This report presents the results of the 2013 Spanish Catheter Ablation Registry.
MethodsData were collected using 2 systems: retrospectively by completing a dedicated form and prospectively by reporting to a central database. Each participating center chose 1 of the 2 data collection methods.
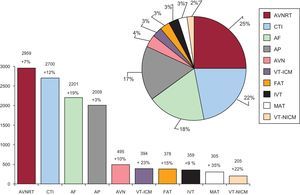
ResultsEighty centers voluntarily contributed data to the registry. A total of 11 987 ablation procedures were performed, with a mean (standard deviation) of 149 (105) procedures per center. The 3 main arrhythmic substrates treated were atrioventricular nodal reentrant tachycardia (n=2959; 24.6%), cavotricuspid isthmus ablation (n=2700; 22.5%), and atrial fibrillation (n=2201; 18.4%). The number of ventricular ablation procedures was similar to the 2012 activity, but there was a slight increase in procedures for scar-related postmyocardial infarction ventricular tachycardia. The success rate was 94.4%, major complications occurred in 1.8%, and the mortality rate was 0.03%.
ConclusionsIn line with previous reports, the data from the 2013 registry show a continuing increase in the number of ablations performed. Overall, there was a high success rate and few complications. Ablation of complex substrates has continued to increase.
Keywords
This article presents the 2013 Official Report of the Spanish Catheter Ablation Registry, developed by the Spanish Society of Cardiology Working Group on Electrophysiology and Arrhythmias and representing the 13th year of uninterrupted activity by this group.1–12 The registry is a voluntary nationwide effort that includes data submitted annually from the majority of arrhythmia units operating in Spain, making it one of the few available large-scale observational registries focusing on catheter ablation.
The main objectives of the registry are to observe and describe the developments occurring in the interventional treatment of cardiac arrhythmias in Spain and to provide reliable information on the facilities available in our arrhythmia units and the type of activity performed.
METHODSAs in previous years, data were collected using 2 different systems: a prospective method and a retrospective method. For the prospective approach, the registry provided a dedicated database and required patients to be included individually. The retrospective approach consisted in completing a standardized questionnaire sent to all participating interventional electrophysiology laboratories in January 2014; the questionnaire was also available on the Working Group on Electrophysiology and Arrhythmias website.13 All the data compiled using both systems remained anonymous, even to the registry coordinators. The Secretariat of the Spanish Society of Cardiology ensured that the participating centers could not be identified.
The information collected concerned the technical and human resources available in our arrhythmia units, the procedures performed, and the patients’ demographic data. As in previous years, the data on human resources only included information from centers in the publicly-funded health system, and the epidemiologic variables only included those from patients treated in centers using the prospective data collection method.
We analyzed the same 10 arrhythmic substrates as those collated in previous registries: atrioventricular nodal reentrant tachycardia (AVNRT), accessory pathway (AP), atrioventricular node ablation, focal atrial tachycardia (FAT), cavotricuspid isthmus, macroreentrant atrial tachycardia, atrial fibrillation (AF), idiopathic ventricular tachycardia, ventricular tachycardia in ischemic cardiomyopathy (VT-ICM) (ie, associated with postmyocardial infarction scarring), and ventricular tachycardia in nonischemic cardiomyopathy (VT-NICM) (ie, not associated with postinfarction scarring). The following variables common to all the substrates were analyzed: number of patients and procedures performed, success rate, type of ablation catheter used, and number and type of procedure-related complications, including periprocedure death. In addition, we analyzed a number of substrate-specific variables, such as the anatomic location and type of accessory pathway-mediated arrhythmia, the location and mechanism of atrial tachycardia, and the type of ventricular tachycardia.
As in previous years, the success rate refers only to the immediate postprocedure data (acute success rate). The number of recurrences is unknown because there was no follow-up analysis. Various therapeutic approaches with different objectives are available to treat AF, VT-ICM, and VT-NICM, and the criteria for success/failure may differ according to the technique applied. Hence, these substrates were excluded from the overall outcome analysis of ablation procedures. As to complications, only those occurring during hospitalization following the procedure were notified.
Statistical AnalysisQuantitative variables are expressed as the mean (standard deviation). Differences between quantitative variables were evaluated using the Student t test for dependent or independent samples, as appropriate. Differences between categorical variables were assessed using the chi-square or Fisher exact test. Statistical significance was set at a P value of <.05. The statistical analysis was carried out using an SPSS (15.0) database.
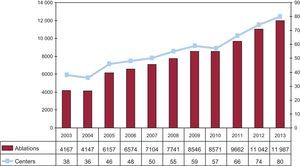
RESULTSIn keeping with the general trend over the last few years, there was a significant increase in the number of centersparticipating in the registry and the total number of ablation procedures performed. Eighty centers contributed to the 2013 registry (Appendix 2), and for the first time, nearly 12 000 ablation procedures were notified (Figure 1). The participating centers included 64 (80%) from the public healthcare system and 16 from the private sector.
