During pregnancy, there are a number of important changes to cardiovascular function which are necessary for progression of a successful pregnancy. Additionally, preexisting cardiovascular conditions can be exacerbated by the adaptations that occur during gestation. These can present serious therapeutic challenges in the management of the cardiology patient during pregnancy. Significantly, the number of pregnant women at risk of cardiovascular complications is on the rise, so identification of risk factors that predict cardiac outcomes is essential to proper screening of the obstetrical patient. In diagnosed preexisting conditions, such as pulmonary hypertension, counseling is important prior to pregnancy. In the case of underlying disorders unmasked by pregnancy, or new-onset complications like preeclampsia, appropriate monitoring and treatment of the cardiovascular complications is warranted. Ultimately, collaborative care by both obstetricians and cardiologists is essential for the successful resolution of cardiovascular dysfunction in the obstetrical patient.
Keywords
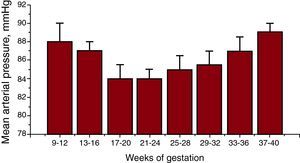
A variety of changes in the cardiovascular system occur during normal pregnancy, including increases in cardiac output, arterial compliance, and extracellular fluid volume and decreases in blood pressure (BP) and total peripheral resistance.1 Mean BP gradually falls during pregnancy, with the largest decrease in BP typically occurring at 16 to 20 weeks.2 BP then begins to rise during the mid-third trimester to levels approaching prepregnancy BP values (Figure 1). The decrease in BP during pregnancy is characterized by decreases in both systolic BP (SBP) and diastolic BP (DBP) with the decrements in DBP exceeding those in SBP.
Figure 1. Mean arterial pressure in women during normal pregnancy (Redrawn from Moutquin et al. 2 ).
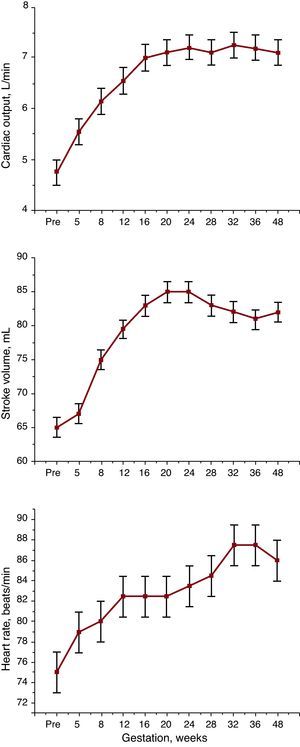
Blood flow to various organs increases during pregnancy to meet the increased metabolic needs of tissues. Thus, venous return and cardiac output increases dramatically during pregnancy. Cardiac output gradually increases during the first 2 trimesters with the largest increase occurring by 16 weeks of gestation.3 The increase in cardiac output is well established by 5 weeks of gestation and increases to 50% above prepregnancy levels by 16 to 20 weeks of gestation. The rise in cardiac output typically plateaus after 20 weeks of gestation and remains elevated until term. The increases in cardiac output are associated with significant increases in stroke volume and heart rate (HR) (Figure 2). Mean circulatory filling pressure, an important determinant of venous return, is also elevated during pregnancy. Moreover, resistance to venous return is dramatically reduced during pregnancy.
Figure 2. Changes in cardiac output, stroke volume, and heart rate during pregnancy (Redrawn from Hunter et al. 3 ).
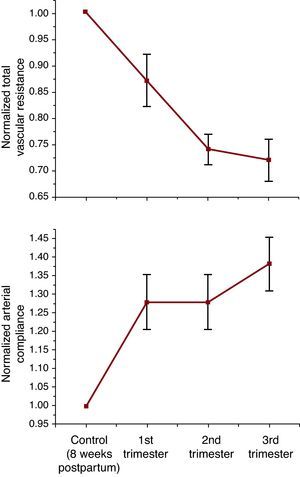
The increased cardiac output and slight decrease in BP during pregnancy is associated with a marked reduction in systemic vascular resistance.4 Total peripheral resistance decreases very early during pregnancy and continues to decrease throughout the second and third trimester, although to a lesser extent near term (Figure 3). Arterial compliance also changes dramatically during pregnancy. Arterial compliance increases during the first trimester and remains elevated throughout the remainder of pregnancy. Thus, both steady and pulsatile afterload decreases occur during normal pregnancy in humans.
