novo atherosclerosis within the instent neointima and another case of atherosclerotic plaque rupture on the distal edge of the stent. The formation and progression of atherosclerosis in the in-stent neointima probably requires the passage of several years. In the cases in our series in which there was complicated atherosclerosis within the stent or on its edges, 90, 110, and 120 months had elapsed. In contrast, in those cases in which neointimal proliferation is identified as the major mechanical mechanism, the time to the event was much shorter (15 and 63 months).
All of the patients in our series were being treated indefinitely with an antiplatelet agent and had dual antiplatelet therapy during the first month after implantation. In contrast to the case of DES, it is not clear whether the indefinite prolongation of dual antiplatelet therapy is capable of preventing VLST in BMS.
Finally, it is important to perform an intracoronary imaging technique such as IVUS to obtain information on the mechanism of the thrombosis, with a view to percutaneous treatment during the event. Thus, when there is atherosclerosis within the stent or on the edges and severe restenosis, the implantation of another stent makes it possible to obtain an optimal result. If what predominates is the thrombus with mild restenosis, related or not to underexpansion, the outcome can be optimized by means of balloon dilatation without implantation of a new stent.
To conclude, the findings of this study indicate that the pathophysiology of VLST in BMS may differ from that associated with DES. The progression of atherosclerosis within the stent or on the edges and neointimal proliferation are the major factors in the development of VLST in BMS.
Correspondence: Dr. Á. Sánchez-Recalde.
Unidad de Hemodinámica y Cardiología Intervensionista, Planta 1.a Diagonal, Hospital General Universitario La Paz.
P.o de la Castellana, 261. 28046 Madrid. Spain
E-mail: recalde@secardiologia.es
Received November 2, 2009.
Accepted for publication January 7, 2010.