As has been the case since the founding of the registry, the retrospective approach was the most widely used system for data collection. Only 8 sites(10%) collected data prospectively.
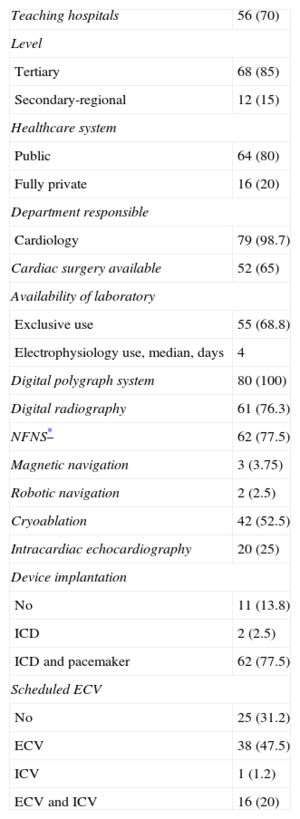
The participating hospitals were mainly third-level (85%) and teaching (70%) centers. Patients were attended in cardiology departments in 79 of the 80 participating centers (98.7%), and 65% had cardiac surgery units (Table 1).
Characteristics and Infrastructure of the 80 Electrophysiology Laboratories Participating in the 2013 Registry
| Teaching hospitals | 56 (70) |
| Level | |
| Tertiary | 68 (85) |
| Secondary-regional | 12 (15) |
| Healthcare system | |
| Public | 64 (80) |
| Fully private | 16 (20) |
| Department responsible | |
| Cardiology | 79 (98.7) |
| Cardiac surgery available | 52 (65) |
| Availability of laboratory | |
| Exclusive use | 55 (68.8) |
| Electrophysiology use, median, days | 4 |
| Digital polygraph system | 80 (100) |
| Digital radiography | 61 (76.3) |
| NFNS* | 62 (77.5) |
| Magnetic navigation | 3 (3.75) |
| Robotic navigation | 2 (2.5) |
| Cryoablation | 42 (52.5) |
| Intracardiac echocardiography | 20 (25) |
| Device implantation | |
| No | 11 (13.8) |
| ICD | 2 (2.5) |
| ICD and pacemaker | 62 (77.5) |
| Scheduled ECV | |
| No | 25 (31.2) |
| ECV | 38 (47.5) |
| ICV | 1 (1.2) |
| ECV and ICV | 16 (20) |
ECV, external cardioversion; ICD, implantable cardioverter-defibrillator; ICV, internal cardioversion; NFNS, nonfluoroscopic navigation system.
Unless otherwise indicated, data are expressed as No. (%).
As in previous registries, the analysis of epidemiologic characteristics included only data from sites using prospective data notification. This year there were 8 such centers (as in 2011 and 2012), providing data on 1787 ablation procedures.
The patients’ mean age was 43 (15) years. According to the procedures performed, the youngest patients (37 [10] years) underwent AP ablation and the oldest (74 [8] years) atrioventricular node ablation. Most AVNRT ablation procedures were carried out in women (80%), whereas ablation of AF and ventricular tachycardia was mostly conducted in men (75% and 71%, respectively), associated or not with structural heart disease. These data are virtually identical to those reported in previous registries.
Also consistent with previous findings, 41% of patients had a history of structural heart disease, and left ventricular dysfunction was mainly limited to patients undergoing atrioventricular node ablation and heart disease-associated ventricular tachycardia ablation. The same distribution was seen in the group of patients with automatic implantable cardioverter defibrillators.
Infrastructure and ResourcesThe technical and human resources available in arrhythmia units participating in the 2013 registry and the activity carried out are presented in Tables 1 and 2.
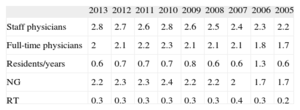
Changes in the Human Resources in Public Health System Electrophysiology Laboratories Participating Since 2005 (Mean No. per Hospital)
| 2013 | 2012 | 2011 | 2010 | 2009 | 2008 | 2007 | 2006 | 2005 | |
| Staff physicians | 2.8 | 2.7 | 2.6 | 2.8 | 2.6 | 2.5 | 2.4 | 2.3 | 2.2 |
| Full-time physicians | 2 | 2.1 | 2.2 | 2.3 | 2.1 | 2.1 | 2.1 | 1.8 | 1.7 |
| Residents/years | 0.6 | 0.7 | 0.7 | 0.7 | 0.8 | 0.6 | 0.6 | 1.3 | 0.6 |
| NG | 2.2 | 2.3 | 2.3 | 2.4 | 2.2 | 2.2 | 2 | 1.7 | 1.7 |
| RT | 0.3 | 0.3 | 0.3 | 0.3 | 0.3 | 0.3 | 0.4 | 0.3 | 0.2 |
NG, nursing graduate; RT, radiologic technologist.
Fifty-five centers (68.8%) were equipped with at least 1 dedicated cardiac electrophysiology laboratory, and 9 centers (11.2%) had 2 laboratories. As in previous years, the laboratory was available for 3.7 (1.4) [median, 4] days per week. Only 4 of the 16 private centers had a room exclusively devoted to cardiac electrophysiology activity.
