To the Editor:
Due to the elevated rate of mortality with which it is associated, left ventricular (LV) free wall rupture is a dreaded complication of acute myocardial infarction (AMI). The incidence is especially high during the first 24 hours, after which it decreases progressively; beyond the fifth day post-AMI, this complication is uncommon. The onset is usually acute, in the form of cardiac tamponade, although it can be subacute.1 The major risk factors are female sex, advanced age, complete obstruction of the infarct-related artery, and previous AMI.2 Although coronary anatomy (reperfusion of the infarct-related artery and absence of collateral circulation) is the key predictive factor,2,3 in most cases, previous coronary arteriogram is not available.1 Moreover, primary angioplasty reduces the risk of LV free wall rupture as compared to fibrinolysis.4
We report the case of a 72-year-old hypertensive man, an ex-smoker, who had had an inferior AMI in 1999 that was treated with fibrinolysis; the pre-discharge exercise test was normal. He was asymptomatic from that time until 4 days prior to his admission to our center, when he began to note tightness in the middle of his chest, despite which, he remained at home for more than 36 hours. Four days after the onset of symptoms, he was referred to our center, where he told us that he was asymptomatic. The electrocardiogram revealed the presence of inferior and lateral Q waves, and inverted T waves were observed in V5-V6. Laboratory studies showed a total creatine kinase (CK) concentration of 1400 U/L, CK-MB isoenzyme of 150.2 U/L, and troponin T of 22 ng/mL.
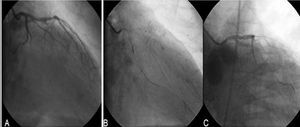
The next day, catheterization evidenced apical akinesia, posterobasal hypokinesia and a preserved ejection fraction. Heparin (9000 units) was administered, but glycoprotein IIb/IIIa inhibitors were not employed. We observed a 90% lesion in right coronary artery, which was treated with direct stenting, and complete obstruction of the second marginal artery, which was small in diameter. This artery was recanalized using a floppy guide wire (Galeo HF 0.014) and angioplasty was performed with a Crossail balloon (1.5x20 mm) (Figure 1). A few seconds later, the patient developed syncope with severe hypotension and bradycardia. When the balloon was withdrawn, passage of the contrast material to the distal arterial bed was observed, but there was no passage to the pericardium. Pericardiocentesis was carried out as electromechanical dissociation secondary to tamponade was suspected. Echocardiography performed once pericardiocentesis had begun confirmed the presence of tamponade and revealed ventricular rupture. After 30 minutes of advanced resuscitation maneuvers, death occurred.
Figure 1. Images of the catheterization. A: complete obstruction of the second marginal branch of the circumflex artery. B: recanalization of the second marginal branch. C: hemodynamic deterioration following angioplasty in the second marginal branch.
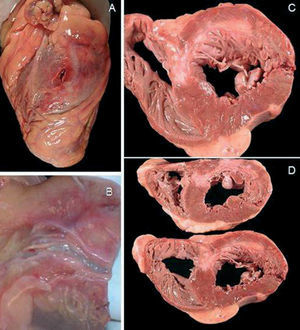
This case is of interest because it involves a fully evolved infarct in a man with a second AMI for whom coronary arteriogram performed prior to the development of the complications was available. In the presence of tamponade, it was necessary to rule out arterial or ventricular rupture. We provide the images of the LV free wall rupture and the intact marginal artery (Figure 2). With regard to the etiology of rupture occurring seconds after revascularization, we can not exclude the effect of acute reperfusion injury5 or the possible presence of the rupture prior to the procedure, since echocardiography had not previously been performed. Most ruptures are produced in cases of late or unsuccessful reperfusion or prior to reperfusion.6 We consider that the case reported here highlights the importance of reperfusion injury and partial or aborted ruptures.
Figure 2. Macroscopic images of the necropsy. A and C: left ventricular free wall rupture. B: intact marginal artery. D: previous inferior infarction and left ventricular free wall rupture.