In the present article, we review publications from the previous year in the following 3 areas: clinical cardiology, geriatric cardiology, and heart failure and transplantation. Among the new developments in clinical cardiology are several contributions from Spanish groups on tricuspid and aortic regurgitation, developments in atrial fibrillation, syncope, and the clinical characteristics of heart disease, as well as various studies on familial heart disease and chronic ischemic heart disease. In geriatric cardiology, the most relevant studies published in 2014 involve heart failure, degenerative aortic stenosis, and data on atrial fibrillation in the geriatric population. In heart failure and transplantation, the most noteworthy developments concern the importance of multidisciplinary units and patients with preserved systolic function. Other notable publications were those related to iron deficiency, new drugs, and new devices and biomarkers. Finally, we review studies on acute heart failure and transplantation, such as inotropic drugs and ventricular assist devices.
Keywords
Surgical repair results were described in a study of 119 patients with tricuspid regurgitation; the cause was organic in 40%. Most lesions were repaired using de Vega annuloplasty (73%). The mortality and complication results were satisfactory, and age and cardiopulmonary bypass time persistently appeared as predictive factors of death and residual tricuspid regurgitation. As in other series, this study suggested that the indications are restrictive and limited to those patients with more advanced or organic valvular disease. Consequently, there are relatively few cases for the wide period considered; on average, an intervention was performed on tricuspid regurgitation in only 6.4% of the 133 valvular disease patients treated annually. Moreover, the high proportion of patients with organic valvular disease or previous surgery increased the risk of the intervention.1
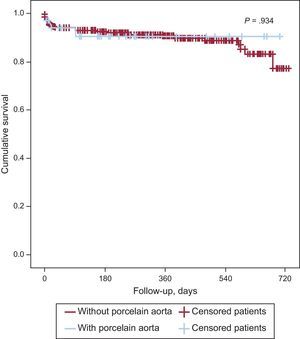
Various studies on percutaneous aortic valve implants have been published during the year. One particularly notable article reported the results of percutaneous aortic valve implantation in patients with porcelain aorta.2 This study presented short- and long-term results after percutaneous aortic valve implantation with the Medtronic CoreValve® System in patients with porcelain aorta. A total of 449 patients were included from 3 academic centers. The prevalence of porcelain aorta was 8%. Bearing in mind the lack of uniformity in the definitions used, atherosclerosis of the aorta was found in up to one-third of octogenarians who underwent cardiac surgery interventions, and the frequency of true porcelain aorta was between 1% and 5% (Figure).
In one of the largest series published, Forteza et al3 presented the results of valve-sparing surgery in 51 patients with bicuspid aortic valve and aneurysm of the aortic root or ascending aorta. Valves with calcification in both cusps or with retraction, tissue loss, or perforations were not considered candidates for repair. At the end of follow-up, no patients had died and all patients were free of aortic regurgitation > II and reintervention on the aortic valve. Thus, this surgical technique is an option in selected patients with bicuspid aortic valve and shows excellent medium-term results.3
Atrial FibrillationAtrial fibrillation and its consequences is one of the most prevalent conditions in clinical cardiology, affecting up to 21% of patients attending cardiology clinics. This anomaly was studied in several important articles published in 2014. The FIATE study,4 a cross-sectional, multicenter study of patients attending Spanish health centers, included 2070 patients with a mean age of 74 years (50.7% women) with atrial fibrillation routinely attended in primary care. The therapeutic strategy in 4 out of 5 patients was based on heart rate control; the patients showed high use of oral anticoagulants (84%) and were mainly followed up in primary care (72%). Finally, the last 3 INR (international normalized ratio) readings of only 33% of patients were within the therapeutic range.4
Regarding the diagnosis of this heart condition, Sanmartín et al5 analyzed the possible benefits of an information campaign and atrial fibrillation diagnosis. In this program, individuals ≥ 65 years were invited by letter and through posters and leaflets to consult a specially trained nurse in 3 health centers and the specialized center of a tertiary referral hospital for 5 consecutive days. The selected population had no history of atrial fibrillation or flutter. The program included a brief medical history, blood pressure reading, and palpation of the radial or humeral pulse for at least 15seconds. If the nurse detected any pulse irregularity, an electrocardiogram was performed and immediately analyzed by a family physician. In 1532 participants with a mean (SD) age of 72.5 (6.5) years, there were 17 cases of newly diagnosed atrial fibrillation (1%). The authors concluded that, while the benefits of this type of campaign are difficult to estimate in terms of the health education provided, this approach detects few asymptomatic cases of atrial fibrillation in an at-risk Spanish population.5
