To the Editor:
Inadequate stent expansion during implantation can be interpreted as an in-stent lesion during conventional angiography. This phenomenon is a lesser known mechanism than intimal proliferation, and is known as stent pseudorestenosis. Highly sensitive techniques, such as intravascular ultrasound,1 are needed for the differential diagnosis between these entities, because of the implications for treatment. Nonoptimal stent apposition in the vessel wall has been related to revascularization complexity in some situations,2-4 and has been considered a factor associated with the subsequent development of events, such as stent thrombosis.5,6 Resolution of false restenosis may require the use of various revascularization techniques to increase stent expansion, sometimes with considerable difficulties and not always successfully.
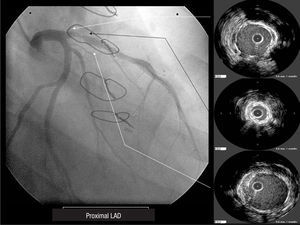
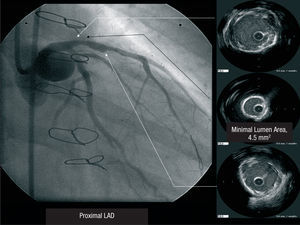
A 45-year-old woman, ex-smoker as the single risk factor, went to another hospital for acute anterior myocardial infarction that was treated with systemic fibrinolysis. Since this failed, salvage angioplasty was performed. The right coronary and circumflex arteries showed no lesions, but a critical lesion was detected in the proximal left anterior descending artery (LAD), which was treated with implantation of a bare metal stent. At 2 months she was readmitted for unstable angina and electrocardiographic evidence of transient ST-segment elevation in the anterior territory in one of the crises. During hospitalization, the patient presented numerous angina attacks at rest with little therapeutic response. Repeat angiography showed a significant in-stent lesion that was interpreted as early stenosis. Surgical revascularization with a left mammary artery graft to the LAD was performed. At 4 months the patient again presented numerous angina attacks with no electrocardiographic changes and poor therapeutic response to the usual antianginal therapy. At that time she was referred to our center. Coronary angiography showed mammary graft occlusion and a critical lesion in the stent implanted in the proximal LAD. Intravascular ultrasound of the LAD lesion showed a lumen area of 2.5 mm2 and a circumferential annular calcification that prevented stent expansion, with no intimal proliferation (Figure 1). Numerous attempts to break the annular calcification and expand the stent with various high-pressure balloons of different diameters and cutting balloons were unsuccessful. The angina symptoms persisted; hence, a second procedure was undertaken. Because the revascularization options were limited, rotational atherectomy in the lesion area was chosen. Following an unsuccessful initial attempt with a 2-mm burr, stent ablation was finally achieved with a 2.25-mm burr. After multiple dilations with high-pressure balloons, the results were reassessed with intravascular ultrasound, which showed rupture of the calcium plaque in the lesion and a final lumen area of 4.5 mm2 (Figure 2). Because few options were available for revascularization and the procedure was difficult, the outcome was considered at the limits of acceptability. The cause of mammary artery graft occlusion was not determined. Various procedures showed TIMI 3 coronary flow, but no signs of embolization.
Figure 1. Baseline proximal left anterior descending artery. DA proximal = Proximal LAD
Figure 2. Post-atherectomy proximal left anterior descending artery.