Figure 3. Changes in total vascular resistance and arterial compliance during normal pregnancy (Redrawn from Poppas et al. 4 ).
While the mechanisms responsible for mediating the changes in systemic hemodynamics have yet to be completely elucidated, a number of important factors are thought to contribute to physiological changes in the vascular system that occur during pregnancy. Substantial evidence indicates that nitric oxide (NO) production is elevated in normal pregnancy and that these increases appear to play an important role in the vasodilation of pregnancy.5 Inhibition of NO synthesis in animal models of pregnancy attenuates the decreases in total peripheral resistance and increases in cardiac output associated with pregnancy.
Hormonal factors such as estrogen and relaxin are thought to be important in stimulating the production of NO during pregnancy. Relaxin, which is primarily produced by the corpus luteum, has been shown to chronically reduce total peripheral resistance and increase cardiac output and systemic arterial compliance.6 In addition, neutralization of endogenous circulating relaxin by antibodies during early gestation markedly attenuate the changes in cardiac output, systemic vascular resistance, and arterial compliance during pregnancy. These effects of relaxin are thought to be mediated by interactions between endothelin type B receptors and NO. Thus, relaxin appears to play an important role in many of the cardiovascular adaptations of pregnancy via NO-dependent mechanisms.
PREGNANCY AND HEART DISEASEAlthough maternal cardiac disease complicates a small percentage of pregnancies overall, it is a significant cause of nonobstetrical maternal and fetal morbidity and mortality.7 Pregnancy is associated with significant hemodynamic changes, namely volume expansion and increased cardiac output, which in the setting of underlying maternal cardiac disease may lead to decompensation and fetal demise. In addition to the hemodynamic changes imposed by the gravid state, factors such as peripheral vasodilation from anesthesia or blood loss that may occur with delivery may aggravate cardiac dysfunction in women with significant underlying cardiac disease (Table 1).
Table 1. Conditions Associated With High Risk of Maternal Complications During Pregnancy.
| Pulmonary hypertension |
| Eisenmenger syndrome |
| Marfan syndrome with aortic dilatation |
| Severe left ventricular systolic dysfunction |
| Peripartum cardiomyopathy |
| Severe preeclampsia |
Congenital heart disease is becoming more prevalent in women of childbearing age as a result of improved diagnostic modalities and reparative techniques.8 Furthermore, acquired heart disease has become more prevalent now that many women are postponing pregnancy until later ages when the risk of cardiovascular disease is increased due to hypertension (HTN), diabetes, and obesity. Risk assessment in women with underlying cardiac disease is crucial. In a prospective study of 562 consecutive pregnant women with heart disease, 13% of pregnancies were complicated by primary cardiac events, defined as pulmonary edema, arrhythmia, stroke, or cardiac death.9 The predictors of cardiac events were prior cardiac events or arrhythmias, poor functional class (defined as New York Heart Association (NYHA) class III-IV heart failure [HF]) or cyanosis, left heart obstruction (mitral valve area <2cm2, aortic valve area <1.5cm2, or peak left ventricular [LV] outflow gradient >30mmHg), and LV dysfunction defined as LV ejection fraction (EF) <40%. It is therefore imperative that women with both acquired and congenital cardiac conditions be counseled about avoiding pregnancy and be evaluated and monitored if they become pregnant.
HEART FAILUREParticularly in the third trimester, the hemodynamic changes that occur can lead to clinical decompensation in women with underlying cardiomyopathies. Normal physical findings associated with pregnancy often include tachycardia, S3 gallop, systolic “flow” murmur, peripheral edema, and sometimes jugular venous distension which may obscure a diagnosis of HF in the gravid female. Also, many women with normal pregnancies experience symptoms such as dyspnea or orthopnea that may mask the presence of underlying LV dysfunction. It is in these settings where diagnostic testing such as brain natriuretic peptide levels or an echocardiogram may be useful.