During 2014, new data were published on the use of new direct oral anticoagulant drugs in the prevention of embolisms in patients with atrial fibrillation. The ENGAGE AF-TIMI 48 study6 showed how edoxaban, a new once-daily factor Xa inhibitor, has been successfully added to this group of drugs. This clinical trial included 21 105 patients followed up for 2.8 years and compared the 60mg and 30mg one-a-day edoxaban regimens. Edoxaban was noninferior to well-controlled warfarin in the prevention of stroke and systemic embolism. Compared with warfarin, edoxaban was associated with a more consistent dose-related reduction in bleeding, showing itself to be a new therapeutic option, effective and safer than standard warfarin therapy.6
For direct oral anticoagulant drugs already used in clinical practice, many studies have confirmed the results of the initial clinical trials, reaffirming the benefit and safety of their correct use in preventing stroke and peripheral embolisms in patients with nonvalvular atrial fibrillation. The use of direct oral anticoagulants is absolutely contraindicated in patients with mechanical aortic or mitral valve prostheses (in the 7 days before randomization or in the previous 3 months), as indicated by the results of the RE-ALIGN study.7 This phase II clinical trial examined the efficacy and safety of dabigatran in these 2 types of patients. After the inclusion of 252 patients, the trial was prematurely terminated due to an excess of embolic and bleeding events in the patients treated with dabigatran. Safety analysis showed that, dabigatran was associated with an increased risk of bleeding events. Analysis of the efficacy of dabigatran in the prevention of thromboembolic phenomena revealed a nonsignificant trend toward an increased risk of embolic events, defined as a composite of death, stroke, transient ischemic attack, systemic embolism, or myocardial infarction, which could be largely explained by the higher number of cerebrovascular events.7
SyncopeThe use of the implantable loop recorder has been expanded for the diagnosis of patients with syncope. One notable, prospective, multicenter Spanish registry included patients who received an implantable loop recorder from 2006 to 2008. There were 1-year follow-up data for 91% of participants. Of the 743 patients included (55.6% men; mean age, 64.9 years), 31% had heart disease and 24.6% had bundle branch block. The indication for implantation was syncope in 76.4% of patients. In a third of the patients, a final diagnosis was obtained with the implantable loop recorder, independent of the baseline characteristics. There were 414 events in 48% of the patients (325 patients) and a final diagnosis was obtained in 230 of them (70.8% of patients with events and 33.1% of patients with follow-up). The most frequent diagnosis was syncope secondary to bradyarrhythmia, without differences among patients with heart disease, bundle branch block, or normal heart. Patients with recurrent syncope as the indication for implantation had more events during follow-up.8
Clinical Characteristics of Patients With Heart DiseaseMejía-Lancheros et al9 published a subanalysis of the PREDIMED study, which included 7447 people with cardiovascular risk factors; the lower age limit was 55 years for men and 60 years for women. The study analyzed if socioeconomic differences, as gauged by educational level, determined the treatment prescribed for diabetes, hypertension, or dyslipidemia. Multivariate analysis failed to show differences between participants with moderate or low educational levels and the treatment received, suggesting that free universal health care effectively reduces possible treatment differences related to socioeconomic status.
Barrios et al10 analyzed the clinical profile and management of hypertensive patients seen in primary care according to age, taking data from the PRESCAP 2010 study. Of the 12 961 patients included, 440 (3.4%) were younger than 45 years, 1672 (12.9%) were 45 to 54 years of age, and 10 849 (83.7%) were older than 54 years. Systolic blood pressure increased as patients aged, along with the proportion of patients with dyslipidemia, diabetes mellitus, target organ damage, and cardiovascular disease. In contrast, increased patient age was accompanied by decreases in diastolic blood pressure and the proportion of patients who smoked and with family history of cardiovascular disease. Blood pressure control worsened as patient age increased (62.3%, 54.8%, and 44.0%, respectively; P = .0001), despite greater use of combination therapy (43.4%, 49.9%, and 66.4%; P = .0001). As patient age increased, physicians made fewer changes to the antihypertensive treatment in response to poor blood pressure control (36.3%, 35.1%, and 27.5%; P = .0001). The most frequent response in all patients was to add another drug, followed by a dose increase, and the least frequent approach was to modify the pharmacological treatment, without significant differences according to age.
