Mitral regurgitation (MR) is one of the major valvular diseases. Surgical mitral valve (MV) repair is the standard of care for patients with severe degenerative MR due to prolapse or flail of a valve leaflet. Surgical MV repair is performed combining ring annuloplasty with leaflet and chordal repair as necessary.
Within the growing era of percutaneous treatments for valvular heart disease, the echo-guided NeoChord MV repair procedure (NeoChord, Inc, St Louis Park, MN, USA) has demonstrated early safety and efficacy outcomes in a selected group of patients with posterior MV prolapse/flail not requiring an adjunctive annuloplasty.1
Recent analyses have provided more insights into patient selection for the NeoChord procedure, finding precise morphological and echocardiographic criteria.1,2 In particular, the leaflet-to-annulus index (LAI), which precisely defines those patients who do not have a leaflet-to-annulus mismatch and who for this reason could benefit of an isolated leaflet therapy without concomitant annuloplasty.
The LAI is defined as the ratio between the sum of anterior mitral leaflet length (AML) and posterior mitral leaflet length (PML) over the anteroposterior diameter (AP) of the MV annulus (AP; AML+PML/AP). The LAI was a positive postoperative predictor of MR ≤ mild at 1-year of follow-up once it was superior to 1.2.2
Moreover, the estimated coaptation length (CL) index has been recently introduced as an additional tool to estimate the potential postoperative leaflet CL.3 The CL index is defined according to the following formula: [(AML+PML)-AP]/2]. Postoperative CL is a predictive factor for durable MV repair when it is longer than 6mm.4
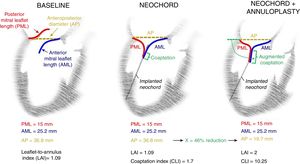
On the basis of these assumptions, we proposed to use the combination of the validated LAI and CL index formulas to discriminate between patients who benefit from a ringless NeoChord procedure alone because the predicted final CL will be adequate to gain an effective and durable result and those who require an adjunctive annular therapy to reduce the AP diameter, resulting in an improvement of the CL (figure 1).
Schematic representation of a treated patient showing the heart in an echocardiographic long-axis view, after only leaflet treatment with NeoChord implantation and after combination of NeoChord and direct annuloplasty procedures. AML, anterior mitral leaflet length; AP, anteroposterior diameter; CLI, coaptation index; LAI, leaflet-to-annulus index; PML, posterior mitral leaflet.
Transcatheter annuloplasty procedures have also been demonstrated to be safe and effective in reducing AP annulus diameter. Transcatheter annuloplasty can be performed with devices acting directly or indirectly on the MV annulus.
Indirect annuloplasty through the coronary sinus (Carillon Mitral contour system, Cardiac Dimensions, Kirkland, USA) is recommended when the preoperative computed tomography scan shows a correct alignment and closed continuity between the coronary sinus and the MV annulus.
Direct annuloplasty can be performed using the Cardioband system (Edwards Lifesciences, Irvine, CA, USA). It is advisable not to have annular calcifications and proximity of the circumflex artery. Both devices can achieve an AP diameter reduction of 20% to 45%.5
Six patients considered not suitable for conventional MV repair based on their specific characteristics by the local Heart Team (table 1) were treated with single-stage transcatheter annular and leaflet therapies. All patients had an advanced-stage degenerative MV pathology with the presence of leaflet flail and concomitant annular dilatation. All patients underwent leaflet treatment with NeoChord implantation with a mean number of 3 chordae and concomitant annuloplasty procedure implanting the Cardioband device in 2 patients (, transesophageal echocardiogram showing baseline condition, implantation of the Cardioband followed by implantation of the NeoChord with maximum cinching of the annuloplasty device), and the Carillon in 4 patients (, transesophageal echocardiogram showing baseline condition, implantation of the Carillon followed by implantation of NeoChord). In a single NeoChord plus Cardioband case, a commissural MitraClip (Abbott, Menlo Park, CL, USA) was also implanted at the end of the procedure to treat a residual mild MR due to a commissural prolapse. This resulted in trace MR as the final outcome. The decision process for selecting the annuloplasty device was tailored based on the integration of the patient's anatomical and echocardiographic data (MV annulus and leaflet measurements, presence/absence of annular calcifications, location of the coronary sinus, and circumflex artery).
