To the Editor:
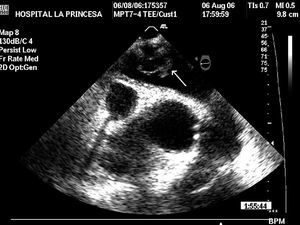
We describe a 65-year-old woman with no relevant history admitted for major depression. During hospitalization, she experienced a traumatic head injury and underwent cranial computed tomography, which revealed a small subarachnoid hemorrhage. She presented cardiorespiratory arrest the following day, but recovered successfully. The patient also presented considerable hemodynamic instability; transesophageal echocardiography showed dilatation, and hypokinesia of the right ventricle (RV), with a thrombus in the pulmonary artery (Figure 1). Based on a diagnosis of massive acute pulmonary thromboembolism (PTE), fibrinolysis for the cerebral hemorrhage was not performed and the patient was scheduled for emergency surgery.
Figure 1. Thrombus in the pulmonary artery trunk (arrow). 0o cross-sectional view of the aortic root and pulmonary artery.
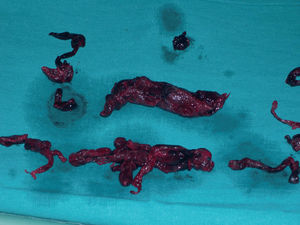
During anesthesia induction, cardiac arrest occurred again, requiring an emergency sternotomy. Longitudinal arteriotomy of the trunk was performed and large thrombi were removed from the pulmonary artery trunk and both pulmonary arteries (Figure 2). The patient required circulatory assistance for 330 min. She left the operating theater on high-dose vasoactive and inotropic drugs, although the sternotomy was not closed because of extensive RV dilation.
Figure 2. Thrombi removed from the pulmonary artery trunk and both pulmonary arteries.
In the intensive care unit (ICU), the patient improved hemodynamically, and the sternotomy was closed on the third day. Sodium heparin therapy was started and she was extubated on day 10 and discharged after 1 month with no sequelae.
Fibrinolysis is the treatment of choice in acute PTE,1 although an increasing number of cases are treated by surgery. Gulba et al2 found a similar mortality between the medically treated group and the surgical group, but with a lower incidence of recurrence in the latter (21% vs 7.7%). Meneveau et al3 pointed out that surgery provides greater benefits in patients with acute PTE who do not respond to thrombolytics. Leacche et al4 described 47 patients and mortality of 6% in a series in which only 32% of patients presented RV dysfunction and only 11% had presented cardiac arrest. At present, preoperative cardiac arrest, which occurs rather often during anesthesia induction,5 is considered to be the greatest indicator of surgical mortality.4
Early diagnosis is needed to prevent irreversible damage, since 70% of patients with acute PTE die within the first hour.6 Echocardiography currently allows rapid, efficient diagnosis of PTE.7
Surgery may be prolonged due to the need for RV assist. In our patient, although the thrombus was removed within 20 min, 5 hours of assist were needed for the RV to recover slightly. Sadeghi et al8 has advocated the use of RV assist if necessary.
The use of a vena cava filter is controversial. When anticoagulant therapy is given, recurrence after embolectomy is below 5%.9 The use of a filter is currently indicated in patients with PTE and a contraindication for anticoagulation and in patients with PTE despite anticoagulation therapy.10 Our patient began sodium heparin therapy on postoperative day 3, with oral anticoagulants prescribed for 6 months. Doppler echocardiography of the lower limbs as well as hypercoagulability and tumor marker testing were all negative. On this basis, a filter was not implanted in the inferior vena cava and it was decided to follow the patient's progress in the outpatient clinic.
In conclusion, emergency embolectomy was done successfully in a patient with a massive PTE who had experienced 2 previous cardiac arrests. Early diagnosis followed by early intervention is essential in patients with massive PTE who are not eligible for fibrinolysis.