Genetic and Familial Heart DiseasesSelection of notable studies in this field is difficult due to the enormous volume published and the important work performed by various Spanish groups in this area. Villacorta et al11 describe the case of a patient who had frozen embryos from in vitro fertilization who wanted only those free from mutation to be implanted. A genetic study showed that the patient had inherited 2 mutations in the same gene, 1 from each parent. Thus, all her descendents would have one or the other mutation. In their experience, almost half of patients, both carriers and noncarriers of the mutation, are in reproductive age and were advised on reproductive issues. In addition, the penetrance of hypertrophic cardiomyopathy is high. There are various legal limitations in certain professions (police, fire service, pilots, etc) and competitive athletics for patients who develop this disease. Thus, career and sporting counseling should be given to families with this genotype before professions are selected.
The second work12 was a cost-utility analysis of a genetic study of patients with hypertrophic cardiomyopathy in the units of the Son Llàtzer and Puerta de Hierro hospitals from 2008 to 2012. The authors calculated the costs of the genetic study and the costs of clinical visits and associated tests that could be saved by dispensing with follow-up in genotype-negative families. The overall expense was low, at just €135 per family who underwent the genetic study. In addition, latest-generation sequencing techniques that allow analysis of more genes at a lower cost are likely to further reduce the cost of the method and tip the scale toward a net economic saving. Of the sample, 24% were younger than 30 years and could be advised on their professional and sporting activities. Naturally, the benefit is also significant for families negative for the genotype. As well as the lack of need for lifelong follow-up, participants who learn that they are not carriers of the mutation are free to pursue any type of physical or professional activity and have no reproductive implications.
Chronic Coronary Artery DiseaseThe CLARIFY study13 involves an international registry with a planned follow-up of 5 years that is being performed in 41 countries in outpatients with stable coronary artery disease. During 2014, the baseline results of the CLARIFY study in Spain were published and compared with those of other Western European countries. Worldwide, 33 248 patients were included, 14 726 in western Europe and 2257 in Spain.13 In Spain, the mean age was 65 years, slightly lower than that of other western countries, and most participants were men (81%). Compared with the rest of western Europe, the Spanish cohort had a higher frequency of diabetes mellitus (34% vs 25%; P < .0001), myocardial infarction (64% vs 60%; P < .0001), and stroke (5% vs 3%; P = .0007) and a lower frequency of family history of coronary artery disease (19% vs 31%; P < .0001). The most common treatments in the Spanish sample were lipid-lowering drugs (96%), aspirin (89%), and beta-blockers (74%). Thus, Spanish patients with coronary artery disease are similar to those of the other European countries participating in the registry and appear to be representative of the Spanish population with coronary artery disease.
GERIATRIC CARDIOLOGYIn this area, the most relevant studies of 2014 concern heart failure (HF), degenerative aortic stenosis, and atrial fibrillation. In HF, special emphasis has been placed on reducing the number of hospital admissions, the main determinant of the health care cost of HF patients. The developments in aortic stenosis are derived from transcatheter aortic valve implantation, while those in atrial fibrillation concentrate on comparison of the effectiveness and safety of the new oral anticoagulants with those of warfarin in older patients.
Health care reform in the United States has identified reduced hospitalizations due to HF as a priority for achieving a saving in the costs of the health care system. Thus, funding has been reduced for hospitals exceeding certain established standards. Accordingly, and because the prevalence of HF increases with age, Bourge et al14 performed a subanalysis of the classic DIG (Digitalis Investigation Group) study that analyzed the role of digoxin in reducing hospitalization of ambulatory patients older than 65 years with HF and left ventricular systolic dysfunction (ejection fraction < 45%). Digoxin reduced all-cause hospitalizations within 30 days following discharge in these patients (5.4% vs 8.1%; hazard ratio [HR] = 0.66; 95% confidence interval [95%CI], 0.51-0.86; P = .002), with a similar 30-day mortality rate (0.7% vs 1.3%; HR = 0.55; 95%CI, 0.27-1.11; P = .096).
Chaudhry et al15 analyzed the risk factors for hospitalization in geriatric patients with newly diagnosed HF, determining the importance of certain geriatric conditions on hospitalization risk, which reached 7.9 admissions per 10 person-years; the factors independently associated with hospitalization were diabetes mellitus, functional class III or IV of the New York Heart Association, renal failure, slow gait, left ventricular systolic dysfunction, depression, and muscle weakness. The authors state that these conditions should be assessed in older patients diagnosed with HF.