Preoperative and postoperative characteristics of the patients treated with COMBO mitral valve repair procedures
| Patient number | 1 | 2 | 3 | 4 | 5 | 6 |
|---|---|---|---|---|---|---|
| PROCEDURES | Carillon+NeoChord | Carillon+NeoChord | Carillon+NeoChord | Carillon+NeoChord | Cardioband+Neochord+Mitraclip | Cardioband+NeoChord |
| Baseline Characteristics | ||||||
|---|---|---|---|---|---|---|
| Sex, male | 1 | 1 | 1 | 1 | 1 | 1 |
| Age | 75 | 82 | 78 | 73 | 70 | 60 |
| STS score valve repair | ||||||
| Mortality, % | 1.27 | 2.65 | 1.86 | 6.10 | 0.80 | 1.59 |
| Morbidity, % | 13.81 | 20.68 | 18.28 | 38.19 | 9.99 | 14.83 |
| Comorbidities | ||||||
| CAD | 2 VD | 0 | 3 VD | 1 VD | 0 | 3 VD |
| Previous MI | 0 | 0 | 0 | 1 | 0 | 1 |
| Previous PCI | 1 | 0 | 0 | 1 | 0 | 1 |
| Previous heart surgery | 0 | 0 | CABG+AVR | 0 | 0 | CABG |
| Previous TAVI | 0 | 0 | 0 | 0 | 0 | 0 |
| Systolic pulmonary artery pressure, mmHg | 45 | 50 | 40 | 30 | 30 | 50 |
| COPD | 0 | 0 | 0 | 0 | 0 | 0 |
| AF | 1 | 0 | 1 | 1 | 0 | 0 |
| Past CVA | 0 | 0 | 1 | 0 | 0 | 0 |
| Chronic renal failure (GFR <60mL/min) | 52 | 50 | 66 | 28 | 61 | 95 |
| NYHA | ||||||
| II | 0 | 0 | 0 | 0 | 0 | 0 |
| III | 1 | 1 | 1 | 1 | 1 | 1 |
| IV | 0 | 0 | 0 | 0 | 0 | 0 |
| Hospital admission for HF (number of times before admission for treatment) | 0 | 1 | 1 | 1 | 0 | 2 |
| LVEF | 50 | 50 | 60 | 20 | 65 | 30 |
| Preoperative Echocardiography | ||||||
|---|---|---|---|---|---|---|
| IC, mm | 48.3 | 41.7 | 45.4 | 44.0 | 48.0 | 45.7 |
| AP, mm | 38.8 | 38.4 | 35.1 | 35.3 | 38.6 | 36.8 |
| AML, mm | 23.0 | 24.0 | 22.9 | 18.0 | 19.0 | 25.2 |
| PML, mm | 16.3 | 20.3 | 9.3 | 10.0 | 21.0 | 15.0 |
| EROA, cm2 | 0.6 | 0.5 | 0.6 | 0.7 | 0.7 | 0.7 |
| R Vol, mL | 85.4 | 69.4 | 88.5 | 125.0 | 88.2 | 58.0 |
| LAI | 1.0 | 1.15 | 0.91 | 0.8 | 1.03 | 1.09 |
| CI, mm | 0.25 | 2.95 | −1.45 | −7 | 0.7 | 1.7 |
| Postoperative Echocardiography | ||||||
|---|---|---|---|---|---|---|
| IC, mm | 30.9 | 31.3 | 33.2 | 25.7 | 34.3 | 19.3 |
| AP, mm | 28.1 | 23.9 | 25.7 | 25.3 | 27.1 | 19.7 |
| EROA, cm2 | 0.04 | 0.08 | 0.01 | 0.04 | 0.01 | 0.02 |
| R Vol, mL | 6.3 | 10.3 | 1.6 | 8.3 | 1.6 | 2.1 |
| LAI | 1.4 | 1.8 | 1.25 | 1.1 | 1.5 | 2.0 |
| CI, mm | 5.65 | 10.1 | 3.25 | 2.7 | 6.5 | 10.25 |
| IC postoperative reduction, % | 36 | 25 | 27 | 42 | 28 | 58 |
| AP postoperative reduction, % | 28 | 38 | 28 | 31 | 30 | 46 |
AF, atrial fibrillation; AML, anterior mitral leaflet length; AP, anteroposterior mitral annulus diameter; AVR, aortic valve replacement; CABG, coronary artery bypass graft; CAD, coronary artery disease; COPD, chronic obstructive pulmonary disease; CVA, cerebrovascular accident; CI, coaptation length Index; EROA, effective regurgitant orifice area; GFR, glomerular filtration rate; HF, Heart Failure; IC, intercommissural diameter; LVEF, left ventricle ejection fraction; LAI, leaflet-to-annulus index; MI, myocardial infarction; NYHA, New York heart Association; PCI, percutaneous coronary intervention; PML, posterior mitral leaflet length; R vol, regurgitant volume; TAVI, transcatheter aortic valve implantation; VD, vessel disease.
In all patients, we implanted the annuloplasty device first, observing an immediate reduction in the MR but with persistent leaflet flail requiring additional leaflet therapy to reduce its height and generating stable coaptation. All procedures were successful with minimal residual MR (table 1). All patients showed an echocardiographically effective AP reduction with consequent postoperative increase in the LAI and CL index. All patients achieved the 30-day follow-up with residual MR <mild and New York Heart Association class I.
This article describes the initial clinical experience of the application of a new single-stage combined transcatheter approach to treat patients presenting advanced-stage degenerative MV disease with the concomitant combination of transcatheter annular and leaflet therapies. This surgical-like transcatheter MV repair was safe, feasible, and effective in treating a specific subset of highly selected patients. It is important to highlight that the decision-making algorithm derives from the knowledge acquired in the field of surgical MV repair over the last 50 years of practice after demonstration that those concepts provided excellent results. The present toolbox concept of transcatheter MV devices to treat MV leaflet and annulus represents the contemporary evolution of the wide variety of surgical techniques described and used by surgeons to perform MV repair. Future clinical studies will be required to further validate this surgical-like single stage transcatheter MV repair COMBO approach.
DisclosuresA. Colli, A Beiras-Fernandez, von Berdeleben S, received travel grants from NeoChord, Inc. A. Beiras-Fernandez is proctor for NeoChord, Inc. S. von Bardeleben received travel grants from NeoChord Inc, Edwards Lifesciences, Carillon Contour system and Cardiac Dimensions.
Conflicts of interestA. Colli received travel grants from NeoChord, Inc. A. Beiras-Fernández was a proctor for NeoChord, Inc. S. von Bardeleben received travel grants from NeoChord, Inc, Edwards Lifesciences and Cardiac Dimensions.
The other authors have nothing to disclose.
Supplementary data associated with this article can be found in the online version, at https://doi.org/10.1016/j.rec.2019.04.003.