External electric cardioversion was performed in 54 laboratories and internal cardioversion in only 16 of these centers. According to the data notified, 1 site carried out internal cardioversion alone. In a larger percentage than in 2012 (86.2%), most units were outfitted to perform cardiac pacing device implantation, mainly defibrillators: implantation of both defibrillators and pacemakers was performed in 77.5% of laboratories, defibrillator implantation alone in 2.5%,and pacemaker implantation alone in 3.8%.
All the participating centers were equipped with a digital polygraph system, 76.3% digital radiography, and 46.6% portable fluoroscopy. A single nonfluoroscopic navigation system was available in 77.5% of centers, 20 sites had 2 such systems, and 3 sites had 3. Although the differences are smaller than in the previous registry, nonfluoroscopic navigation systems were more widely available in public healthcare centers than in private ones (85.2% vs 50.0%).
The number of remote navigation systems was slightly lower than in previous years. Three centers had a magnetic navigation system and 2 a robotic navigation system. The number of sites performing intracardiac echocardiography has also decreased (20, representing a reduction from 35.6% to 25.0% relative to 2012). Ultrasound ablation remained available at a single site, but cryoablation was incorporated in a significantly larger number of centers (42, representing an increase from 45.9% to 52.5% relative to 2012).
The number of healthcare professionals (physicians, nursing graduates, and resident physicians) working in electrophysiology laboratories was slightly lower than in previous years, despite the growing number of ablation procedures performed. In total, 65.3% of centers had more than 1 full-time physician, and 30.7%, more than 2. Of note, 10 healthcare centers had 4 staff physicians working full-time in electrophysiology laboratories. At least 2 full-time nursing graduates were on the staff of 75.6% of laboratories. Thirty centers hadresident physicians, at an average of 1.6 residents per site (1 hospital had 8 residents).
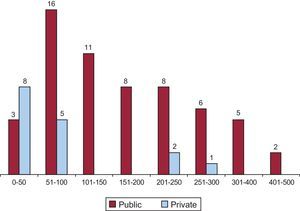
Overall ResultsIn 2013, 80 centers submitted catheter ablation data to the registry, the highest level of participation since its inception (Figures 1 and 2). In total, 11 987 procedures were reported, yielding a mean of 149 (105) procedures (median, 120; range, 9-486) procedures per site. Only 8 private centers performed more than 50 ablation procedures per year, and 3 of them exceeded 200 per year. Seven public health centers carried out more than 300 ablation procedures (2 of them, more than 400).
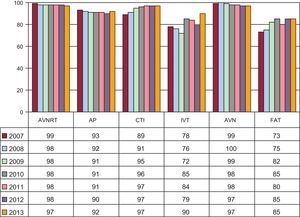
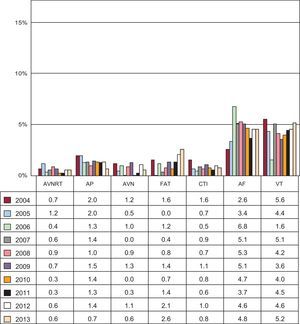
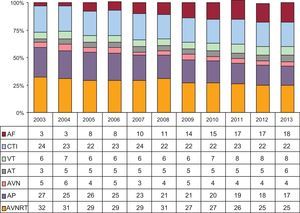
The overall success rate was 94.4% (8728 of 9246), excluding treatment of AF, VT-ICM, and VT-NICM. Among the total number of ablation procedures performed (including AF, VT-ICM, and VT-NICM), 225 complications were notified, yielding a rate of 1.8%. Four deaths were recorded (0.03%) in the following procedures: 1 AF ablation due to an atrioesophageal fistula with a fatal outcome; 2 VT-ICM ablations in which death was not immediate, but occurred due to refractory heart failure after the procedure, and 1 VT-NICM ablation, with death also secondary to heart failure. There were 13 cases of iatrogenic atrioventricular block (0.1%) requiring permanent pacemaker implantation: 5 during AVNRT ablation, 3 during AP treatment, 2 during cavotricuspid isthmus ablation, 1 during macroreentrant atrial tachycardia treatment, and 2 during VT-ICM ablation. The overall 2013 results for procedure success and complications compared with the 2011 and 2012 rates are shown in Figures 3 and 4. The success rates for the various substrates have held steady, with the exception of procedures for ventricular tachycardia in heart disease in general, which decreased from 77% to 69%. This reduction may be related to the criteria used to determine success, which differs between laboratories for these arrhythmias. The incidence of complications relative to 2012 has shown a general trend to reductions in all substrates; of particular note is the decrease associated with atrioventricular node and AP ablation procedures, although a slight increase was seen in procedures for FAT and ventricular tachycardia. The AVNRT remained the most frequently treated substrate, followed by cavotricuspid isthmus ablation. In contrast to data in the 2012 registry and for the first time, AF was the third most commonly treated substrate (Figure 5). The number of ablation procedures has risen for all the substrates, including VT-ICM, which showed a 3% drop in 2012. The most significant increases occurred in treatment for macroreentrant atrial tachycardia and for ischemic and nonischemic cardiomyopathy-related ventricular tachycardia. The 18.8% increase in AF ablation procedures is somewhat smaller than the 2012 value. This treatment accounted for 18% of all ablation procedures performed and ranked third in order of frequency, ahead of AP ablation. VT-NICM ablation procedures remained the least common, although their number has increased considerably over the last few years. The changes occurring since 2003 in the relative frequency of procedures for the various arrhythmic substrates are shown in Figure 6.
