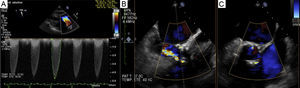
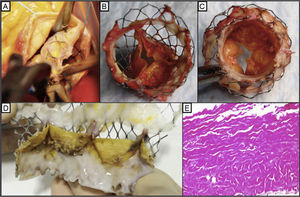
A 58-year-old man with cirrhosis (Child A6) had severe symptomatic stenosis of a bicuspid aortic valve. The multidisciplinary Heart Team decided on treatment by percutaneous aortic valve implantation (29-mm CoreValve, femoral approach), which was successfully carried out, with no complications. Following the procedure, the patient was asymptomatic and transprosthetic pressure gradients were stable. The cirrhosis was stabilized by abstinence from alcohol consumption, optimized medical treatment, and elimination of esophageal varices by band ligation. Five years later, the patient was hospitalized for dyspnea. Transthoracic echocardiography showed elevated maximum and mean transvalvular gradients (87.7/50.6mmHg), with severe aortic regurgitation (Figure 1A). Transesophageal echocardiography (TEE) confirmed degeneration of the prosthesis, with severe stenosis due to commissural fusion of 2 leaflets, and significant mixed intraprosthetic and periprosthetic regurgitation (Figure 1B and Figure 1C). There were no lesions on coronary angiography. Computed tomography confirmed commissural fusion with no thickening of the leaflets. Based on the patient's stabilized hepatic condition (Child A2) and periprosthetic regurgitation, we selected surgical treatment. Following debridement and detachment, the prosthetic valve was removed (Figure 2A) and a biological valve was implanted, with no complications.
The explanted valve showed neoendothelialization, with complete commissural fusion of 2 leaflets and incipient fusion of the other 2 commissures, as well as calcified nodules, predominantly on the ventricular side of the valve (Figure 2B, Figure 2C, Figure 2D). On microscopic evaluation, the valvular leaflets showed destructuration of the collagen fibrillar bundles, with myxoid degenerative changes and dystrophic calcifications, and no inflammation (Figure 2E).
This is the first case in our setting of late degeneration of a self-expanding aortic valve that was surgically removed.
CONFLICTS OF INTERESTC. Morís is a CoreValve proctor.