Over the last 20 years, researchers have accumulated extensive evidence to support the theory that production of oxidants and reactive oxygen species in the postischemic heart is considerably elevated by different types of interaction between the heart and endothelial cells.1 The most accepted theory is the one that implicates oxidative stress with production of reactive oxygen species.2
Heart surgery and, specifically, cardiopulmonary bypass (CPB) is an ideal situation for studying ischemia-reperfusion injury as long-lasting ischemia occurs followed by controlled reperfusion.3,4 The objective of this study was to analyze the changes in measures of oxidative stress and lipid peroxidation in pediatric patients who underwent cardiovascular surgery in order to shed light on the management of ischemia-reperfusion in future surgery.
The study included patients younger than 15 years who underwent congenital heart surgery with CPB. Malondialdehyde (MDA), total glutathione (GST), and glutathione in its reduced (GSH) and oxidized (GSSG) states were measured (nmol/mg of protein). Samples for analysis were taken in the preoperative period (PRE), the immediate postoperative period (PO1), and the late postoperative period (PO2) after 18 to 20hours. New variables representing the percentage change in oxidative stress between PRE and PO1 (_p1), PO1 and PO2 (_p2), and PRE and PO2 (_p3) were derived to investigate the correlation between oxidative stress and time in relation to surgery.
Thirty children (19 girls [63.3%]) were included with a median [interquartile range] age of 4.1 [2.7-8.0] years. The surgery types were as follows: 11 closures of atrial septal defects, 2 pulmonary stenosis interventions, 3 total corrections of tetralogy of Fallot, 3 corrections of atrioventricular canal defect, 6 closures of ventricular septal defects, 2 aortic stenosis interventions, 2 corrections of univentricular hearts (one using the Glenn technique and the other using the Fontan technique), and 1 surgical correction of transposition of the great arteries. The median total CPB time was 79 [52.5-125.5] minutes, which was slightly lower than in other series,5 and the median aortic clamp time was 38.5 [22-59] min.
Table 1 shows that the production of MDA was significantly increased and the production of different states of glutathione significantly reduced at each postoperative time point compared with baseline. The Friedman nonparametric test was used to compare the measures of the antioxidant system (glutathione states) and lipid peroxidation (MDA), with statistically significant differences (P < .001). After multiple comparisons with the Wilcoxon test and application of the Bonferroni correction, MDA and GST differed significantly from each other (P<.016) at the 3 time points.
Values (nmol/mg Protein) of Measures of Antioxidant Defense and Lipid Peroxidation
| Sample times | GST | GSSG | GSH | MDA |
|---|---|---|---|---|
| 1 | 3.56 (0.77) | 0.33 (0.30) | 3.23 (0.78) | 0.15 (0.04) |
| 2 | 2.56 (0.71) | 0.23 (0.19) | 2.32 (0.69) | 0.21 (0.09) |
| 3 | 3.25 (0.66) | 0.27 (0.18) | 2.99 (0.71) | 0.18 (0.06) |
| Friedman test, P<.001. | ||||
| MDA2-MDA1 | MDA2-MDA3 | MDA1-MDA3 | GST2-GST1 | GST3-GST2 | GST1-GST3 | |
|---|---|---|---|---|---|---|
| Z | –3.713 | –3.157 | –3.096 | –4.618 | –4.371 | –2.808 |
| P | .0001* | .002* | .002* | .0001* | .0001* | .05 |
GSH, reduced glutathione; GSSG, oxidized glutathione; GST, total glutathione; MDA, malondialdehyde.
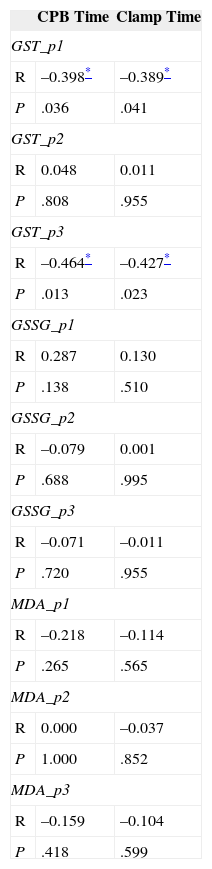
CPB time showed a certain significant correlation with some of the variables of oxidative stress (Table 2). Partial oxygen pressure in blood (to determine whether cyanosis associated with heart disease had any influence) did not correlate with changes in the measures of oxidative stress or lipid peroxidation.
Correlation Statistics for Cardiopulmonary Bypass and Clamp Times With Variables of Antioxidant Defense and Lipid Peroxidation (Pearson Correlation Coefficient [R] and Statistical Significance [P])
| CPB Time | Clamp Time | |
|---|---|---|
| GST_p1 | ||
| R | –0.398* | –0.389* |
| P | .036 | .041 |
| GST_p2 | ||
| R | 0.048 | 0.011 |
| P | .808 | .955 |
| GST_p3 | ||
| R | –0.464* | –0.427* |
| P | .013 | .023 |
| GSSG_p1 | ||
| R | 0.287 | 0.130 |
| P | .138 | .510 |
| GSSG_p2 | ||
| R | –0.079 | 0.001 |
| P | .688 | .995 |
| GSSG_p3 | ||
| R | –0.071 | –0.011 |
| P | .720 | .955 |
| MDA_p1 | ||
| R | –0.218 | –0.114 |
| P | .265 | .565 |
| MDA_p2 | ||
| R | 0.000 | –0.037 |
| P | 1.000 | .852 |
| MDA_p3 | ||
| R | –0.159 | –0.104 |
| P | .418 | .599 |
CPB, cardiopulmonary bypass; GSSG, oxidized glutathione; GST, total glutathione; MDA, malondialdehyde.
Knowledge of oxidative stress in heart surgery to date has been based largely on animal models. It is not known with any certainty which enzymatic redox systems have greatest influence on systemic inflammatory response. In the pediatric CPB model in this study, the genesis of oxidative stress and lipid peroxidation was observed. These reached a maximum after aortic clamping and improved after 24hours without returning to normal values. There were significant differences between PRE and PO2. Reactive oxygen species are highly toxic metabolites that lead to lipid peroxidation and damage to cell membranes, in turn leading to capillary leakage and the production of shock-induced adhesion molecules. This process can activate macrophages in the liver and cause the synthesis, when in a state of shock, of proinflammatory mediators such as tumor necrosis factor and interleukin.6 Lipid peroxidation is an important cause of oxidative damage of cell membranes and cell death. MDA is a good indicator of oxidative stress and an end product of lipid peroxidation. Glutathione is crucial as a cell defense mechanism against oxidative stress.
In addition to its antioxidant activity, GST plays an important role in transmembrane amino acid transport, protein synthesis and degradation, gene regulation, and cell redox regulation. GST mobilization has been shown to be increased in septic animals, with increased usage, by analogy with that seen in our model of CPB. Therefore, the possibility of modulating the availability of GST may be an attractive strategy but studies have yet to be conducted with clinically relevant outcomes.
A multivariate analysis (CPB time, clamp time, and age) was performed by linear regression to identify the factors that actually influence the laboratory indicators of oxidative stress and lipid peroxidation. Longer duration of CPB correlated with greater glutathione deficiency after 18 to 20hours. This was also reflected in the assessment of the percentage increase in glutathione between PRE and PO2.
One of the limitations of this study is that the sample size is small due to the nature of the surgery studied.
Investigation of oxidative stress in heart surgery offers a unique opportunity to make observations in clinically relevant conditions, given that knowledge to date has been derived from animal models. Such information may have important therapeutic implications, because preventing this phenomenon would afford greater myocardial protection and improve postoperative outcome.