Percentage of major complications related to catheter ablation since 2004 by substrate. AF, atrial fibrillation; AP, accessory pathway; AVN, atrioventricular node; AVNRT, atrioventricular nodal reentrant tachycardia; CTI, cavotricuspid isthmus; FAT, focal atrial tachycardia; VT, ventricular tachycardia.
Number and relative frequency of substrates treated by catheter ablation recorded in the 2013 registry. The percent change relative to the 2012 registry is shown for each substrate.
AF, atrial fibrillation; AP, accessory pathway; AVN, atrioventricular node; AVNRT, atrioventricular nodal reentrant tachycardia; CTI, cavotricuspid isthmus; FAT, focal atrial tachycardia; IVT, idiopathic ventricular tachycardia; MAT, macroreentrant atrial tachycardia/atypical atrial flutter; VT-ICM, ventricular tachycardia in ischemic cardiomyopathy; VT-NICM, ventricular tachycardia in nonischemic cardiomyopathy.
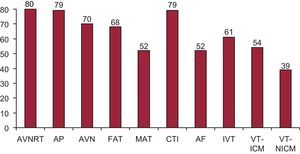
In 2013, AVNRT was the only substrate treated at all sites. According to the data submitted to analysis, AP ablation was not performed in 1 center. Cavotricuspid isthmus was treated in 98.8% and atrioventricular node in 85.2% of centers (Figure 7). VT-NICM remained the substrate treated at the smallest percentage of sites (48.7%). The number of centers performing AF ablation rose from 50 to 52; these represent 65.0% of all participating sites and 67.1% of those belonging to the public healthcare system.
Number of electrophysiology laboratories participating in the registry that treat each substrate. AF, atrial fibrillation; AP, accessory pathway; AVN, atrioventricular node; AVNRT, atrioventricular nodal reentrant tachycardia; CTI, cavotricuspid isthmus; FAT, focal atrial tachycardia; IVT, idiopathic ventricular tachycardia; MAT, macroreentrant atrial tachycardia/atypical atrial flutter; VT-ICM, ventricular tachycardia in ischemic cardiomyopathy; VT-NICM, ventricular tachycardia in nonischemic cardiomyopathy.
The following sections report the data analysis results for each specific arrhythmic substrate.
Atrioventricular Nodal Reentrant TachycardiaAtrioventricular nodal reentrant tachycardia was the condition treated most often, and catheter ablation of this substrate was carried out in all centers. A total of 2959 AVNRT ablation procedures were performed (24.7% of the total), with a mean of 37 (24) per site (range, 2-116). The overall success rate was 97.1% (2885 of 2971), and 51 centers (63.7%) had a rate of 100%. There were 17 complications (0.6%), including 5 cases (0.16%) of atrioventricular block requiring permanent pacemakers, and 6 (0.2%) vascular access complications.
The most commonly used ablation catheter was a conventional, 4-mm-tip radiofrequency catheter. An 8-mm-tip catheter was used in 17 procedures, an irrigated-tip catheter in 49, and a cryoablation catheter in 94 cases.
Cavotricuspid IsthmusCavotricuspid isthmus ablation was the second most frequent procedure, performed in 2700 cases (mean, 34 [26]). Success was reported in 2614 cases (97%) in 79 of the 80 centers (98.7%), with a 100% success rate in 40 centers. There were 23 major complications (0.9%): 18 vascular complications, 2 cases of atrioventricular block requiring permanent pacemakers, 1 episodeof stroke, and 1 case of heart failure. In contrast to the data from 2012, there were no deaths in 2013.
Use of 4-mm-tip ablation catheters for this condition was uncommon (2.8%). The devices employed included 1578 irrigated-tip, 979 8-mm-tip, 52 10-mm-tip, and 20 cryoablation catheters.
Accessory PathwaysFor the first time in the history of the registry, AF ablation overtook AP ablation in 2013, thus ranking AP ablation as the fourth most commonly performed procedure, carried out in all centers except 1. There were 2009 AP procedures, yielding a mean of 25 (17) per site (range, 1–91), and 1856 (92.4%) had a successful outcome. Twenty-three centers achieved a success rate of 100%. Nonetheless, on separate analysis of the 63 centers reporting more than 10 procedures, only 14 reached 100%. There were 14 (0.7%) major complications: 4 vascular complications, with 1 case of major bleeding requiring transfusion of blood products; 3 cases of atrioventricular block requiring permanent pacemakers; 3 pericardial effusions, and 2 strokes.
