To the Editor:
Of pacemaker malfunctions,1 runaway pacemaker events are infrequent electronic complications that present at any time in the life of the pacemaker.2-4 Described between 2 days and 9 years after implantation, they are life-threatening emergencies that can go undetected if they appear intermittently.5,6
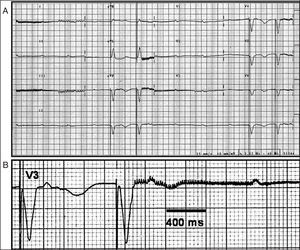
Recently, we attended a 96 year-old woman with a VVIR Medtronic Minix-ST pacemaker implanted in 1995 for symptomatic complete atrioventricular block. She was admitted to our coronary unit with dizziness and progressive dyspnea with blood pressure 130/60 mm Hg and bilateral crepitations in posterior plane. The electrocardiogram showed irregular pacemaker rhythm with 2 consecutive spikes generated at an interval of 960 ms, the second of which was followed by high frequency electric "interference" (3000 Hz). This interference initially accelerated and then decelerated until disappearing and we later registered normal, single pacemaker spikes at 4120 ms intervals (Figure A and B). The high frequency minispikes did not constitute artifacts as they were recorded systematically. Chest x-ray showed a pattern of acute pulmonary edema. The pacemaker problem persisted despite magnetic inhibition of the generator and use of a transitory stimulation electrode. The patient, treated with high dose inotropics and diuretics, finally died of multiorgan failure.
Figure. A: 12-lead electrocardiogram showing irregular pacemaker stimulation alternating 960 ms and 4120 ms cycles. After the impulse that defines the shortest cycle, high frequency (3000 Hz), low amplitude spikes which are not captured by the ventricle, are recorded over 3080 ms. B: electrocardiogram (V3-lead) showing high frequency spikes that initially accelerate and later decelerate until finally disappearing.
In the 60s, incidence of this complication was 2%-4% with 30%-40% mortality.4 It presents in 2 forms: a) pacemaker-induced ventricular tachycardia; and b) extreme bradycardia due to impaired ventricular capture of rapid low amplitude sub-threshold pulses. Although bradycardia is better tolerated than tachycardia, mortality of both presentations does not differ significantly.3-5 Runaway pacemaker events should be considered when pacemaker stimulation frequency is above the established upper limit, excluding the possibility of pacemaker-mediated tachycardia.
Runaway pacemaker events have been attributed to various causes: a) primary circuit failure; b) defects in the generator's hermetic seal; c) circuit damage caused by the electric scalpel or radio-frequency ablation; and d) sterilization of the generator with heat.7 Recently, a runaway event in a patient implanted with a defibrillator was reported.8
The runaway phenomenon is refractory to defibrillation and antiarrhythmic agents as the problem is intrinsic to the pacemaker. Reprogramming the generator and over-stimulation with a transitory electrode have been used with poor results. The use of a magnet to inhibit the pacemaker may be inefficient as this only disables the pacemaker's sensing function. Consequently, the only efficient treatment may be disconnecting the generator electrodes by cutting leads or reprogramming the system.9
Runaway pacemaker events are a potentially lethal malfunction and in Spain they may be more frequent than thought as little is known of them and they often present intermittently.