The Edwards SAPIEN prosthesis was used in cohort A of the PARTNER study (the most important randomized trial performed to date, which compared percutaneous transcatheter and surgical implantations of aortic prostheses in patients with degenerative aortic stenosis with high surgical risk). The US CoreValve Pivotal Trial16 compared surgical aortic valve replacement with implantation of a self-expanding transcatheter bioprosthesis (CoreValve®), the other prosthesis model most frequently used in Spain. Patients receiving the transcatheter prosthesis had lower all-cause mortality at 1 year and reduced cardiovascular and cerebrovascular events, bleeding, acute renal injury, and atrial fibrillation. In contrast, they had a higher rate of vascular complications, need for a permanent pacemaker, and cardiac perforation than the patients who underwent the surgical intervention.
Dvir et al17 published the largest series of patients with dysfunctional aortic bioprostheses thus far —40% due to stenosis, 30% due to regurgitation, and 30% due to combined stenosis and regurgitation—who received a transcatheter valve-in-valve aortic prosthesis implant. The 30-day mortality in the 459 patients included was 7.6%. In addition, 1.7% had a stroke and 93% remained in functional class I or II of the New York Heart Association 1 month after the implantation. The mean 1-year survival was 83.2%. Determinants of poor prognosis were the presence of stenosis in the previous bioprosthesis and a small bioprosthesis size. Finally, permanent pacemaker implantation, a frequent occurrence after transcatheter aortic valve implantation, did not increase mortality or hospitalization in these patients but did negatively impact left ventricular function, according to results published by Urena et al.18
In a subanalysis of the ROCKET AF study centered on patients ≥ 75 years old with nonvalvular atrial fibrillation and 2 or more risk factors for stroke, Halperin et al19 reported a higher rate of stroke and major bleeding in older than in younger patients and that the efficacy and safety of rivaroxaban vs warfarin was unaffected by age. Similar results were obtained in a meta-analysis20 of randomized studies comparing the new oral anticoagulants with warfarin in patients ≥ 75 years. The new oral anticoagulants did not increase the risk of bleeding and reduced or were similar to warfarin in reducing embolic events.
One final noteworthy publication was a consensus document21 with recommendations for defibrillator implantation in patients in the final stages of life. These guidelines are useful for decision making in this difficult clinical setting and were developed in a collaboration among the Spanish Society of Geriatric Medicine and Gerontology (Sociedad Española de Geriatría y Gerontología), Spanish Society for Palliative Care (Sociedad Española de Cuidados Paliativos), and the Section of Geriatric Cardiology (Sección de Cardiología Geriátrica) of the Spanish Society of Cardiology (Sociedad Española de Cardiología).
HEART FAILUREThe care management of HF is progressing toward new organizational structures, such as specific programs based on integrated and continuous care, for example, multidisciplinary HF units. Recently, Comín et al22 compared the feasibility and effectiveness of an integrated hospital-primary care program for managing patients with HF compared with the standard approach in 56 742 patients. In the 2083 patients included in the program, vs the 54 659 patients of the other health care areas, there was a lower risk of death (HR = 0.92; 95%CI, 0.86-0.97; P = .005), clinically related readmission (HR = 0.71; 95%CI, 0.66-0.76; P < .001), and rehospitalization for HF.
Heart Failure and Preserved Ejection FractionThere have been no positive developments in this area, given the results of the TOPCAT trial.23 In this study, the addition of spironolactone to optimal medical treatment failed to significantly reduce the composite primary outcome of cardiovascular death, aborted cardiac arrest, or hospitalization for HF. Post hoc analysis of TOPCAT revealed marked national differences in the rates of events. In the Americas (United States, Canada, Brazil, and Argentina), the primary outcome occurred in 27.3% of patients in the spironolactone group vs 31.3% in the placebo group (HR = 0.82; 95%CI, 0.69-0.98; P = .026). However, in patients from Russia and Georgia, the primary outcome occurred in 9.3% of patients treated with spironolactone vs 8.4% of those treated with placebo (HR = 1.10; 95%CI, 0.79-1.51; P = .576). Patients included in Russia and Georgia may not have met the diagnostic criteria for HF and preserved ejection fraction.
