Intravenous administration of metoprolol during ongoing ischemia has been demonstrated to be associated with smaller infarct size (IS) in animal models1,2 and in the METOCARD-CNIC clinical trial.3 Clinical practice guidelines recommend (IIa-A) the use of intravenous beta-blockers at the time of presentation in patients with ST-segment elevation myocardial infarction (STEMI) who are hemodynamically stable.4 However, in some cases, physicians do not prescribe iv beta-blockers to STEMI patients because of the fear that they can develop acute heart failure. There are beta-blockers with a very short half-life that have the theoretical advantage that, upon stopping infusion, their negative inotropic and chronotropic effects disappear within minutes. Given that not all beta-blockers are able to ameliorate ischemia/reperfusion injury,2 there is a need to test the cardioprotective abilities of short-acting beta-blockers in a controlled experimental setting.
Esmolol is a highly beta1-selective, ultra-short-acting beta-blocker with rapid onset of action (60seconds) that reaches steady state in 6minutes after bolus administration. These pharmacological properties make esmolol a great candidate for use in the setting of STEMI when hemodynamic instability is a potential concern. In this study, we aimed to evaluate the infarct-limiting capacity of esmolol infusion during ongoing ischemia in a pig model of anterior STEMI. The benefits of esmolol were evaluated by state-of-the-art cardiac magnetic resonance (CMR) performed at 2 different timepoints: 7 and 45 days after reperfusion. The primary endpoint of the study was day 7 indexed IS: extent of delayed gadolinium enhancement, normalized to area at risk. Area at risk (AAR) was quantified by cardiac computed tomography (CT) performed during index left anterior descending (LAD) occlusion following a previously reported methodology.5 The main secondary endpoints were indexed IS at 45-day and left ventricular ejection fraction (LVEF) on both CMR exams.
The experimental protocol was approved by the local and Community of Madrid animal welfare committee. Experiments were performed according to current legislation. Before the actual ischemia/reperfusion experiments, a dose-response study with 5 animals was conducted to determine the most appropriate esmolol infusion rate: that achieving a 10% reduction of heart rate without sustained hemodynamic instability (250μg/kg/min).
Fifteen male large-white pigs underwent 40minutes of left anterior descending (LAD) coronary occlusion followed by reperfusion. Pigs were randomized to receive either esmolol (n=8) or control (vehicle infusion, n=7), which were initiated (without bolus) 20minutes after LAD artery occlusion, and maintained for a total of 60minutes (ie, it was stopped 40minutes after reperfusion). Since the main objective of the study was to test the infarct-limiting properties of esmolol, the infusion rate was not modified during the protocol, even in those pigs developing hemodynamic instability.
Three animals (2 esmolol and 1 control) died during STEMI induction. The 2 esmolol pigs died secondary to severe hemodynamic instability caused by esmolol infusion, while the control died because of refractory ventricular fibrillation. Three additional pigs (2 esmolol and 1 control) died between day 7 and day 45 CMR.
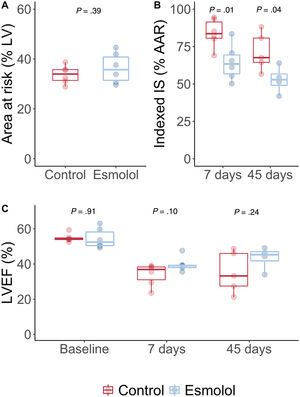
CT-measured AAR did not differ between groups (36.4%±6.1% vs 33.7±3.6% of left ventricular (LV) in esmolol and control, respectively; P=.385), figure 1A. IS was significantly smaller in the esmolol group both in the 7-day (64.4±11.8% vs 84.1±9.4% of AAR; P=.01) and in the 45-day CMR (52.9±9.1% vs 71.5±12.7%; P=.04), figure 1B. Animals in the esmolol group showed a nonsignificant trend toward higher LVEF both at 7- and 45-day CMR (day 7: 39.74.1% vs 34.0±6.2%; P=.091; day 45: 43.4±6.6% vs 35.3±11.8%; P=.264), figure 1C. There were no differences in microvascular obstruction or in edema extension.
A: area at risk (% of LV mass) on computed tomography exam during index coronary occlusion. B: indexed infarct size (% of AAR with delayed gadolinium enhancement) on 7- and 45-day CMR. C: left ventricular (LV) ejection fraction (LVEF) at different timepoints. Boxplots represent median and interquartile range. Circles represent individual data. AAR, area at risk.
In this experimental setting, continuous esmolol infusion initiated during ongoing ischemia was associated with smaller IS and with a trend toward improved LVEF. The numerically higher number of deaths due to hemodynamic instability during the index STEMI can be explained by the experimental protocol aimed at addressing the infarct-limiting properties of esmolol. We speculate that, in a clinical setting, these adverse effects would not occur because, upon signs of acute heart failure, infusion can be reduced or event stopped. Whether this tailored esmolol infusion will reduce IS is unknown, but highly plausible. The main limitation of this study is the loss of 50% of the animals in the esmolol group and 29% in the control group. This experimental study complements previous clinical studies suggesting that esmolol can protect the heart during STEMI.6 Given that not all beta-blockers exert infarct-limiting effects,2 the effects seen with esmolol cannot be ascribed to other short-acting beta-blockers.
In conclusion, this study shows that esmolol infusion is able to reduce indexed IS in an experimental acute myocardial infarction model and shows a trend toward LVEF improvement. However, there are safety concerns regarding hemodynamic instability that require further evaluation.
FUNDINGThis study was funded by a grant from the Spanish Society of Cardiology Investigación Traslacional 2017. J. Nuche is a recipient of a predoctoral grant Jordi Soler Soler from the CIBERCV. The CNIC is supported by the Instituto de Salud Carlos III (ISCIII), the Ministerio de Ciencia e Innovación and the Pro CNIC Foundation, and is a Severo Ochoa Center of Excellence.
AUTHORS’ CONTRIBUTIONSJ. Nuche: design of the protocol, performance of experiments, data analysis, and drafting of the manuscript. S. Huertas: performance of experiments. C. Galán-Arriola: performance of experiments. Analized data. P. López-Ayala: performance of experiments. Critical revision of the manuscript. M. Lobo: performance of experiments. B. Ibáñez: conceptual design of the study. Handling of funding. Critical revision of the manuscript.
CONFLICTS OF INTERESTNone.