Catheterization techniques are essential in the diagnosis and treatment of certain cardiac diseases, but the ionizing radiation used in some of these procedures is associated with health risks for patients and health care staff alike. The radiation doses should be minimized as far as possible. The impact of interventional techniques on the radiation dose received is not negligible. According to the 2011 activity registry of the Spanish Society of Cardiology Working Group on Cardiac Catheterization,1 2998 diagnostic studies and 1368 percutaneous coronary interventions were performed per million population. The Spanish legislation requires individual registration of the radiation dose received in interventional procedures.2 The International Commission on Radiological Protection recommends that levels of reference doses be established for different fluoroscopy-guided procedures to optimize the doses administered to patients.3 Reference values should not be applied in an individual manner because due to complexity reasons or the patient's size these could be exceeded. However, if the reference values were exceeded in a large number of patients, corrective actions would need to be taken.
With the aim of investigating and proposing updated reference dosage values for patients undergoing catheterization procedures, the DOCCACI (DOsimetría y Criterios de Calidad en Cardiología Intervencionista in Spanish, or Dosimetry and Quality Criteria in Interventionist Cardiology in English) group was formed in 2010, under the auspices of the Spanish Society of Cardiology Working Group on Cardiac Catheterization. The list of professionals who constitute the DOCCACI group can be found in the supplementary material that accompanies this article.
Seven public hospitals in 6 different Spanish autonomous communities joined the project. In each center, a catheterization cardiologist and a radiophysicist took on responsibility for providing data on the radiation dose administered to the patients.
The working group was limited initially to the most common procedures, coronary angiography (CA) and percutaneous transluminal coronary angioplasty (PTCA). The PTCA procedures included both those deferred after a prior CA and a CA with PTCA in the same procedure.
The dose indicator most used for patients in interventional techniques is the dose-area product, which is defined as the integral of kerma in air over the radiation field and expressed in units of dose per area, generally in Gy·cm2. Since 2010, as part of the DOCCACI program, anonymous data have been collected that include the type of procedure, dose-area product, fluoroscopy time, number of sequences, and the total number of cine images acquired. Some of the centers with automatic data collection systems via DICOM connections with the devices have acquired a large amount of data without noting the complexity of the cases. The centers that have manually compiled the data and provided the smallest samples selected the cases with normal complexity.
The reference values were calculated for dose-area product, fluoroscopy time, number of sequences, and the total number of cine images acquired as the third quartile of the medians of the distributions in each center. Using this methodology, all centers had the same statistical weight in the calculation of the reference values.
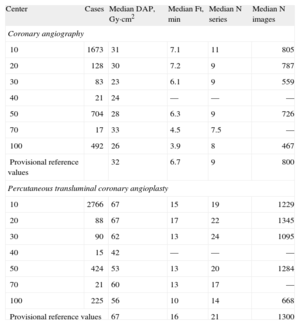
Information was collected for 2802 CA and 3576 PTCA procedures. The Table shows the medians of the dose-area product, fluoroscopy time, number of series, and number of cine images for each center. The last row presents the provisional reference values.
Most Representative Statistical Values of Dose Received by Patients in Participating Centers
| Center | Cases | Median DAP, Gy·cm2 | Median Ft, min | Median N series | Median N images |
| Coronary angiography | |||||
| 10 | 1673 | 31 | 7.1 | 11 | 805 |
| 20 | 128 | 30 | 7.2 | 9 | 787 |
| 30 | 83 | 23 | 6.1 | 9 | 559 |
| 40 | 21 | 24 | — | — | — |
| 50 | 704 | 28 | 6.3 | 9 | 726 |
| 70 | 17 | 33 | 4.5 | 7.5 | — |
| 100 | 492 | 26 | 3.9 | 8 | 467 |
| Provisional reference values | 32 | 6.7 | 9 | 800 | |
| Percutaneous transluminal coronary angioplasty | |||||
| 10 | 2766 | 67 | 15 | 19 | 1229 |
| 20 | 88 | 67 | 17 | 22 | 1345 |
| 30 | 90 | 62 | 13 | 24 | 1095 |
| 40 | 15 | 42 | — | — | — |
| 50 | 424 | 53 | 13 | 20 | 1284 |
| 70 | 21 | 60 | 13 | 17 | — |
| 100 | 225 | 56 | 10 | 14 | 668 |
| Provisional reference values | 67 | 16 | 21 | 1300 | |
DAP, dose-area product; Ft, fluoroscopy time.
The provisional reference values obtained by this working group are lower than those published in 2008 by the group coordinated by the International Atomic Energy Agency,4 which gave reference values of 50 and 125Gy·cm2 for CA and PTCA, respectively, compared to 32 and 67Gy·cm2 in this study. Other variables were also lower in the Spanish program, such as fluoroscopy time (6.7 vs 9.0min in CA and 16 vs 22min in PTCA) or the number of images (800 vs 1000 for CA and 1300 vs 1700 for PTCA). Although the advances in imaging devices technology in the last 10 years could have some impact on the decreases in dose, this has not been observed in published studies. The decreases could be explained by more effective optimization programs and dose recording. Looking at the Table, it can be seen that there are large differences between centers for some of the variables studied, both in the case of CA and PTCA procedures. This suggests that there is still room for optimization.
Follow-up of these aspects of radiologic protection should continue to verify the sustainability of the reference values and ensure that changes in technology are not associated with an increase in the dose that patients receive unless there is a clear clinical benefit. The Catheterization Working Group is committed to continue with this program.
FUNDINGThis study was financed partially by the SAF2009-10485 project of the Ministry of Economy and Competition and the EVC.F01CSN project of the Nuclear Safety Council.
Note
An independent ethics committee approved this study under the title “Radiological risks in fluoroscopy-guided procedures” (B-09/20). These results have been accepted in part for publication as a brief communication in the abstracts book of the International Conference on Radiation Protection in Medicine, sponsored by the International Atomic Energy Agency and the World Health Organization, held in Bonn, Germany, in December 2012.