Iron Deficiency in Heart FailureIron deficiency is common in HF patients and intravenous administration of ferric carboxymaltose improves symptoms and health-related quality of life in patients with HF and reduced ejection fraction, in accordance with the results of the FAIR-HF (Ferinject® Assessment in patients with Iron deficiency and chronic Heart Failure) study. Because there were no long-term data on the use of this therapeutic strategy, the CONFIRM-HF (Ferric CarboxymaltOse evaluatioN on perFormance in patients with IRon deficiency in coMbination with chronic Heart Failure) trial was designed. This study included 304 patients with HF and reduced ejection fraction and iron deficiency (ferritin < 100 ng/mL or 100-300 ng/mL if transferrin saturation was < 20%). After 52 weeks, treatment with ferric carboxymaltose significantly improved the 6-minute walk test results (mean (SD) difference between ferric carboxymaltose and placebo: 33 (11) m; P = .002), symptoms, and health-related quality of life, and significantly reduced the risk of hospitalization due to HF (HR = 0.39; 95%CI, 0.19-0.82; P = .009).24
New Drugs for Chronic Heart FailureMineralocorticoid receptor inhibitors have improved the prognosis of HF and reduced ejection fraction but their use is limited due to hyperkalemia and renal failure. BAY 94-8862 is a powerful and highly selective nonsteroidal mineralocorticoid receptor inhibitor. The safety and tolerability of this new molecule was evaluated in patients with HF and reduced ejection fraction and mild or moderate chronic renal failure in the ARTS trial.25 In this study, the use of BAY 94-8862 was associated with a lower incidence of hyperkalemia (5.3% vs 12.7%; P = .048), less worsening of renal function, and a significant reduction in Nt-proBNP (aminoterminal brain natriuretic peptide fraction) levels.
The most important progress in HF and reduced ejection fraction has been the development of ARNIs (angiotensin receptor-neprilysin inhibitors). LCZ696, the first drug of this new therapeutic class, is composed of 2 molecular fractions: on the one hand, an inhibitor of the neprilysin enzyme, which increases natriuretic peptides and, thus, their beneficial effects (vasodilation, natriuresis, and sympathetic blockade); on the other hand, valsartan, which inhibits the effects of angiotensin II.
The PARADIGM-HF randomized, double-blind trial26 included 8436 patients with symptomatic HF and left ventricular ejection fraction ≤ 40%. The primary outcome was the composite of cardiovascular death or hospitalization due to HF. Patients were randomized to receive LCZ696 200mg/12h or enalapril 10mg/12h, in addition to optimal medical treatment. After a mean follow-up of 27 months, the primary outcome of the study occurred in 21.8% of patients treated with LCZ696 vs 26.5% of patients treated with enalapril (HR = 0.80; 95%CI, 0.73-0.87; P < .001). Compared with enalapril, LCZ696 reduced total mortality by 16%, cardiovascular death by 20%, and hospitalization due to HF by 21%. The most frequent adverse events with LCZ696 were hypotension and mild angioedema; in contrast, LCZ696 reduced the onset of renal failure, hyperkalemia, and cough compared with enalapril.27
Devices and BiomarkersThere are more and more devices that incorporate telemonitoring, which sends clinical data recorded to monitoring centers, such as implantable cardioverter-defibrillators and cardiac resynchronization defibrillators. The IN-TIME trial28 evaluated the impact of telemonitoring on improving the clinical status of patients with HF. The study included 664 patients with chronic HF with ejection fraction < 35% and compared those who received implants with telemonitoring function with control patients. The main evaluation criterion was a composite clinical score. At 12 months follow-up, 27.2% of patients in the control group experienced clinical worsening according to the composite outcome compared with 18.9% in the telemonitoring group (P = .013). In addition, the 1-year mortality was 8.7% in the control group and 3.4% in the telemonitoring group (P = .0004).
Another area that had generated high expectations is that of vagal stimulation. The NECTAR-HF trial29 failed to corroborate the initial data showing improved ventricular remodeling in patients with HF and reduced ejection fraction. In this randomized study, right vagal nerve stimulation failed to induce significant changes in ventricular remodeling, functional capacity, or biomarkers. Significant differences between the groups were only seen in health-related quality of life.
The use and application of HF biomarkers continues to grow and there are now new HF- and renal lesion-related biomarkers. One important development is a new model for stratifying risk in patients with HF: the BCN Bio-HF calculator. Developed by Lupón et al,30 this tool incorporates 3 biomarkers: NT-proBNP, high-sensitivity cardiac troponin T, and high-sensitivity soluble ST2. The BCN Bio-HF calculator was obtained via analysis of 864 consecutive outpatients who were followed up for a median of 3.4 years (305 deaths) and after an initial evaluation of 23 variables included in 8 independent models.