Women with stable underlying LV systolic dysfunction can often undergo pregnancy safely when closely monitored for both maternal and fetal decompensation in a coordinated manner by both a cardiologist and obstetrician, although there is some associated increased risk for both the mother and fetus. The goals of medical therapy in these patients are to relieve volume overload with diuretics and optimize medical therapy for control of BP and afterload reduction. Pregnant patients with HF should be managed similarly to nonpregnant patients with the exception of the use of angiotensin converting enzyme inhibitors or angiotensin receptor blockers due to high risk of adverse effects in the fetus with these drugs. Afterload reduction can instead be achieved with arterial vasodilators such as hydralazine with or without the addition of long-acting nitrates. Beta blockers are typically safe in pregnancy for patients with chronic systolic dysfunction but should be avoided in acute decompensated HF. The use of β-1 specific agents is preferred to minimize β-2 induced peripheral vasodilation and uterine relaxation. Digoxin, an inotropic agent, is generally safe in pregnancy but needs to be monitored as excess levels are associated with adverse outcomes in women.10 Women who present with decompensated HF often require more aggressive diuresis and sometimes require inotropic support with dobutamine or phosphodiesterase inhibitors such as milrinone, which also act as vasodilators.
Both HF and pregnancy are associated with a hypercoagulable state. There are no clear guidelines on anticoagulation in pregnant women with significant LV systolic dysfunction but prophylactic anticoagulation is reasonable to prevent intracardiac thrombi and embolic events in patients with EF <30%-35%.11 Warfarin is typically contraindicated in the first trimester of pregnancy due to its teratogenicity but women may be treated with unfractionated heparin (UH) or low molecular weight heparin (LMWH) instead. Current guidelines recommend either LMWH or UH subcutaneously twice daily throughout pregnancy or UH or LMWH subcutaneously twice daily until week 13 followed by warfarin during weeks 13 to 35 and resuming UH/LMWH until delivery.12
PERIPARTUM CARDIOMYOPATHYPeripartum cardiomyopathy (PPCM) is defined as the development of LV systolic dysfunction and HF between the last month of pregnancy and within 5 months of delivery in the absence of another identifiable cause of LV dysfunction.13 The etiologies are poorly understood but may be related to inflammation, immune system activation, or myocarditis. The clinical presentation is similar to other forms of HF and women should be treated similarly to other cardiomyopathies. The role of endomyocardial biopsy in this setting remains unclear but may reveal patients with evidence of myocarditis. In a retrospective study of 6 women with PPCM treated with intravenous immunoglobulin (IVIG) compared to 11 women controls treated conventionally, women treated with IVIG had significantly greater improvement in EF (increase of 26±8% vs 13±13%) after 6 months.14 Bromocriptine treatment also elicited significant improvement in EF compared to conventional therapy in a small study.15 However, similarly to IVIG, more studies are needed to determine the safety and efficacy of the use of both agents in addition to standard HF therapy in the setting of PPCM. Ventricular function improves in about half of patients and normalization of LV systolic function is less likely in patients with LVEF <30%,16 LV end diastolic dimension >6cm,17 and elevated troponin T levels18 at the time of diagnosis. Because of the relatively high chance of having recurrent LV systolic dysfunction in women who have had normalization of EF, they should be counseled along with any women with a history of PPCM to avoid subsequent pregnancies due to increased risk of HF progression and possibly death.
VALVULAR DISEASEValvular heart disease includes both congenital and acquired lesions. Maternal and fetal risks generally vary based on the specific lesion and the maternal functional classification. As mentioned previously, lesions associated with poorer NYHA functional class (NYHA III-IV) or reduced EF have worse prognoses. Mitral stenosis (MS) secondary to rheumatic disease is the most common valvular lesion in pregnant women. Tachycardia associated with the gravid state shortens LV diastolic filling time, increasing the transmitral valve gradient and left atrial pressure, which can compromise maternal hemodynamics. The further increase in HR associated with the pushing and pain during labor can cause significant drops in an already restricted cardiac output. Beta blockers or calcium channel blockers can be used to blunt tachycardia in these patients. Care must be taken to avoid drastic reductions in preload (eg, with overaggressive diuresis or with anesthesia) as these patients often require higher than normal LV filling pressures to maintain cardiac output. Pulmonary artery catheterization monitoring may be required in patients with severe obstruction. Percutaneous balloon mitral valvotomy is reasonable for pregnant patients who develop severe symptoms attributable to MS.19
Aortic stenosis (AS) in women of childbearing age is most often due to a congenital bicuspid valve and is less commonly seen. There is impaired LV outflow across the valve that can only be increased by increasing HR. However, excessive increases in HR can reduce preload and myocardial oxygen consumption. Severe AS is also associated with systemic vasodilation; therefore it is crucial, particularly during labor and delivery, to avoid further drops in preload (ie, bleeding, Valsalva, or anesthesia) or afterload which may exacerbate the already reduced cardiac output.
