Although neonatal acute myocardial infarction secondary to coronary thrombosis is extremely rare, it has high mortality (about 90%)1 and its early diagnosis requires a high level of clinical suspicion. Of the few cases described in the literature, most are of unknown origin.2 Reported risk factors include prothrombotic conditions, myocarditis, prematurity, neonatal asphyxia, Kawasaki disease, and placement of an umbilical venous catheter.1–4 Various therapeutic strategies are available, such as surgical thrombectomy,5 systemic or local thrombolytic treatment (although controversial in neonates, there have been some successful results),2,4 and use of an extracorporeal membrane oxygenator as hemodynamic support.2–6
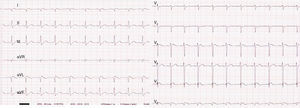
The present scientific letter concerns a male neonate, with no relevant obstetric history except for maternal gastroenteritis at 12 days before birth, who was born at 37+5 weeks gestation via emergency cesarean section due to pathological cardiotocography (DIP II). His Apgar score was 6/9. At birth, he required positive pressure ventilation for 3min due to poor respiratory effort. He was admitted to the neonatal intensive care unit under clinical management and continuous monitoring. There, a marked progressive clinical worsening was seen, with a poor general status and mixed acidosis that required intubation, mechanical ventilation, and refractory intensive inotropic support. For the latter, he was administered stress doses of hydrocortisone. Echocardiography was performed to rule out cardiogenic shock as a differential diagnosis, revealing severe ventricular dysfunction with ejection fraction <15%, with minimal motion of the lateral wall but with preserved right ventricular function. Both coronary arteries were adequately visualized, but no visualization was possible of left coronary artery flow. In addition, a 12-lead electrocardiogram showed deep Q waves in DI, aVL, and V5-V6 (Figure 1).
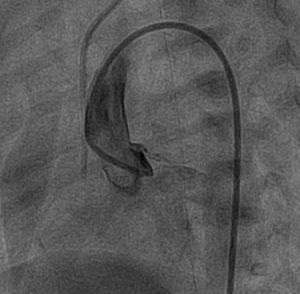
With the diagnosis of cardiogenic shock due to acute left ventricular dysfunction, treatment was begun with prostaglandins to maintain systemic cardiac output through the arterial conduit. The differential diagnosis included myocarditis (due to the maternal history of gastroenteritis), coronary thrombosis, and an anomalous origin of the left coronary artery in the pulmonary artery (although it was unlikely because symptoms do not usually begin until pulmonary resistance decreases). Treatment was started with intravenous gamma-globulins and acyclovir, and it was decided to perform cardiac catheterization. Due to the patient's considerable hemodynamic instability, catheterization was delayed until the fourth day of life, but revealed a filling defect of 1 m in diameter in the left coronary artery, compatible with a thrombosis or dissection of the left main coronary artery (Figure 2, ), confirming the diagnosis of acute myocardial infarction due to thrombosis of the left coronary artery. Initial treatment was to consist of intravenous heparin and systemic r-TPA (recombinant tissue plasminogen activator) or acetylsalicylic acid but, due to the shock-induced coagulopathy, the considerable risk of brain bleeding, and the late diagnosis, treatment was begun with intravenous heparin alone for 7 days, at a dosage of 1.5mg/kg body weight every 12hours. The first percutaneous treatment considered was placement of an intracoronary stent, but this approach was rejected due to the risk-benefit of stent implantation in a neonate. Another possibility was intracoronary administration of r-TPA, but recovery of myocardial viability was considered unlikely due to the delayed diagnosis. In the following days, reopening of the coronary artery was seen on ultrasound, but with minimal recovery of ventricular function (30% ejection fraction). Serological and polymerase chain reaction studies of the blood for the presence of virus were negative, as were thrombophilic studies. The patient remained in the neonatology unit for 94 days due to his considerable hemodynamic lability in response to minimally invasive procedures and intercurrent processes. He was eventually discharged with diuretic therapy, digoxin, carvedilol, acetylsalicylic acid, and nasogastric feeding. During his clinical course, he was admitted several times to the pediatric intensive care unit for cardiac decompensation in the presence of catarrhal symptoms. He was included on the transplant list at 12 months of life and received a transplant 5 months later, with good outcome. Histopathology of the explanted heart showed a dilated left ventricle, with extensive areas of fibroelastosis, and almost half of the external myocardium in the free wall had been replaced by adipose tissue and fibrosis. No coronary obstruction was detected.
Acute myocardial infarction in the neonatal period is exceptional and represents a considerable diagnostic and therapeutic challenge for clinicians and cardiologists. Early diagnosis via electrocardiography, echocardiography, and catheterization is important for adequate treatment and to promote coronary reperfusion because these patients often lack adequate collateral circulation. Prompt treatment could avoid the irreversible myocardial necrosis3,6 that culminates in heart transplantation, as in our patient. Various therapeutic options have been described, but there is no universal consensus because few such patients have been described and because newborns are highly susceptible to immaturity-related complications.2 The most recent articles advocate local thrombolytic treatment with low-dose intracoronary r-TPA, together with the administration of intravenous heparin, with good results and without complications.2,4–6