Nonconventional ablation catheters were used in 503 procedures: 343 irrigated tip, 87 cryoablation, and 35 8-mm tip.
Only 1 of the 79 centers performing AP ablation did not describe the location of the abnormal pathway. The percentages in this regard were similar to those of previous years. Left AP remained the most common location (49.8%), followed by inferoseptal (26.9%) and right (14.7%) AP. Perihisian pathways remained the least common (8.5%). Procedure success according to AP location was as follows: left ventricular free wall, 96.6%; right ventricular free wall, 91.7%; inferoparaseptal, 89.8%; and perihisian/anteroseptal, 83.9%. There were some improvements in outcome relative to the 2012 data.
Atrioventricular Node AblationIn total, 495 atrioventricular node ablation procedures were notified from 70 centers. Success was achieved in 97% of cases. There were 3 complications (0.6%), but only 1 center indicated the type, which involved the vascular access.
Nonconventional ablation catheters were used in 143 cases: 72 irrigated, 67 8-mm, and other types of catheters in the remainder.
Focal Atrial TachycardiaThere were 378 FAT ablation procedures in 68 centers (mean, 5 [4] procedures per center), and the overall success rate was 84.9%. In 67 of the 68 centers, ablation was for FAT affecting the right atrium,whereas only 28 centers treated FAT affecting the left atrium. All centers reported the origin of FAT. Right atrial tachycardia was more common, and the success rate of these procedures was slightly higher than that of left atrial procedures: 86.6% (252/291) for the right atrium vs 79.2% (65/82) for the left atrium. Ten complications (2.6%) were notified: 5 vascular complications, 4 pericardial effusions, and 1 transient ST elevation, likely due to a gas embolism.
The upward trend in the use of special catheters for FAT ablation has continued: 119 in 2011, 156 in 2012, and 174 in 2013. These mainly included irrigated-tip catheters (n=167), with the remainder being cryoablation (n=5) and 8-mm-tip (n=2) catheters.
Macroreentrant Atrial Tachycardia/Atypical Atrial FlutterThis substrate was treated in 52 centers (65%) in a total of 305 procedures (mean, 5.87 procedures per center; range, 1–20), 78 more than in 2012. Success was documented in 240 procedures (78%). Five complications (1.7%) occurred: 2 femoral complications, 2 cases of cardiac tamponade, and 1 atrioventricular block.
The origin of tachycardia was notified in 292 procedures: the right atrium was identified in 147 cases and the left atrium in 145, with success rates of 84.3% and 60.0%, respectively. In 96.3% of cases, devices other than conventional 4-mm-tip catheters were used, mainly irrigated tip catheters (90.1%), and the remainder (9.9%) used 8-mm tip catheters.
Atrial FibrillationIn total, 2201 AF ablation procedures were carried out in 52 (65%) centers (range, 1–126). This activity represents an 18.8% increase with respect to the 2012 registry (which showed a 21% increase relative to 2011), with a mean of 42.3 procedures per center. Six catheterization laboratories performed less than 10 procedures, and 16 less than 25. Sixteen centers carried out more than 50, and in this group, 7 had more than 100 procedures. Among the total, 56.4% (1242 procedures) were for paroxysmal AF and 43.2% (952) were for persistent AF. Four centers reported 7 procedures for permanent AF. Among ablations for persistent AF, 77 were for long-standing cases.
The treatment approach used was reported in 2186 (99.3%) procedures: electrical disconnection at the pulmonary vein ostium in 19.3% of cases, circumferential isolation with the aim of disconnection in 76.5%, and circumferential isolation to reduce electrical connections in the remaining 1.3%. The right atrium was treated in 7 procedures.
Most teams used irrigated-tip catheters (74.5%). In this registry, the percentage of cryoballoon ablations has held steady at 20.8% (n=458), whereas a clear increase was recorded in the last few years. Although the number of procedures rose from 350 to 458, the parallel increase in the total number of AF ablations performed in 2013 resulted in a similar percentage. An 8-mm-tip ablation catheter was used in only 3 procedures. There was an increase in the use of steerable sheaths, implemented in only 9 centers and employed in 457 procedures (20.7% of the total vs 150 procedures [8.0%] in the 2012 registry).
There were 107complications (4.8%, identical to the 2012 percentage): significant pericardial effusion/cardiac tamponade (n=47), vascular access (n=24), stroke (n=8), phrenic nerve palsy (n=7), and pulmonary vein stenosis (n=5). One death occurred (0.4‰), resulting from an atrioesophageal fistula complicated by endocarditis. In addition, there were 7 cases of pericarditis, 1 gastroparesia, 1 anesthesia-related anaphylactic shock, and 6 myocardial infarctions.
Idiopathic Ventricular TachycardiaIdiopathic ventricular tachycardia ablation was carried out in 359 procedures in 61 centers (mean, 5.8 procedures per center; range, 1–32). In total, 323 procedures were successful (89.9%), and there were 13 complications (3.6%): 11 cases of cardiac tamponade, 1 vascular complication, and 1 perioperative stroke; there were no cases of atrioventricular block or myocardial infarction.