Regurgitant valvular lesions such as mitral or aortic insufficiency are generally well tolerated if associated with no or mild HF symptoms (NYHA class I-II). The normal fall in systemic vascular resistance associated with pregnancy reduces afterload and subsequently the amount of regurgitant flow across the valve unless severe. Epidural anesthesia further reduces peripheral resistance, improving forward cardiac output.
ARRHYTHMIASMost arrhythmias that occur in pregnancy in the absence of structural heart disease are benign and transient. Symptomatic and recurrent tachyarrhythmias should be evaluated to rule out exacerbating factors such as structural cardiac abnormalities, hyperthyroidism, or pulmonary embolism. Any hemodynamically unstable or life-threatening arrhythmias should be electrically cardioverted or defibrillated per Advanced Cardiac Life Support guidelines. Patients with stable, symptomatic arrhythmias may be managed pharmacologically with agents that have the fewest potential adverse effects to the fetus. Patients with atrial fibrillation or atrial flutter should be considered for anticoagulation therapy.
PREECLAMPSIAPreeclampsia (PE) is characterized by the new onset of HTN defined as SBP≥140mmHg or DBP≥90mmHg and proteinuria in a previously normotensive woman after 20 weeks gestation. The pathogenesis or PE is not well understood but may involve abnormalities in placental vascular development in early pregnancy resulting in relative placental ischemia or hypoxemia and release of antiangiogenic substances (ie, s-Flt-1 and soluble endoglin) into the maternal circulation leading to vascular endothelial dysfunction and HTN.20 Some of the factors associated with increased risk of developing PE include history of PE in previous pregnancy or family history of PE, nulliparity, chronic HTN or renal disease, high body mass index, or age >40 years.21 The associated HTN and proteinuria typically present in the third trimester and progress until delivery.
Besides HTN and proteinuria, PE is associated with generalized edema, hypercoagulability, thrombocytopenia, and sometimes target organ damage to the liver or kidneys. Patients may experience central nervous system symptoms such as headaches or blurred vision and if they develop seizure activity are characterized as having eclampsia. The definitive treatment for PE is delivery of the fetus to prevent maternal or fetal complications; the decision on whether or not to deliver depends on gestational age, maternal-fetal stability, and severity of PE. Women with mild disease who are managed conservatively should reduce their physical activity and have frequent follow up maternal and fetal evaluations and laboratory testing. Severe HTN (SBP ≥ 160mmHg or DBP ≥ 100mmHg) should be treated to prevent maternal vascular complications such as stroke, and commonly prescribed agents include hydralazine, labetalol, or calcium channel blockers. Fetuses of patients with severe PE are typically delivered regardless of gestational age to prevent further maternal and fetal complications. The HTN and proteinuria associated with PE often resolve within a few days postpartum but may last up to a few weeks.
CONGENITAL HEART DISEASEAtrial septal defects (ASD) are the most common congenital lesions seen during pregnancy and are usually tolerated well in the absence of pulmonary HTN or atrial tachyarrhythmias. Ventricular septal defects (VSD) are typically identified earlier in life and most large shunts are corrected before reaching childbearing age. Small shunts are generally well tolerated, but large VSDs are associated with increased risk of developing HF or pulmonary HTN, increasing the risk of maternal and fetal mortality. Eisenmenger syndrome (discussed below) can develop with large shunts and is associated with high maternal mortality rates.
Tetralogy of Fallot (TOF) is the commonest form of cyanotic heart disease in adults; most pregnant women who present with TOF will have undergone surgical correction and do well throughout pregnancy and delivery. If uncorrected, the decreased peripheral vascular resistance associated with pregnancy may increase right to left shunting. Cyanosis, when present, is associated with erythrocytosis, hyperviscosity, and thromboemboli, increasing the risk of maternal cardiovascular complications.22 Symptoms in patients without correction are typically dependent on VSD size, degree of pulmonic stenosis, and right ventricular hypertrophy. Hemoglobin levels ≥20 gm/dl and arterial oxygen saturation ≤85% are associated with poor fetal outcomes and should be avoided.23 Women who have undergone operative repair may have residual pulmonic or tricuspid insufficiency and right ventricular dysfunction which may be worsened by the hypervolemia that accompanies pregnancy.
