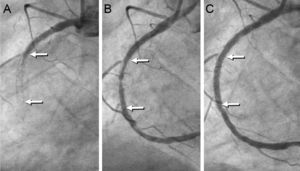
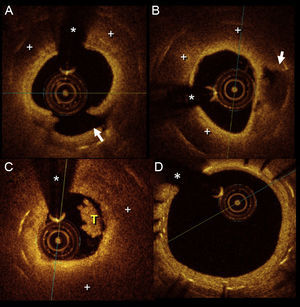
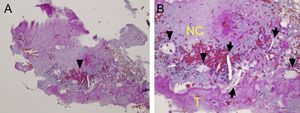
Previous pathological reports have described in-stent neoatherosclerosis as a new underlying pathological substrate to late thrombotic events. A 63-year-old man, who had undergone implantation of a drug-eluting stent in the midright coronary artery 2 years previously, presented with an inferior ST-segment elevation myocardial infarction. Emergent coronary angiography revealed stent thrombosis at the right coronary artery (Figure 1A, arrow). Thromboaspiration retrieved abundant material and obtained a normal anterograde coronary flow (Figure 1B). Subsequently, the artery was treated with balloon angioplasty with a good angiographic result (Figure 1C). Optical coherence tomography (Figure 2) was performed immediately after thromboaspiration and disclosed the presence of neoatherosclerosis, consisting of a large lipid areas (+) obscuring most of the underlying stent struts and a large cap rupture (Figure 2A). A glistening neointima covering the lipid pools (+) and a plaque cavity (arrow) originating from the adjacent ruptured cap was also observed (Figure 2B). A white thrombus (T) is readily depicted in the lumen (Figure 2C); (*) denotes wire artifact. There was also mild neointimal proliferation at the edge of the stent (Figure 2D). Intracoronary specimens obtained after aspiration were examined histopathologically with Masson's trichrome staining (Figure 3A; 20 x). The retrieved tissue at higher magnification (Figure 3B: 40 x) consisted of thrombus (T), cholesterol crystals (arrows), lipid-laden, foamy, macrophages (arrowheads) and a large necrotic core (NC), the hallmark of in-stent neoatherosclerosis.
This case illustrates in vivo the close correlation between intracoronary imaging and the corresponding pathological substrate in a patient with in-stent neoatherosclerosis complicated by atherosclerotic plaque rupture leading to very late stent thrombosis.