The type of ventricular tachycardia treated was described in all 359 procedures: right ventricular outflow tract in 210; left ventricular outflow tract in 77; fascicular tachycardia in 33, and tachycardias other than the above (notified as other locations) in 39 procedures. Ablation was successful in 97.1%, 75.3%, 81.8%, and 58.9%of these procedures, respectively. The focal site of origin of the condition was the aortic root in 30 cases, the pulmonary artery in 17, and within a coronary vein in 3 cases. The catheters used were a 4-mm-tip type in 27.3% of cases, irrigated tip in 71.9%, and an 8-mm-tip or cryoablation catheter in 0.4% each.
Ventricular Tachycardia in Ischemic CardiomyopathyVentricular tachycardia in ischemic cardiomyopathy was treated in 54 (67.5%) centers by 394 ablation procedures (7.3 per center; range, 1–28). The following complications (n=29; 7.3%) were notified: vascular access (n=7), cardiac tamponade (n=14), stroke (n=1), heart failure (n=4), and complete atrioventricular block (n=2). Two patients (0.5%) died, 1 due to heart failure and the other due to heart failure and asystolia at 3 weeks.
The type of ablation performed was specified in 92.3% of cases (the access route was described as “endo/epi”, without clarification in 19 cases): a “conventional” approach was used in 91 cases and a substrate approach in 273. An irrigated-tip ablation catheter was used in most VT-ICM cases (96.2%). Steerable tips were employed in 91 cases. The success rate was 90.8% overall, 84.6% with the conventional approach, and 91.2% with the substrate approach. The number of procedures using an epicardial approach has held steady since the last Report, accounting for 11.8% (46 procedures) in the present registry, performed in a total of 18 centers.
Ventricular Tachycardia in Nonischemic CardiomyopathyA total of 205 VT-NICM ablation procedures were performed in 39 laboratories (48.7%) (5.26 procedures per center; range 1–20). These included 40 ablations forarrhythmogenic cardiomyopathy (success, 85%), 13 for branch-to-branchtachycardia (success, 77%), 69 for nonischemic dilated cardiomyopathy (success, 69.5%), 34 for nonsustained ventricular tachycardia (success, 79.4%), and 35 for conditions notified as another type (success, 62.9%). Five were epicardial procedures performed in only 2 centers; success was not specified.
There were 9 complications (4.3%): 3 vascular access-related, 3 cases of cardiac tamponade, and 3 heart failures, 1 leading to death (0.5%).
An irrigated-tip catheter was used in 98% of procedures and a 4-mm-tip catheter in all the remaining cases except 2: 1 procedure used a cryoablation catheter and the other a Lynx® catheter.
DISCUSSIONThe number of participating centers in the Spanish Catheter Ablation registry showed a further rise in 2013, making the Registry increasingly more representative of the situation regarding ablation procedures in our setting. In 2012, there were 74 participants, the largest number up to that time, whereas 80 centers submitted data to the current registry. The mean number of ablation procedures per site was greater than in the previous registry and the total number of procedures surpassed by far the 2012 value.
A slight decrease was documented in the healthcare professionals performing this activity. There was a small rise in the number of physicians dedicated to electrophysiology, but a decline was seen in those working fulltime. The number of residents, nursing graduates, and radiologic technologists has dropped since 2012. Laboratories exclusively used for electrophysiology were mainly operating in public healthcare centers.
The percentage of sites equipped with a nonfluoroscopic navigation system decreased slightly to below 80%. The availability of magnetic navigation and robotic navigation systems decreased by 1 center each.
As in previous years, there was an overall rise in the number of ablation procedures performed. However, there was a change in the relative percentages of the various substrates treated. The number of AF ablations significantly increased, and this substrate now ranks as the third most often treated (ahead of AP), in contrast to the 2012 data. Macroreentrant atrial tachycardia was the substrate showing the greatest percent rise. Of note, there was a slightly smaller percent increase in AF ablation procedures relative to last year. The number of centers performing > 50 AF procedures held steady. The complication rate associated with AF ablation decreased in 2013, as was the case for the other substrates.
The number of ablations for ventricular tachycardia in general was higher than in the previous registry, and this substrate showed the second greatest rise after macroreentrant atrial tachycardia. The number of procedures for idiopathic ventricular tachycardia remained stable and there was a notable increase in the procedural success rate, likely because of greater navigator use. There was a clear rise in the percentage of VT-ICM ablations relative to 2012, during which time a 3% reduction was documented. The substrate approach remains that most commonly used for this condition, at a 3:1 ratio with the conventional approach. As in the case of idiopathic ventricular tachycardia, the success rate for VT-ICM was significantly higher than in the previous year. There was, however, no significant increase in successful outcomes with the epicardial approach, which remained stable.