PULMONARY HYPERTENSIONPulmonary HTN is associated with high mortality during pregnancy regardless of the etiology and patients should be strongly discouraged from becoming pregnant. Causes include primary pulmonary HTN, chronic thromboembolic disease, or secondary pulmonary HTN from valvular heart disease or congenital intracardiac shunts (Eisenmenger syndrome). Eisenmenger syndrome can occur in the setting of large unrepaired left to right shunts when pulmonary vascular changes occur in response to increased pulmonary blood flow leading to increased pulmonary vascular resistance and ultimately shunt reversal in these patients. This can be observed in patients with ASDs, VSDs, or a patent ductus arteriosus and is associated with high maternal (40%) and fetal mortality (8%).24 The hemodynamic changes associated with labor and delivery as well as during the puerperium are poorly tolerated and the majority of maternal deaths are due to hypovolemia, thromboembolic events, or cesarean delivery; most occur during or within the first week after delivery.25 Termination of pregnancy should be considered in patients with severe pulmonary HTN or Eisenmenger syndrome.
MARFAN SYNDROMEMarfan syndrome is an autosomal dominant disorder involving multiple organ systems and is associated with significant cardiovascular, musculoskeletal, and ocular complications. Most patients with Marfan syndrome have a mutation in the fibrillin-1 gene, a major component of microfibrils which have a load bearing role in elastic arteries such as the aorta. The hypervolemia, tachycardia, and increased stroke volume and cardiac output associated with pregnancy increase aortic wall tension and shear stress. Aortic dilation, aortic insufficiency, and aortic dissections are major causes of morbidity and mortality in patients with Marfan syndrome, and the diagnosis and treatment of these patients is aimed at preventing these complications. Mitral valve prolapse with or without regurgitation is another associated cardiovascular complication of Marfan syndrome. Women with a history or suspicion of Marfan syndrome should be evaluated with an echocardiogram to assess aortic root diameter in addition to serial clinical assessments. Beta blockers are used to slow aortic dilatation and aortic insufficiency and may improve survival in patients with Marfan syndrome.26 Pregnancy is usually contraindicated when the aortic root diameter exceeds 4cm, but the risk of major adverse cardiovascular complications appears to be low with aortic root diameters less than 4cm.27 Monthly or bimonthly echocardiography examinations are recommended in all pregnant women with aortic root or ascending aortic dilatation and these women should deliver at hospitals where cardiothoracic surgery is available.28 It may be reasonable to prophylactically replace the aortic root and ascending aorta in patients with aortic root diameters >4cm who are contemplating pregnancy. Patients should also be counseled about the heritable nature of Marfan syndrome as it is an autosomal dominant disorder.
CONCLUSIONSImprovements in diagnosis and treatment of patients with congenital heart disease along with an increasing number of women delaying pregnancy until later ages have increased the incidence of women at risk for cardiovascular complications during pregnancy. Several factors associated with increased maternal and fetal complications during pregnancy have been identified and include poor functional class (NYHA class III-IV) or cyanosis, history of previous cardiac events or arrhythmias, LV obstruction (moderate to severe MS or AS), and reduced LV systolic function (LVEF ≤40%). Patients with certain high-risk features such as pulmonary HTN, Marfan syndrome with aortic dilatation, or severely reduced LV systolic function should be counseled against becoming pregnant. Patients should be counseled on obtaining adequate rest, and correctable conditions such as anemia should be treated. Vaginal delivery usually carries the lowest risk of complications in most cardiac conditions but caesarean delivery may be indicated in women with certain conditions or with prolonged or difficult labor. To optimize outcomes in pregnant women with underlying cardiac disease, patients should be evaluated and monitored with a “team” approach by both an obstetrician and cardiologist.
CONFLICT OF INTERESTNone declared.
.
Received 14 July 2011
Accepted 16 July 2011
Corresponding author: Department of Physiology and Biophysics, University of Mississippi Medical Center, 2500 North State Street, Jackson, MS 39216-4505, United States. jgranger@umc.edu