Acute Heart FailureInotrope use in acute HF can cause problems with myocardial ischemia, arrhythmias, and increased mortality. Omecamtiv mecarbil is a new inotropic agent that activates myocardial ATPase to improve the formation of actin-myosin bridges and increase the ventricular ejection time, contraction force, and systolic volume, without changing the myocardial consumption of oxygen or intracellular calcium. In the ATOMIC-AHF study,31 which included 613 patients with left ventricular ejection fraction ≤ 40% and a history of symptomatic HF, 3 increasing doses of omecamtiv mecarbil intravenously administered for 48hours were compared with placebo. The main end point, improvement in dyspnea at 6, 24, and 48hours, was not reached; however, a more adjusted analysis of the sample did show a positive tendency with the higher doses. Doubts regarding the drug and the study arose after it was determined that there were a higher number of ischemic events and higher level of troponin I in the omecamtiv mecarbil group. Thus, we have to wait for phase III studies to confirm its use for acute HF.
After the expectations created by the RELAX-AHF (Efficacy and Safety of Relaxin for the Treatment of Acute Heart Failure) trial of the use of serelaxin in acute HF, efforts have focused on better understanding its beneficial effects and, particularly, its hemodynamic action. One recent double-blind and randomized study evaluated the hemodynamic effects of serelaxin in 71 patients with acute HF (intravenous perfusion of 30μg/kg/day for 20h). Patients treated with serelaxin had significantly reduced pulmonary capillary pressure and pulmonary arterial pressure, without changes in the cardiac index. Intravenous cardiac serelaxin was safe and improved renal function parameters and Nt-proBNP values.32
Finally, another family of HF drugs activates soluble guanylate cyclase. This protein plays a key role in the mechanism of action of nitric oxide because its activation induces the production of cyclic guanosine monophosphate, which essentially generates vasodilation. In the LEPHT,33 riociguat, a new activator of soluble guanylate cyclase, had minor effects in patients with pulmonary hypertension secondary to left ventricular dysfunction. BAY 1021189, another activator of soluble guanylate cyclase, is currently being evaluated in 2 phase II studies of patients with HF with reduced and preserved ejection fraction.
Advanced Heart Failure and Heart TransplantationPalliative use of intravenous inotropes in patients with advanced HF is clinically widespread, despite little published evidence. The LevoRep study34 evaluated levosimendan use in this type of patient. This randomized, double-blind, and placebo-controlled study included 120 patients with advanced HF who received 0.2μg/kg/min levosimendan for 6h every 15 days (4 cycles in total). The study failed to show a significant improvement in functional capacity and health-related quality of life, the main components of the primary end point. Levosimendan was safe and associated with a lower rate of cardiac mortality, indication for cardiac transplant, and the presence of acute HF.34 The results of the Spanish LION trial are currently being awaited, as this study evaluated a similar approach in the same patient profile.
Implantations of mechanical ventricular assist devices with continuous flow pumps continue to increase. The good results shown by the new third-generation mechanical ventricular assist devices with continuous flow pumps (HeartWare HVAD®) are widening the indications and, particularly, the definitive or destination therapy. The latest annual report of INTERMACS35 reviewed the first 8 years of patient enrollment, with more than 10 000 implantations of mechanical ventricular assist devices; the actuarial survival is still 80% at 1 year and 70% at 2 years.
In heart transplantation, cellular rejection is one of the main causes of morbidity and mortality. It is still being diagnosed using invasive methods, such as endomyocardial biopsy. A recent study36 showed that cellular rejection could be identified using a noninvasive biomarker such as microRNA. After including 113 heart transplant recipients, the authors observed 4 microRNAs with differential serological expressions (miR-10a, miR-31, miR-92a, and miR-155) and strong correlations with their tissular expression in cellular rejection. In ROC analysis, miR-10a (AUC [area under the curve] = 0.976), miR-31 (AUC = 0.932), miR-92a (AUC = 0.989), and miR-155 (AUC = 0.998) were significant (P < .0001) for all comparisons. This study supports the previous good results with noninvasive molecular techniques for assessing cellular rejection in heart transplantation.
CONFLICTS OF INTERESTSNone declared.