Atrial fibrillation ablations continued to increase, but at a percentage slightly lower than in 2012. Procedures using point-by-point radiofrequency ablation remained stable and those performed with a cryoballoon slightly increased. The year 2013 has witnessed the introduction of new approaches involving single-shot devices such as PVAC (Pulmonary Vein Ablation Catheter) and the use of new energies such as laser, although in very small numbers
CONCLUSIONSOnce again, the 2013 Spanish Catheter Ablation Registry contains one of the largest samples of ablation procedures reported in the related literature, reaching nearly 12 000 procedures. Increasingly more complex arrhythmic substrates were treated, while the success rates remained high and the percentages of major complications and deaths were low.
Nonetheless, as in previous years, the patent increase in the number and complexity of procedures performed in 2013 was not accompanied by a parallel increase in the number of healthcare professionals dedicated to this activity.
CONFLICTS OF INTERESTNone declared.
The coordinators would like to thank all the centers that voluntarily and disinterestedly submitted their data to the 2013 Spanish Catheter Ablation Registry. We extend special thanks to Cristina Plaza for her excellent and untiring administrative work.
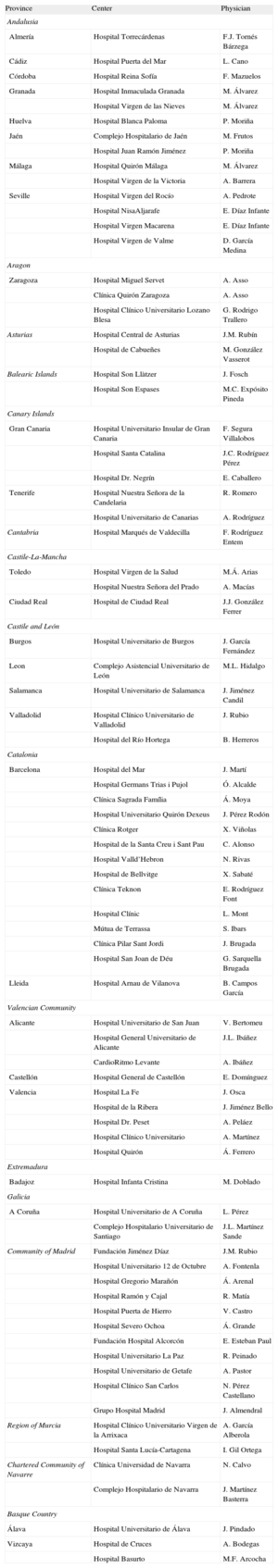
Francisco José Tornés, Lucas Cano, Francisco Mazuelos, Miguel Álvarez, Pablo Moriña, Manuel Frutos, Alberto Barrera, Alonso Pedrote, Ernesto Díaz-Infante, Dolores García-Medina, Antonio Asso, Gonzalo Rodrigo-Trallero, José Manuel Rubín, Mar González-Vasserot, Javier Fosch, María Carmen Expósito, Federico Segura-Villalobos, Juan Carlos Rodríguez-Pérez, Eduardo Caballero, Rafael Romero, Aníbal Rodríguez, Felipe Rodríguez-Entem, Miguel Á. Arias, Alfonso Macías, Juan José González-Ferrer, Javier García-Fernández, María Luisa Hidalgo, Javier Jiménez-Candil, Jerónimo Rubio, Benito Herreros, Julio Martí, Oscar Alcalde, Ángel Moya, Jordi Pérez-Rodón, Xavier Viñolas, Concepción Alonso, Nuria Rivas, Xavier Sabaté, Lluis Mont, Enrique Rodríguez-Font, Sonia Ibars, Josep Brugada, Georgia Sarquella-Brugada, Bieito Campos, Vicente Bertomeu, José Luis Ibáñez, Alicia Ibáñez, Eloy Domínguez, Joaquín Osca, Javier Jiménez-Bello, Antonio Peláez, Ángel Martínez, Ángel Ferrero, Manuel Doblado, Luisa Pérez, José Luis Martínez-Sande, José Manuel Rubio, Adolfo Fontenla, Ángel Arenal, Roberto Matía, Víctor Castro, Ángel Grande, Elena Esteban-Paul, Rafael Peinado, Agustín Pastor, Nicasio Pérez-Castellano, Jesús Almendral, Arcadio García-Alberola, Ignacio Gil-Ortega, Naiara Calvo, Javier Martínez-Basterra, Javier Pindado, Andrés Bodegas, and M. Fe Arcocha.
| Province | Center | Physician |
| Andalusia | ||
| Almería | Hospital Torrecárdenas | F.J. Tornés Bárzega |
| Cádiz | Hospital Puerta del Mar | L. Cano |
| Córdoba | Hospital Reina Sofía | F. Mazuelos |
| Granada | Hospital Inmaculada Granada | M. Álvarez |
| Hospital Virgen de las Nieves | M. Álvarez | |
| Huelva | Hospital Blanca Paloma | P. Moriña |
| Jaén | Complejo Hospitalario de Jaén | M. Frutos |
| Hospital Juan Ramón Jiménez | P. Moriña | |
| Málaga | Hospital Quirón Málaga | M. Álvarez |
| Hospital Virgen de la Victoria | A. Barrera | |
| Seville | Hospital Virgen del Rocío | A. Pedrote |
| Hospital NisaAljarafe | E. Díaz Infante | |
| Hospital Virgen Macarena | E. Díaz Infante | |
| Hospital Virgen de Valme | D. García Medina | |
| Aragon | ||
| Zaragoza | Hospital Miguel Servet | A. Asso |
| Clínica Quirón Zaragoza | A. Asso | |
| Hospital Clínico Universitario Lozano Blesa | G. Rodrigo Trallero | |
| Asturias | Hospital Central de Asturias | J.M. Rubín |
| Hospital de Cabueñes | M. González Vasserot | |
| Balearic Islands | Hospital Son Llàtzer | J. Fosch |
| Hospital Son Espases | M.C. Expósito Pineda | |
| Canary Islands | ||
| Gran Canaria | Hospital Universitario Insular de Gran Canaria | F. Segura Villalobos |
| Hospital Santa Catalina | J.C. Rodríguez Pérez | |
| Hospital Dr. Negrín | E. Caballero | |
| Tenerife | Hospital Nuestra Señora de la Candelaria | R. Romero |
| Hospital Universitario de Canarias | A. Rodríguez | |
| Cantabria | Hospital Marqués de Valdecilla | F. Rodríguez Entem |
| Castile-La-Mancha | ||
| Toledo | Hospital Virgen de la Salud | M.Á. Arias |
| Hospital Nuestra Señora del Prado | A. Macías | |
| Ciudad Real | Hospital de Ciudad Real | J.J. González Ferrer |
| Castile and León | ||
| Burgos | Hospital Universitario de Burgos | J. García Fernández |
| Leon | Complejo Asistencial Universitario de León | M.L. Hidalgo |
| Salamanca | Hospital Universitario de Salamanca | J. Jiménez Candil |
| Valladolid | Hospital Clínico Universitario de Valladolid | J. Rubio |
| Hospital del Río Hortega | B. Herreros | |
| Catalonia | ||
| Barcelona | Hospital del Mar | J. Martí |
| Hospital Germans Trias i Pujol | Ó. Alcalde | |
| Clínica Sagrada Família | Á. Moya | |
| Hospital Universitario Quirón Dexeus | J. Pérez Rodón | |
| Clínica Rotger | X. Viñolas | |
| Hospital de la Santa Creu i Sant Pau | C. Alonso | |
| Hospital Valld’Hebron | N. Rivas | |
| Hospital de Bellvitge | X. Sabaté | |
| Clínica Teknon | E. Rodríguez Font | |
| Hospital Clínic | L. Mont | |
| Mútua de Terrassa | S. Ibars | |
| Clínica Pilar Sant Jordi | J. Brugada | |
| Hospital San Joan de Déu | G. Sarquella Brugada | |
| Lleida | Hospital Arnau de Vilanova | B. Campos García |
| Valencian Community | ||
| Alicante | Hospital Universitario de San Juan | V. Bertomeu |
| Hospital General Universitario de Alicante | J.L. Ibáñez | |
| CardioRitmo Levante | A. Ibáñez | |
| Castellón | Hospital General de Castellón | E. Domínguez |
| Valencia | Hospital La Fe | J. Osca |
| Hospital de la Ribera | J. Jiménez Bello | |
| Hospital Dr. Peset | A. Peláez | |
| Hospital Clínico Universitario | A. Martínez | |
| Hospital Quirón | Á. Ferrero | |
| Extremadura | ||
| Badajoz | Hospital Infanta Cristina | M. Doblado |
| Galicia | ||
| A Coruña | Hospital Universitario de A Coruña | L. Pérez |
| Complejo Hospitalario Universitario de Santiago | J.L. Martínez Sande | |
| Community of Madrid | Fundación Jiménez Díaz | J.M. Rubio |
| Hospital Universitario 12 de Octubre | A. Fontenla | |
| Hospital Gregorio Marañón | Á. Arenal | |
| Hospital Ramón y Cajal | R. Matía | |
| Hospital Puerta de Hierro | V. Castro | |
| Hospital Severo Ochoa | Á. Grande | |
| Fundación Hospital Alcorcón | E. Esteban Paul | |
| Hospital Universitario La Paz | R. Peinado | |
| Hospital Universitario de Getafe | A. Pastor | |
| Hospital Clínico San Carlos | N. Pérez Castellano | |
| Grupo Hospital Madrid | J. Almendral | |
| Region of Murcia | Hospital Clínico Universitario Virgen de la Arrixaca | A. García Alberola |
| Hospital Santa Lucía-Cartagena | I. Gil Ortega | |
| Chartered Community of Navarre | Clínica Universidad de Navarra | N. Calvo |
| Complejo Hospitalario de Navarra | J. Martínez Basterra | |
| Basque Country | ||
| Álava | Hospital Universitario de Álava | J. Pindado |
| Vizcaya | Hospital de Cruces | A. Bodegas |
| Hospital Basurto | M.F. Arcocha | |